Manuscript accepted on :27-08-2025
Published online on: 16-09-2025
Plagiarism Check: Yes
Reviewed by: Dr. Gowri Burle
Second Review by: Dr. Mohammed Ahmed
Final Approval by: Dr. Anton R Keslav
Siti Nor Aqilah Mohd Noor1 , Shazia Jamshed2
, Shazia Jamshed2 , Chiau Ming Long3
, Chiau Ming Long3 , Umar Idris Ibrahim1
, Umar Idris Ibrahim1 , Ahmad Kamal Ariffin Abdul Jamil1
, Ahmad Kamal Ariffin Abdul Jamil1 , Nurulumi Ahmad1
, Nurulumi Ahmad1 , Aslinda Jamil1
, Aslinda Jamil1 , Kheng Seang Lim4
, Kheng Seang Lim4 and Pei Lin Lua1*
and Pei Lin Lua1*
1Faculty of Pharmacy, Universiti Sultan Zainal Abidin (UniSZA), Terengganu, Malaysia
2School of Pharmacy, International Medical University (IMU), Kuala Lumpur, Malaysia
3School of Medical and Life Sciences, Sunway University, Selangor, Malaysia
4Faculty of Medicine, University of Malaya, Kuala Lumpur, Malaysia
Corresponding Author E-mail:peilinlua@unisza.edu.my
DOI : https://dx.doi.org/10.13005/bpj/3260
Abstract
This study aimed to explore the perceptions and clinical experiences of Indian traditional medicine, Ayurveda practitioners in Malaysia regarding the use of complementary and alternative medicine (CAM) in the treatment of epilepsy. An exploratory qualitative design was employed. In-depth face-to-face interviews were conducted with purposively sampled Ayurveda practitioners (n=8; 5 males and 3 females; mean age = 45.1 ± 8.3 years) with a minimum of 5 years of clinical experience specifically in managing patients with epilepsy using CAM approaches. A semi-structured topic guide explored their diagnostic approaches, treatment practices, perceived effectiveness, and professional interactions. Interviews were audio-recorded, transcribed verbatim, and analysed thematically using an inductive approach. Five major themes were identified: (1) perceived value and limitations of CAM, (2) therapeutic relationship and communication, (3) individualized treatment and clinical decision-making, (4) integration with other health systems, and (5) impact on patient outcomes. Practitioners highlighted Ayurvedic medicines' holistic character, relaxing and purifying properties, and few side effects. Treatments were tailored to pulse diagnosis, patient behaviour, and physical and psychological features. Patient care was said to require trust and emotional rapport, participants said. Some reported growing acceptance from biomedical experts'. Reduced seizure frequency, emotional stability, and quality of life, especially in youngsters, were frequently mentioned as positive outcomes. Ayurveda practitioners view CAM as a flexible, patient-centered supplement to traditional therapy. Epilepsy care requires personalisation, therapeutic alliance, and cultural relevance, according to their findings. These findings suggest exploring integrative care approaches that incorporate traditional healing practices in culturally varied environments.
Keywords
Apasmara; Ayurveda; Alternative medicine; Complementary; Epilepsy; Perceptions; Practitioner
Download this article as:| Copy the following to cite this article: Noor S. N. A. M, Jamshed S, Long C. M, Ibrahim U. I, Jamil A. K. A. A, Ahmad N, Jamil A, Lim K. S, Lua P. L. Perceptions and Experiences of Indian Traditional Medicine Practitioners in Managing Epilepsy: A Qualitative Study in Malaysia. Biomed Pharmacol J 2025;18(3). |
| Copy the following to cite this URL: Noor S. N. A. M, Jamshed S, Long C. M, Ibrahim U. I, Jamil A. K. A. A, Ahmad N, Jamil A, Lim K. S, Lua P. L. Perceptions and Experiences of Indian Traditional Medicine Practitioners in Managing Epilepsy: A Qualitative Study in Malaysia. Biomed Pharmacol J 2025;18(3). Available from: https://bit.ly/4nwcAVR |
Introduction
Epilepsy, impacting approximately 70 million individuals globally, is a common neurological disorder that often leads to chronic disability, psychological distress, and social stigma.1 Approximately thirty percent of patients experience drug-resistant epilepsy (DRE), characterised by persistent seizures despite adequate pharmacological intervention and the availability of many antiepileptic drugs (AEDs).2,3 This therapeutic break down has prompted numerous individuals and families to seek alternative therapy choices, especially traditional medical systems with enduring cultural and clinical significance. It is estimated that globally, 7.5 – 73.3% of individuals with epilepsy utilise CAM approaches, highlighting a significant patient demand that reflects the experiences reported in our study.14
Ayurveda, particularly Siddha, offers a distinctive and comprehensive approach to the treatment of epilepsy in South Asia.4-6 Ayurvedic knowledge characterises epilepsy as Apasmara—a chronic, relapsing disorder associated with disturbances in memory, consciousness, and mental equilibrium, believed to arise from imbalances in the body’s elemental forces (doshas) and mental states (gunas).6-8
Standard therapy modalities include mind-body interventions (satvavajaya chikitsa), lifestyle alterations, detoxification procedures (shodhana), and the application of specific herbal treatments. Historically utilised for their neuroprotective and anticonvulsant properties, botanicals such as Brahmi (Bacopa monnieri), Jatamamsi (Nardostachys jatamansi), and Ashwagandha (Withania somnifera) are now corroborated by preclinical evidence.9,10 Diagnosis and treatment are frequently customised according to individual constitution (prakriti), pulse assessment, behavioural observation, and lifestyle factors.11
In addition to biological factors, Indian traditional medicine underscores the significance of the therapeutic connection, emotional support, and carer participation as essential components of recovery.12,13 The relational dynamics are crucial to the CAM experience and frequently cited as factors contributing to patient satisfaction and long-term adherence.14,15 However, CAM is not an unified entity; variations in the types of practices utilised, simultaneous administration of AEDs, and the particular type of epilepsy may all affect patient reactions and overall efficacy.16,17
Although these systems are quite prevalent in India and among diaspora populations, there is a paucity of empirical research examining the clinical perspectives and personal experiences of traditional practitioners managing epilepsy. The majority of current study emphasise the role of traditional medicine practitioners in providing CAM, yet there is limited insight into traditional healers’ perceptions of epilepsy, their therapeutic approaches, and their interactions with biomedical institutions. This study aims to address this gap by examining how practitioners of Indian traditional medicine understand and manage epilepsy. This research aims to elucidate clinical reasoning, therapeutic approaches, and perceived roles within the broader healthcare context through a qualitative examination of their perspectives.
Materials and Methods
Study design and setting
This qualitative study adopted a thematic analysis orientation, implemented an exploratory approach utilizing in-depth face-to-face interviews to explore the perceptions and clinical experiences of Indian traditional medicine (Ayurveda) practitioners regarding the use of CAM in the treatment of epilepsy. Ethical permission was obtained from the Universiti Sultan Zainal Abidin, UniSZA Human Research Ethics Committee (UHREC) [Reference number: UniSZA/UHREC/2022/439], and the study was also registered and approved by the National Medical Research Register (NMRR), Ministry of Health Malaysia [NMRR ID: 23-01207-PS8 (IIR)].
Participants
A purposive sampling technique was employed to ensure participants had relevant expertise with CAM modalities in Ayurveda. Participants were recruited via a Google Form titled ‘Healthcare Providers’ Opinion on CAM Use in Epilepsy Patients,’ which screened for eligibility and practice factors. All practitioners who completed the form agreed to participate, and no refusals or dropouts occurred. Maximum variation sampling was performed to include varied ethnic and practice backgrounds. Sampling continued until data saturation was reached, defined as the point when no new codes or themes emerged during analysis. All interviews were conducted between the researcher and the participant in a private setting, and no other individuals were present during the sessions.
Procedure and Interview Process
Face-to-face, in-depth interviews were conducted by three members of the research team, all with advanced academic qualifications in pharmacy and prior experience in qualitative research. A semi-structured topic guide consisting of nine open-ended questions was used. These questions explored areas such as the perceived benefits and limitations of CAM, challenges in its use, practitioner–patient communication, collaboration with other professionals, personalization of treatments, and approaches to diagnosis and treatment. The guide was developed based on prior literature and validated by five experts in the pharmacy field for relevance and clarity.18-20 The questionnaire guide was prepared only in English, and no local language translation was produced. To ensure methodological rigor, the interviewers’ expertise in qualitative methods guided the sessions, with additional support from a trained research assistant.
Participants were given an information sheet and provided written informed consent before the interview. A short ice-breaker was included to establish rapport. Interviews, conducted over three months, lasted 25 to 45 minutes, were held in private settings (clinics and workplaces), audio-recorded with participant permission, and supported by field notes. While English was the major language utilized, participants were permitted to respond in Bahasa Melayu or English, with real-time translation provided by the research assistant as appropriate. All interviews were recorded verbatim and anonymised for confidentiality.
Data Analysis
This method encompassed several critical stages: data familiarization, open coding, categorization of codes into overarching themes, and the formulation of final themes and subthemes.21All coding and theme development were performed manually by the researcher using printed transcripts and structured coding sheets, in line with Braun & Clarke’s six-phase framework for thematic analysis. The researcher did the coding, which was subsequently verified by a secondary researcher to strengthen the legitimacy and consistency of the findings. Disputes over coding or theme development were settled by dialogue and consensus. Field notes were utilized to enhance contextual comprehension and interpretation of the data. To ensure trustworthiness and rigor, the study followed to Guba and Lincoln’s standards for qualitative research in generating credibility, transferability, dependability, and confirmability.22 A flowchart detailing the study procedure is provided in Figure 1.
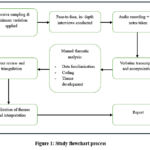 |
Figure 1: Study flowchart processClick here to view Figure |
Results
Eight Ayurveda practitioners participated in the study, achieving data saturation within this cohort. All interviews were conducted in person using a semi-structured guide. The participants included both male and female practitioners from Indian ethnic backgrounds, each with clinical experience ranging from 6 to 15 years in managing epilepsy with CAM. Table 1 summarizes participant demographics.
Table 1: Demographics of the respondents
| Characteristic | Description |
| Total number of respondents | 8 (P1-P8) |
| Experience (years) | 5 – 15 |
| GenderMale
Female |
5 3 |
| Age (mean ± SD)Workplace
Urban |
45.1 ± 8.3 years8 |
*P1-P8: Participant 1 – Participant 8
Five main themes were identified, each with related sub-themes: (1) perceived value and limitations of CAM in epilepsy care, (2) therapeutic relationships and communication with patients, (3) individualized treatment and clinical decision-making, (4) integration with other healthcare systems, and (5) perceived impact on patients and families. These themes reflect the complex and holistic nature of Ayurvedic epilepsy care as practiced in the Malaysian context. Table 2 illustrates the themes.
Table 2: Emerged themes from thematic analysis
| No | Themes | SUB-THEMES |
| 1 | Perceived Value and Limitations of CAM | · Holistic Benefits with Fewer Side Effects· Limitations in Specific Epilepsy Types
· Systemic and Regulatory Constraints |
| 2 | Therapeutic relationships and Communication with Patient | · Trust-Building and Emotional Rapport· Two-Way Communication and Continuous Feedback
· Social Reintegration and Emotional Support |
| 3 | Individualized Treatment and Clinical Decision-Making | · Personalized Assessment and Dosage Adjustment· Diagnostic Tools and Observational Skills
· Stepwise Therapeutic Philosophy · Specific Herbal Formulations and Delivery Methods |
| 4 | Integration with other Healthcare Systems | · Increasing Biomedical Referrals· Peer Collaboration and Learning Platforms |
| 5 | Perceived Impact on Patients and Families | · Clinical Improvements and Reduced Seizure Frequency· Holistic Improvement and Quality of Life
· Empowerment and Adherence |
Theme 1: Perceived Value and Limitations of CAM in Epilepsy Care
Ayurveda practitioners emphasized that CAM treatments offered a holistic, gentle, and long-term approach for managing epilepsy. They believed CAM could calm neurological disturbances without the harsh side effects often associated with conventional antiepileptic drugs. However, they also recognized clear limitations when treating severe or structurally based epilepsy, and they described systemic barriers such as legal restrictions on herbal medicine use.
Holistic Benefits with Fewer Side Effects
CAM was seen as non-invasive and restorative, particularly suitable for children or stress-related epilepsy cases. Calming therapies, dietary changes, and the use of medicated ghee were core strategies believed to stabilize the nervous system gently.
“Seizures… due to dysfunction of the brain cells… we calm them down. But calming is not only with medicine but it involves body detox, stress relief, and family support as well.” – P7
“Ghee plays a very very important role… it crosses the blood-brain barrier. That’s why we process it with herbs so it acts like a carrier to deliver compounds to the brain and reduce seizure reactivity.” – P6
“CAM gives a calming effect without the heaviness of allopathic side effects. The patient feels light, not drowsy. That’s the difference we see.” – P4
Limitations in Specific Epilepsy Types
Participants acknowledged that not all epilepsy types respond equally to Ayurvedic therapies. In particular, conditions with congenital or degenerative origins were described as harder to treat or not curable with CAM alone.
“Some types of epilepsy like sannipata cannot be treated. These are very complex neurological, mental, and physical imbalances all together …. sometimes the patient’s structure is beyond healing.” – P5
“There are patients with long-standing seizure history or genetic involvement, but Ayurveda can help, but we can’t reverse the brain damage. They remain stable, but not fully seizure-free.” – P7
Systemic and Regulatory Constraints
Legal limits on Ayurvedic products and lack of access to essential herbs restricted their treatment scope. Moreover, the absence of a psychological framework within some CAM models was identified as a gap.
“No holistic approach psychologically… that’s the biggest backdrop. We only focus on medicine, but emotional and lifestyle factors are huge in epilepsy.” – P2
“Limited access… because certain herbs not allowed. We can’t do full treatment sometimes due to import laws or bans.” – P3
Theme 2: Therapeutic Relationship and Communication with Patients
Practitioners highlighted the deeply relational nature of their work. Building trust with patients and families was not only central to diagnosis and treatment, but seen as therapeutic in itself. Communication was described as ongoing, two-way, and emotionally engaged.
Trust-Building and Emotional Rapport
Trust emerged as a fundamental cornerstone of the therapeutic interaction. Practitioners emphasised that emotional safety, empathy, and mutual understanding must be created prior to effective treatment. This trust was influenced by personal experiences, enhancing their awareness of patients’ needs. One practitioner shared her experience treating her own child with epilepsy, underscoring the personal commitment involved.
“My son… has seizures since 8 months old… I try to keep him calm. I’ve lived this as a mother and a practitioner. I know what calmness, confidence, and a peaceful home can do.” – P7
Two-Way Communication and Continuous Feedback
Therapeutic relationships were sustained through regular follow-up, text-based updates from caregivers, and open dialogue about treatment effects and lifestyle changes.
“Communication will be two-way. We don’t just give medicine and wait. Parents message us, and we keep seizure records, every episode is tracked and analysed month by month.” – P2
“Even small changes like headache or stress, families inform us so we can adjust the treatment. It’s a cycle of sharing, not just us prescribing to the patient.” – P4
“We need updates from the patient to change medicine. If the seizure happens, how, when, what triggered it … we record all that regularly.” – P5
Social Reintegration and Emotional Support
Beyond seizure control, practitioners aimed to restore confidence, independence, and social functioning in their patients.
“Helping patients build confidence to reintegrate into society… is as important as stopping seizures. Many patients come feeling excluded or ashamed.” – P5
“They start going back to school, making friends. With Ayurveda, it’s not only seizure control but it’s giving them a chance to feel normal again.” – P6
Theme 3: Individualized Treatment and Clinical Decision-Making
Ayurvedic practice was highly personalized. Diagnosis and treatment were tailored based on patient-specific factors such as pulse, digestion, age, symptoms, and emotional state. Therapies included herbal preparations, oils, and detox regimens administered in a stage-wise manner.
Personalized Assessment and Dosage Adjustment
Treatment protocols were described as unique to each patient, adapted according to age, severity, and digestive strength. Adjustments were made over time as patient needs evolved.
“No two treatments are the same. Even for the same epilepsy type, the dosage, herbs, and method change depending on digestion, mental state, and patient cooperation.” – P6
“Treatment changes depending on age and severity. For children we go gentler, for adults more stabilising. It’s not copy-paste treatment.” – P8
“Some patients need more support for mental symptoms, others for physical heat. The combination is made specific to them.” – P5
Diagnostic Tools and Observational Skills
Practitioners relied on traditional diagnostic techniques such as pulse reading, as well as non-verbal cues including body language and energy levels.
“We make decisions based on pulse diagnosis, symptoms, and epilepsy type. But also on how they speak, how they walk …. it’s all part of the diagnosis.” – P5
“Diagnosis starts from how the person walks into the room. The posture tells you a lot, even their speech rhythm and tone give signals.” – P6
Stepwise Therapeutic Philosophy
Treatment often began with detoxification, followed by calming therapies and then strengthening remedies. This approach was said to align with the body’s natural rhythms.
“Sometimes just detox makes a huge difference. Once the body is cleaned, the calming herbs work better. This order matters.” – P4
“It’s like peeling layers where first remove the toxins, then rebuild the strength. That’s why the patient must commit to the full process.” – P6
Specific Herbal Formulations and Delivery Methods
Practitioners used herbs like Brahmi, Jatamamsi, Manjishta, and Shankhpushpi, often administered in ghee, capsule, or decoction form. These were selected for their brain-calming and circulatory properties.
“Herbs like Brahmi, Jatamamsi, Kapikacchu… cross the blood-brain barrier. That’s why we use ghee or oil to prepare the formula which it helps delivery to the nervous system.” – P5
“Manjishta and Shankhpushpi used in tablet form …. also oil-based decoctions for absorption through skin or nasal route.” – P7
Theme 4: Integration and Collaboration with Other Health Systems
Participants described a gradual shift toward more collaborative care, particularly as some modern doctors began recognizing the value of CAM therapies. Peer learning and CME events also supported shared knowledge.
Increasing Biomedical Referrals
Some reported that allopathic doctors referred patients for complementary care, particularly for patients dissatisfied with drug-based regimens.
“Modern doctors are referring patients now. Especially those who don’t respond to AEDs or those who want to avoid side effects.” – P1
“Sometimes neurologists send their parents or children to us when they want a drugless alternative. That’s new but growing.” – P3
Peer Collaboration and Learning Platforms
Traditional practitioners reported a strong sense of collegiality with other Ayurveda providers, especially through continuing medical education (CME) events in India.
“Interaction mainly via CME in India. We attend conferences and share with other traditional practitioners.” – P5
“We align with traditional practitioners using oil-based treatments. It’s a shared heritage, but we learn from each other too.” – P6
Theme 5: Impact of CAM Treatment on Patients and Families
Participants shared several success stories and noted improvements across physical, emotional, and social domains. Children especially showed promising outcomes with lifestyle changes and consistent Ayurvedic care.
Clinical Improvements and Reduced Seizure Frequency
Many practitioners reported lower seizure frequency and increased seizure-free periods in their patients following treatment.
“Child… from monthly seizures to once a year. That’s not magic but it’s from strict diet, calm living, and consistency.” – P1
“Adults… episode frequency reduced. But it takes patience. People want instant cure, we give progressive healing.” – P2
“We’ve seen even drug-resistant cases come under control after long-term Ayurveda with commitment.” – P4
Holistic Improvement and Quality of Life
Patients were said to experience overall better emotional regulation, digestion, and mental clarity. Family members frequently noted these changes in their children, indicating favourable patient-centered outcomes.
“60 to 70% feel better overall holistically which help them have better digestion, better sleep, better mood.” – P6
“Some patients showed up to 50% improvement. Some patients noted that not just seizures, but school, work, social life also improved.” – P5
“Parents tell us their children sleep better, talk more, and feel less anxious. That’s success too.” – P7
Empowerment and Adherence
When patients trusted their practitioners and felt emotionally supported, their adherence improved and so did outcomes. CAM was seen as empowering patients to co-manage their care.
“The best medicine… is the patient. We can only guide; they must walk the healing path.” – P1
“Diet, behaviour, trust … all contributed. That’s the triangle that keeps epilepsy stable in most patients we see.” – P3
“When the family follows advice sincerely, the results show. That’s why education and emotional support are part of treatment.” – P4
Discussion
This study provides an in-depth understanding of how Ayurvedic practitioners view and manage epilepsy. Their narratives reflect a holistic clinical perspective, perceiving epilepsy not solely as a neurological problem, but as a multifaceted affliction stemming from imbalances in physical, emotional, and spiritual realms. This perspective is fundamentally based on Ayurvedic knowledge, namely regarding epilepsy as Apasmara, where disturbances in memory, consciousness, and the three doshas (vata, pitta, kapha) are considered central to its pathophysiology.4,7-9
Participants in this study highlighted individualised evaluation and pulse-based diagnosis, aligning with Ayurveda’s constitutional methodology. These findings have been confirmed by clinical evaluations that illustrate how treatment is customised according to the patient’s lifestyle, psychosocial context, and constitutional type (prakriti).9,11 This context-specific care is facilitated by therapies that include purgatives, nasal administration, and oil-based external treatments such as shirodhara and abhyanga. These therapies, however historical, are currently being re-examined in integrative neuroscience for their influence on the autonomic nervous system.5,8,23
Additional, participants identified a therapeutic arsenal of many herbs that are well-documented in both traditional and contemporary pharmacology. Brahmi (Bacopa monnieri), Kapikacchu (Mucuna pruriens), Jatamamsi (Nardostachys jatamansi), and Shankhpushpi (Convolvulus pluricaulis) are often referenced for their contributions to soothing the nervous system, augmenting cognitive performance, and promoting neuroplasticity.() These herbs have exhibited anticonvulsant, antioxidant, and GABAergic modifying activities in preclinical and pharmacological investigations.9,10,24,25 Similarly, preparations like Ashwagandharishta, Brahmi ghrita, and Saraswatarishta have been linked to decreased seizure frequency and mood stabilisation.4,5,8,26
Participants noted that ghee-based formulations were not just traditional but also provided a biological function by facilitating the transport of lipophilic substances across the blood-brain barrier, hence increasing brain delivery. This justification is progressively supported by pharmacological research affirming the role of ghee as a carrier in medication absorption and central nervous system targeting.4,5 Additionally, network pharmacology research have revealed several drug-like phytochemicals in these plants that act synergistically on epilepsy-related targets.27
Regardless these proven advantages, participants recognised the constraints of CAM in addressing epilepsy with structural causes or irreversible neural impairment. This aligns with clinical data indicating that CAM therapies are more effective as complimentary interventions rather than as independent treatments for certain epilepsy subtypes.9,11 Furthermore, regulatory obstacles including limited herb accessibility, absence of standardisation, and inadequate policy support were identified as impediments, corroborating conclusions from international CAM policy assessments.13,14 Epidemiological data indicate that 20–40% of epilepsy patients remain DRE, with many actively seeking CAM as supplemental methods, underscoring the clinical significance of these methods of treatment.28,29,30,31
A significant topic in the participants’ accounts was the therapeutic interaction. Practitioners perceived healing as profoundly relational, encompassing emotional support, trust cultivation, and sustained contact with patients and carers. This reflects the Ayurvedic concept of Satvavajaya chikitsa, which employs mental, behavioural, and spiritual therapies to achieve equilibrium.8,12 These relational dynamics elucidate why numerous patients resort to complementary and alternative medicine after perceiving biological therapy as overly impersonal or inadequately responsive to psychosocial distress.13,15
Participants also reported enhanced inter-systemic collaboration. Some have observed that contemporary physicians are directing patients, particularly those with DRE or pursuing non-pharmacological alternatives. These experiences correspond with the integrative care models developing in India, where official and informal referrals between CAM and biomedical practitioners are increasingly prevalent.12,32 Nonetheless, these connections are constrained by structural deficiencies in training, research translation, and regulatory integration.14
The results reported by practitioners decreased seizure frequency, enhanced emotional resilience, and improved quality of life are corroborated by recent studies on yoga, dietary changes, and Ayurvedic treatments.11,21,33 Significantly, patients were characterised not as passive recipients but as active collaborators in their healing process. CAM practitioners underscored the importance of behavioural discipline, familial involvement, and compliance with daily routines as essential for sustained enhancement. This empowerment-oriented methodology is reflected in research about patient adherence and desire for CAM, especially in culturally rooted contexts such as India and Malaysia.14,15
Conclusion
This study offers insights into the clinical experiences and perspectives of practitioners of Indian traditional medicine (Ayurveda) in the management of epilepsy in Malaysia. The findings highlight the significance of CAM as a holistic, personalised, and culturally integrated approach to care. Practitioners highlighted the significance of emotional rapport, personalised diagnosis, and the therapeutic application of herbal and oil-based formulations in the management of seizure-related symptoms. In alongside reducing symptoms, the use of CAM was seen as beneficial in decreasing seizure frequency, enhancing emotional stability, and improving quality of life, highlighting its potential as a complementary approach in the management of epilepsy.
Despite existing limitations, especially regarding the treatment of structurally based epilepsies and regulatory challenges, participants conveyed a sense of optimism regarding collaboration with biomedical professionals and a rising patient interest in integrative solutions. Meaningful outcomes were reported, including a reduction in seizure frequency, enhancement of emotional well-being, and an improved quality of life, especially in children.
The findings underscore the necessity for inclusive health policies that acknowledge the significance of traditional systems such as Ayurveda. It is advisable to conduct additional research with larger and more diverse populations of practitioners and patients to investigate integration pathways, safety regulations, and long-term outcome monitoring.
This study enhances the understanding of epilepsy management in traditional healing systems, providing implications for culturally competent, patient-centred care in pluralistic health systems.
Acknowledgement
We would like to express our gratitude to the Director-General of Health Malaysia for granting permission to publish this article. We also appreciate all the peers who helped with the writing process of this manuscript, including Dr. Nurul Afiedia Roslim, Ms. Siti Maisarah Mohd Noor, and Ms. Nur Kamilah Mohd Fauzy.
Funding Source
This project has been funded by the Ministry of Higher Education Malaysia under the Fundamental Research Grant Scheme (grant number: FRGS/1/2022/SS0/UNISZA/01/1).
Conflict of Interest
The author(s) do not have any conflict of interest.
Data Availability
This statement does not apply to this article
Ethics Statement
Ethical approval was obtained from the UniSZA Human Research Ethics Committee (UHREC) (reference code: UniSZA/UHREC/20220439) and Medical Research and Ethics Committee (MREC), Ministry of Health (MoH) Malaysia (reference code: ID-23-01207-PS8 (IIR)).
Informed Consent Statement
Written informed consent was obtained from all participants at the beginning of the study.
Clinical Trial Registration
This research does not involve any clinical trials.
Permission to reproduce material from other sources
Not applicable.
Authors’ Contribution
- Siti Nor Aqilah Mohd Noor: Data collection, Analysis, Conceptualization, Methodology, Writing – Original Draft.
- Shazia Jamshed: Data collection, Review & Editing
- Chiau Ming Long: Data collection, Review & Editing
- Umar Idris Ibrahim: Review & Editing
- Ahmad Kamal Ariffin Abdul Jamil: Review & Editing
- Nurulumi Ahmad: Review & Editing
- Aslinda Jamil: Review & Editing
- Kheng Seang Lim: Review & Editing
- Pei Lin Lua: Data collection, Analysis, Review, Visualization & Supervision
References
- Thijs RD, Surges R, O’Brien TJ, Sander JW. Epilepsy in adults. Lancet. 2019;393(10172):689-701.
CrossRef - Nagabushana D, S PK, Agadi JB. Impact of epilepsy and antiepileptic drugs on health and quality of life in Indian children. Epilepsy Behav. 2019;93:43-48.
CrossRef - Satishchandra P, Rathore C, Apte A, et al. Evaluation of one-year effectiveness of clobazam as an add-on therapy to anticonvulsant monotherapy in participants with epilepsy having uncontrolled seizure episodes: An Indian experience. Epilepsy Behav. 2022;130:108671.
CrossRef - Shanmugasundaram ER, Akbar GK, Shanmugasundaram KR. Brahmighritham, an Ayurvedic herbal formula for the control of epilepsy. J Ethnopharmacol. 1991;33(3):269-276.
CrossRef - Moon S, Raut N, Moon H, Dhawande A, Gurav S. Organoleptic, physicochemical, phytochemical and pharmacological evaluation of six medicated ghee used for Ayurvedic management of Epilepsy. J Ayurveda Integr Med. 2024;15(6):100995.
CrossRef - Babar RP, Gund SM, Kale AB. Concept of medicated ghee (Ghrita Kalpana) in the management of Childhood Epilepsy (Apasmara). ayurpub. 2017;II(1):347-349.
- Manyam BV. Epilepsy in ancient India. Epilepsia. 1992;33(3):473-475.
CrossRef - Adiga SH, Adiga RS, Bhat KMR, Upadhya D. Ayurveda therapy in the management of epilepsy. Epilepsy Behav. 2024;159:110026.
CrossRef - Sriranjini SJ, Sandhya K, Mamta VS. Ayurveda and botanical drugs for epilepsy: Current evidence and future prospects. Epilepsy Behav. 2015;52(Pt B):290-296.
CrossRef - Pandey MM, Katara A, Pandey G, Rastogi S, Rawat AK. An important Indian traditional drug of ayurveda jatamansi and its substitute bhootkeshi: chemical profiling and antioxidant activity. Evid Based Complement Alternat Med. 2013;2013:142517.
CrossRef - Chauhan P, Tantray J, Chauhan P, et al. A Comprehensive Review On Recent Advancement In Allopathy and Ayurveda In The Management Of Epilepsy. Int J Pharm Sci & Res. 2024;15(1):66-77.
- Khan A, Huerter V, Sheikh SM, Thiele EA. Treatments and perceptions of epilepsy in Kashmir and the United States: a cross-cultural analysis. Epilepsy Behav. 2004;5(4):580-586.
CrossRef - Niemi M, Ståhle G. The use of ayurvedic medicine in the context of health promotion–a mixed methods case study of an ayurvedic centre in Sweden.BMC Complement Altern Med. 2016;16:62. Published 2016 Feb 17. doi:10.1186/s12906-016-1042-z
CrossRef - Farrukh MJ, Makmor-Bakry M, Hatah E, Tan HJ. Use of complementary and alternative medicine and adherence to antiepileptic drug therapy among epilepsy patients: a systematic review. Patient Prefer Adherence. 2018;12:2111-2121.
CrossRef - Chabangu Q, Maputle MS, Lebese RT. Management of epilepsy through indigenous traditional and Western approaches in Africa: A systematic review. Health SA. 2022;27:1984.
CrossRef - Farrukh MJ, Makmor-Bakry M, Hatah E, Tan HJ. Medication adherence status among patients with neurological conditions and its association with quality of life.Saudi Pharm J. 2021;29(5):427-433. doi:10.1016/j.jsps.2021.04.003
CrossRef - Ernawati I, Islamiyah WR, Sumarno. How to Improve Clinical Outcome of Epileptic Seizure Control Based on Medication Adherence? A Literature Review.Open Access Maced J Med Sci. 2018;6(6):1174-1179. Published 2018 Jun 17. doi:10.3889/oamjms.2018.235
CrossRef - Bishop FL, Lewith GT. Who Uses CAM? A Narrative Review of Demographic Characteristics and Health Factors Associated with CAM Use. Evid Based Complement Alternat Med. 2010;7(1):11-28.
CrossRef - Pope C., Mays N. Qualitative research in health care. 3rd ed. London: BMJ Books; 2006.
CrossRef - Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349-357.
CrossRef - Braun V, Clarke V. Using thematic analysis in psychology.Qual Res Psychol. 2006;3(2):77-101.
CrossRef - Guba EG, Lincoln YS. Competing paradigms in qualitative research. In: Denzin NK, Lincoln YS, eds. Handbook of Qualitative Research. Thousand Oaks, CA: Sage; 1994:105–117.
- Saxena VS, Nadkarni VV. Nonpharmacological treatment of epilepsy. Ann Indian Acad Neurol. 2011;14(3):148-152.
CrossRef - Agarwa P, Sharma B, Fatima A, Jain SK. An update on Ayurvedic herb Convolvulus pluricaulis Choisy. Asian Pac J Trop Biomed. 2014;4(3):245-252.
CrossRef - Joshi VK, Joshi A. Rational use of Ashwagandha in Ayurveda (Traditional Indian Medicine) for health and healing. J Ethnopharmacol. 2021;276:114101.
CrossRef - Tanna IR, Aghera HB, Ashok BK, Chandola HM. Protective role of Ashwagandharishta and flax seed oil against maximal electroshock induced seizures in albino rats. Ayu. 2012;33(1):114-118.
CrossRef - Choudhary N, Singh V. Insights about multi-targeting and synergistic neuromodulators in Ayurvedic herbs against epilepsy: integrated computational studies on drug-target and protein-protein interaction networks. Sci Rep. 2019;9(1):10565.
CrossRef - Kwan P, Arzimanoglou A, Berg AT, et al. Definition of drug resistant epilepsy: consensus proposal by the ad hoc Task Force of the ILAE Commission on Therapeutic Strategies.Epilepsia. 2010;51(6):1069-1077. doi:10.1111/j.1528-1167.2009.02397.x
CrossRef - Löscher W, Klitgaard H, Twyman RE, Schmidt D. New avenues for anti-epileptic drug discovery and development.Nat Rev Drug Discov. 2013;12(10):757-776. doi:10.1038/nrd4126
CrossRef - Anzellotti F, Dono F, Evangelista G, et al. Psychogenic Non-epileptic Seizures and Pseudo-Refractory Epilepsy, a Management Challenge.Front Neurol. 2020;11:461. Published 2020 Jun 2. doi:10.3389/fneur.2020.00461
CrossRef - Al-Asmi A, Al Sabahi F, Al-Adawi S, et al. Complementary and Alternative Medicine for People with Epilepsy: Opinions of Physicians in Oman.Oman Med J. 2024;39(3):e629. Published 2024 May 30. doi:10.5001/omj.2024.70
CrossRef - Nono D, Gumisiriza N, Tumwine C, et al. Impact of COVID-19 on the well-being of children with epilepsy including nodding syndrome in Uganda: A qualitative study. Epilepsy Behav. 2023;138:108992.
CrossRef - Sharma S, Gulati S, Kalra V, Agarwala A, Kabra M. Seizure control and biochemical profile on the ketogenic diet in young children with refractory epilepsy–Indian experience. Seizure. 2009;18(6):446-449.
CrossRef







