Manuscript accepted on :19-04-2023
Published online on: 21-06-2023
Plagiarism Check: Yes
Reviewed by: Dr. Ankur Kumar Arya and Dr. Anjaneyulu Vinukonda
Second Review by: Dr. Karuna Priya Chitra karunakaran
Final Approval by: Dr. Eman Refaat Youness
Rahmi Annisa1* , Retno Susilowati2
, Retno Susilowati2 , Evika Sandi Savitri2
, Evika Sandi Savitri2 , Maharani Retna Duhita2
, Maharani Retna Duhita2 and Sharida Fakurazi3
and Sharida Fakurazi3
1Department of Pharmacy, Faculty of Medicine and Health Science, Universitas Islam Negeri Maulana Malik Ibrahim, Malang, Indonesia.
2Department of Biology, Faculty of Science and Technology, Universitas Islam Negeri Maulana Malik Ibrahim, Malang, Indonesia.
3Department of Human Anatomy, Faculty of Medicine and Health Sciences, Universiti Putra Malaysia, Serdang 43400, Selangor Darul Ehsan, Malaysia.
Corresponfing Author E-mail: rahmiannisa@farmasi.uin-malang.ac.id
DOI : https://dx.doi.org/10.13005/bpj/2647
Abstract
Film Forming Hydrogel is a dosage form that changes shape to film by solvent evaporation after being applied to the wound area. This study aims to present a study to develop film-forming hydrogels with a brief description of the membrane properties formulated from biopolymers for wound application. Over the last ten years, much effort has been conducted to develop new artificial polymeric membranes that meet the demanding requirements for topical applications such as skin wound care. Therefore, this study represents the ideal polymer specifications for wound dressing membranes, such as cross-linked hydrogels compatible with wound dressings. The results of the analysis showed that single-component hydrogels have low mechanical strength. Therefore, recent trends offer composite or hybrid hydrogel membranes to achieve a typical wound with various requirements to meet the characteristic aspects of film-forming hydrogels.
Keywords
Biomedical Applications; Film-Forming; Hydrogels; Membranes; Wound Dressings
Download this article as:| Copy the following to cite this article: Annisa R, Susilowati R, Savitri E. S, Duhita M. R, Fakurazi S. The Discovery of Drug Delivery from Development Film Forming Hydrogel for Wound Dressing Applications: A Systematic Review. Biomed Pharmacol J 2023;16(2). |
| Copy the following to cite this URL: Annisa R, Susilowati R, Savitri E. S, Duhita M. R, Fakurazi S. The Discovery of Drug Delivery from Development Film Forming Hydrogel for Wound Dressing Applications: A Systematic Review. Biomed Pharmacol J 2023;16(2). Available from: https://bit.ly/3XpwTZh |
Introduction
Hydrogel is a semisolid pharmaceutical preparation with a hydrophilic base. Hydrogels have the advantages of being easy to use and clean, and hydrogels also have intermolecular forces that can reduce the mobility of molecules and produce good viscosity. researchers in recent years many make hydrogel preparations because one of its uses can be medical 1.
The advantages include being easy to use and clean and having intermolecular forces that reduce molecular mobility and produce suitable viscosity 1. Recent studies have made many hydrogel preparations for medical purposes 2. Hydrogels are attractive candidates for biomedical development because they are hydrophilic, have good flexibility, and are sensitive to the physiological environment.
Hydrogels can expand and remove water reversibly and show stimuli in specific environments, such as temperature, pH, and ionic strength. Therefore, the good physiological response of the hydrogel to changes in physiological variables suggests its use in several biomedical applications. Hydrogel is often used in medicine as a wound healing agent observed the hydrogel contained PVA/chitosan/glycerol hydrogel prepared with irradiation followed by freeze-thawing, hydrogel application was successfully used as a dressing material in the medical treatment of burns and environmental injuries being wet can enhance the wound healing process 3. Several studies of the development trend of hydrogels as wound dressing membranes have been conducted using polymers and commercial products such as Geliperm, Curasol, and Tegagel. The following was discovered from the first attempt by biomaterial scientists to develop wound dressing hydrogels following the requirements for wound healing in the shortest time hydrogels generally control fluids and those lost from the body, maintain moisture in the damage, and have a network-like structure 4.
Cross-linking methods are commonly used to stabilize hydrogels by chemical or physical interactions between polymer chains, which helps to retain large amounts of absorbed water. In biomedical applications, physical or radiation cross-linking is preferred over chemical. This is because the physical method avoids the presence of agents, organic solvents, and chemical reagents and overcomes the toxicity problem. Therefore, techniques such as hydrogen, Van der Waals, or freeze-thawing (F-T) successive cycles are the safest for hydrogel formation. Thus, they are commonly used for wound dressings and in situ cross-linking cases 4.
Indonesia’s statistical data on the annual cost of wound healing in 2021 has increased significantly. Hence, conscious efforts have been made to reduce the management of wound care costs. Surprisingly, although polymer advances have shown promising potential and have existed in studies for decades, their understanding still needs to be improved, and the number of publications is relatively exclusive and scattered. Based on recent contributions, polyvinyl alcohol (PVA)-hybrid hydrogel membranes are considered the most frequent candidate for wound dressings 4. This study aims This study aims to present a study to develop film-forming hydrogels with a brief description of the membrane properties formulated from biopolymers for wound application. These modern dressing methods are recommended for covering and initiating healing efficiency and wound rates. This article is expected to provide an overview of optimizing the form of film forming hydrogels as wound dressings.
Material and methods
This study was conducted systematically using several databases, including a computer-based electronic search. The inclusion criteria include 2015 – 2021, the language of published literature in English or Indonesian, and study journals. Others include literature related to polymeric hydrogel membranes and wound dressing applications. The exclusion criteria are literature in journal reviews and literary texts, which cannot be accessed entirely. Furthermore, the literature used was discovered through an original study on the website, which included various databases that are easily accessible. International databases were obtained from ScienceDirect, Springer, PubMed, Sage, and Taylor & Francis Online. The keywords used include Film-forming, Hydrogels, Membranes, Wound dressings, and Biomedical Applications. A qualitative meta-synthesis approach was used for data analysis because the object representing data in the literature is heterogeneous. The Prisma Guideline diagram was used to collect relevant studies, and 13 were selected for a more detailed review. The strategy used in the review is shown in Figure 1.
 |
Figure 1: Review strategy scheme. |
Results and Discussion
Strategy for article selection and search after selecting a specific and systematic article search strategy using the PRISMA guideline method with four databases, namely ScienceDirect, Springer, PubMed, Sage, and Taylor & Francis Online. 13 research articles were relevant to the topic of discussion (Figure 1).
Hydrogels
Hydrogels are polymer networks that expand extensively, consisting of chains in which water is dispersed 5. It is also defined as the most common hydrogel as a network of water polymers that expand and are linked by a simple reaction of one or more monomers. The hydrogel criteria are divided into various classifications, including:
Classification based on polymer,
Classification based on the type of cross-linker,
category based on physical appearance,
Classification based on an electric charge,
variety based on configuration,
Classification based on natural and synthetic6.
The hydrogels are often used in medicine for wound healing. Furthermore, hydrogels from PVA/chitosan/glycerol, made by irradiation followed by freeze-thawing, have been successfully used as a dressing material in treating burns and wounds because a wet environment enhances the wound healing process 7.
The characteristics of Film Forming Hydrogel are expected to form films that are resistant to physiological stress caused by skin movement and maintain contact between the film and the skin for a long time. Optimal film forming must have benefits such as hydrogels, namely easy application, fast drying on the skin, proper hardness and adhesiveness, and film benefits such as good flexibility and elasticity. Film forming affects the wound healing mechanism. This is due to the normal pH conditions of human skin is pH 4-6; when an injury occurs, the surface pH becomes alkaline ranging from pH 7-8.9. Alkaline conditions will inhibit the healing process, so acidic conditions around the wound are needed to enhance the healing process. Acidic conditions will occur if film-forming preparations are made in an acidic pH range of around 5.5 ± 0.5 8.
Hydrogel is a three-dimensional polymer network with crosslinked hydrophilic polymers. It swells or stores water and physiological solutions up to a thousand times their dry weight and is also not readily soluble. They are insoluble in water due to cross-linking between polymer molecular chains, while their ability to absorb and expand water is due to functional groups such as -OH, -CONH, CONH2, and SO3H. Moreover, natural and synthetic hydrophilic absorb and retain large amounts of water 8.
Hydrogel bases can be made by chemical and physical cross-linking methods, as follows:
Chemical cross-linking
Using chemicals as cross-linking materials such as glutaraldehyde, formaldehyde, and others
Using radiation.
The formation of covalent bonds between different polymer chains results in chemical cross-linking. Furthermore, the use of chemicals will cause residues in the hydrogel. Therefore it is potentially toxic to patients. The radiation method also causes the degradation of the polysaccharide polymer 8.
Physical cross-linking method
In this case, physical interactions occur between different polymer chains by forming hydrogen bonds to prevent the hydrogel from being dissolved. In this method, the mechanical strength of the film increases due to the presence of ice crystals, which function as a biological cross-linker material. The chains are separated from the ice crystals when they are close together, forming polymer crystals, where hydrogen bonds are formed between the polymer chains. In some studies, this method depends on the freeze process time of the hydrogel and the number of freeze-thawing cycles 8-10.
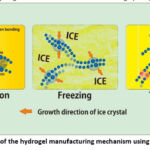 |
Figure 2: Schematic diagram of the hydrogel manufacturing mechanism using the freeze-thawing method |
Crystal formation in PVA solution using the Freeze Thawing method is known to have a relationship between PVA concentration, freezing time, and melting time. The results using the Freeze Thawing method at a temperature of -20°C for 45 and 60 minutes and room temperature of 23°C for 12 hours showed an increase in crystallinity when the freezing time increases. In the melting process, crystallinity will increase and then decrease due to damage to the crystal structure. However, its degree decreases along with the increasing concentration of PVA 9.
The manufacture of PVA hydrogels using the Freeze Thawing method showed the effect of the cycle number on bioadhesive properties, swelling ratio, and in-vitro residence time. This indicated that increasing the number of Freeze Thawing cycles reduces these three factors 9.
Film Forming System
Film Forming System is a non-solid dosage that forms a film on the targeted area after being applied to the skin or other body surfaces. It consists of an active ingredient and a film-forming additive in a carrier. The carrier produces a film containing the drug as shown in Figure 3.
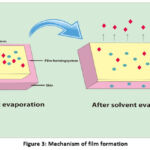 |
Figure 3: Mechanism of film formation |
The resulting film is either a solid polymer material acting as a matrix to regulate drug release on the skin or a liqrapidly absorbed into the stratum corneum. The drug concentration increases throughout this process, reaching saturation and possibly supersaturation levels on the skin surface. Achieving supersaturated drug levels will increase drug flux by increasing the thermodynamic activity of the formulation without affecting the skin as a barrier, reducing side effects or irritation 10.
Film forming has a combination of the transdermal patch and semisolid dosage forms. Therefore, it has the advantages of both dosage forms, as shown in Table 1, which summarises the benefits of FFS over Patch and Semisolid forms. This is supported by the drug pattern of the three systems shown in Figure 3 10.
Table 1: Comparison of topical delivery systems
|
|
Patch |
Film Forming |
Semisolid form |
|
Visual Form
Skin feel
Applications
Dose Adjustment
Dosage Frequency
Sustained release
Occlusive Properties
Wipe off resistance
Residual residue |
Very visible Non-sticky, non-greasy Easy Low 1-7 days Yes Yes Yes Possible |
Almost invisible Non-sticky, non-greasy Easy High 1-2 days Yes No Yes No |
Visible
Sometimes sticky, greasy
Sometimes messy High
1 day or less
No
No
No
No |
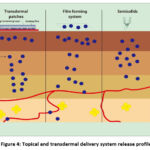 |
Figure 4: Topical and transdermal delivery system release profile |
The formulation of the film-forming system may take the form of solutions, gels, or emulsions. Its compositions in solution or semisolid form contain a film-forming polymer as a base for forming a film matrix 11. Initially, film development was used in surgery or wound care as tissue glue for covering after surgery and in cosmetic products. Some factors that affect the delivery of active ingredients from film forming include physicochemical properties, type and concentration of polymer, plasticizer, metamorphosis after application, and other additives such as penetration enhancers, lipids, or cyclodextrins. Furthermore, the preparations from film forming apply to various shapes and in any place and have a long shelf life compared to conventional semisolid preparations 12.
Film Forming Hydrogel
Film Forming Hydrogel is a dosage form that changes shape to film by solvent evaporation after being applied to the wound area. It comprises a film-forming hydrophilic polymer, plasticizer, and volatile solvent tolerant to the skin. The characteristics of this hydrogel include the ability to form films resistant to physiological stress caused by skin movement and maintain a long time of contact between the film and skin. Furthermore, optimal Film Forming Hydrogels should have benefits such as easy application, drying quickly on the skin, having suitable hardness and adhesiveness, and possessing film benefits such as good flexibility and elasticity [8].In this hydrogel formulation, the active ingredients dissolved in the film-forming carrier are incorporated in the film formed on the skin, which functions as an external carrier or limits the supply of active ingredients, thus regulating the release of active ingredients 11.
The active ingredient intended for film-forming hydrogel applications can penetrate the stratum corneum. Lipophilic active ingredients can penetrate the stratum corneum better than hydrophilic active ingredients. The active ingredient should ideally have logP 1 and 3 and have a molecular weight lower than 1000 Da because a small molecular weight indicates a higher diffusion speed. Another characteristic of active ingredients that must be considered in formulation development is solubility. If the carrier in the film-forming formulation contains organic solvents, the active ingredients must be soluble in these solvents. Formulations with dissolved drugs must have a pH value of 5-10 because the skin’s pH 5. The formulation’s pH value must be in that range to avoid skin irritation during application. The optimal pH value for penetration is <7 12.
The preparation is commonly applied to the wound area, and the resulting film holds the effects of physiological stress due to skin movement. Film Forming Hydrogel is designed to be a gel when stored in a tube or package; however, after applying it for a certain period, it transforms into a thin film 12.
Film Forming Hydrogel Component
The type and concentration of polymer, solvent, plasticizer, other additives, and active ingredients influence the characteristics of Hydrogel Film Forming. One example is the Sodium Fusidat formulation, used for wound healing with a combination of PVA and PVP polymers, ethanol with a minor concentration as a solvent, and propylene glycol as a plasticizer 12.
Components of Hydrogel Film Forming Formulation
Polymer
Polymer is one of the factors that influence the Hydrogel Film formulation. At skin temperature (28 – 32oC), it forms a thin and light film, forming a skin layer, and also has high flexibility and affinity to the skin to avoid excessive use of plasticizers. The polymer is combined with other film-forming polymers to obtain the desired properties. Hydrophilic polymers are natural or synthetic and absorb and retain large amounts of water. The formulation will create contact with the skin by forming a semi-occlusive film. Therefore the active ingredients are concentrated in the polymer matrix. The polymers that can be used in the formulation of Hydrogel Film Forming are shown in Table 2.
Table 2: Film Forming Polymer Solvent.
|
Polymer |
Characteristics |
|
Hydroxypropyl Methylcellulose (HPMC) HPMC (E4M, E15, E50M, K4M) |
The resulting film has a good texture because it is thin and not greasy. Does not interact with other ingredients. Surface active agent adsorbs water, then it is easily dispersed, lubricating, and provides a comfortable feeling in occlusive conditions after being applied to the skin. |
|
Ethyl-cellulose |
Non-toxic, non-irritating, non-allergenic. Good film-forming creates a strong film. |
|
Hydroxypropyl cellulose |
Nonionic, not pH sensitive. Soluble water |
|
Polyvinyl pyrrolidone (PVP) PVP K30, PVP VA64 |
Soluble in water and other solvents. Has adhesive and binding properties. It can function as a bioavailability enhancer. |
|
Polyvinyl alcohol (PVA) |
Soluble water. Excellent film-forming and adhesive. Non-toxic and biocompatible. |
|
Chitosan |
Excellent film forming. Increases paracellular permeability and drug penetration. Control drug release. |
|
Eudragit (Polymethacrylate copolymer) Eudragit RS100, RL 100, NE, RS 30D, S100 |
Transparent, elastic, self-adhesive. It has good adhesive strength on the skin. |
|
Silicone Polydimethylsiloxane (PDMS) |
Water vapor permeable. It has the adequate adhesive ability and durable film. |
|
Copolymer acrylate Avalure(R) AC 118, AC 120 |
Tough, breathable, and resistant to abrasion (scratches). |
The solvents used in Film Forming Hydrogels should evaporate immediately to create a film after application. They are usually organic. However, their use may cause irritation and damage to the skin. Commonly used solvents include ethanol and isopropanol. The development of ethanol as a solvent in Hydrogel Film Forming at a concentration of 8% showed the fastest drying time.
Moreover, increasing the ethanol concentration in the formulation showed an increase in the strength and adhesive properties of the film. However, it has no significant effect on its mechanical properties. Other solvents used are shown in Table 3.
Table 3: Solvents in topical delivery systems.
|
Category |
Example |
|
Glycol |
Propylene glycol, polyethylene glycol |
|
Alcohol |
Ethanol, butanol, isopropanol, benzyl alcohol, lanolin alcohol, fatty alcohol |
|
Other solvents |
Ethyl acetate, oleic acid, isopropyl myristate |
Plasticizer
The plasticizer is used in film-forming hydrogel to give flexibility and improve the tensile strength of the resulting film. It should be compatible with polymers and have low permeability. The plasticizers commonly used in formulas are glycerol, polyethylene glycol, sorbitol, dibutyl phthalate, propylene glycol, triethyl citrate, and others. Glycerol and sorbitol belong to the polyol group, which has a hydroxyl group. Therefore, it reduces internal hydrogen bonds (polymer-polymer interactions) 13.
Conclusion
Film Forming Hydrogel is a dosage form consisting of a film-forming hydrophilic polymer, a plasticizer, and a skin-tolerant volatile solvent. Polyvinyl alcohol (PVA)-hybrid hydrogel membranes are nominated as the most frequent polymer membrane candidates. The formulation will contact the skin by forming a semi-occlusive film to concentrate the active ingredients in the polymer matrix. The film that is created must be thin, transparent, and have high flexibility and affinity for the skin to be very suitable for use as a wound dressing.
Acknowledgment
This research is supported and funded by the International Collaborative Development Research Maulana Malik Ibrahim State Islamic University, Malang, Indonesia, in 2022-2023.
Conflict of Interest
The author declares that there are no conflicts of interest.
Funding Sources
There are no funding sources.
References
- Maqbool A, Mishra M. K, Pathak S, Kesharwani A, Kesharwani A. Semi-Solid Dosage Forms Manufacturing: Tools, Critical Process Parameters, Strategies, Optimization, and Recent Advances. Indo. Am. J. Pharm. Res., 2018; 7: 882-893.
- Suksaeree J, Luprasong C, Monton C. Swelling Behavior of Polyvinyl alcohol and lactic acid hydrogel films. Asian. J. Pharm. Sci., 2016; 11: 102-103.
CrossRef - Thiruvoth F. M, Mohapatra D. P, Sivakumar D. K, Chittoria R. V, Nandhagopal V. Current concepts in adult wound healing physiology. Plast. Aesthet. Res., 2015; 2: 250-256.
CrossRef - Saranya T. V, and Manoj K. Formulation, Evaluation and Optimization of Novel Silver Sulfadiazine Loaded Film Forming Hydrogel For Burns. J. drugs. Med., 2016; 8: 1-10.
CrossRef - Sun J.P, Hou S.Q. Preparation and characterization of carboxymethyl chitosan hydrogel. Pig. Res Tech., 2016; 45: 246-251.
CrossRef - Kim D. W, Kim K. S, Seo Y. G, Lee B. J, Park Y. J, Youn Y. S, Kim J. O, Yong C. S, Jin S. G, Choi H. G. Novel Sodium Fusidate-loaded film forming hydrogel with easy application and excellent wound healing. Int. J pharm., 2015; 495: 57-74.
- Mandegari M, Ghasemi-barakah L, Zamani M. Manipulating the degradation rate of PVA nanoparticles by a novel chemical‐free method. Polymers. Adv. Tech., 2019; 30: 230-239.
CrossRef - Lai W. F, and Rogach A. L. Hydrogel-based material for the delivery of herbal medicines. ACS. App. Mater. Interfaces., 2017; 9: 11309-11320.
CrossRef - Ranjha N. M, and Khan S. Chitosan/Poly (vinyl alcohol) Based Hydrogels for Biomedical Applications: A review. J. Pharm. Alter. Med., 2017; 2: 30-41.
- Oliveira R. N, McGuinness G. B, Ramos M. E. T, Kajiyama C. E, Thire S. M. Properties of PVA Hydrogel Wound-Care Dressings Containing UK Propolis. Macromolecular Symposia., 2016; 368: 122-127.
CrossRef - Gajra B, Pandya S. S, Sing S, Rabari H. A. Mucoadhesive Hydrogel Films of Econazole Nitrate: Formulation and Optimization Using Factorial Design. J.Drug. Delivery., 2015; 5: 223-230.
- Kathe K and Kathpalia H. Film forming systems for topical and transdermal drug delivery.Asian. J. Pharm. Scie., 2017; 12: 487–497.
CrossRef - Saudagar B. J, Gangurde P. A. Formulation, Development, and Evaluation of Film-Forming Gel for Prolonged Dermal Delivery of Miconazole Nitrate. Int. J. ChemTech. Res., 2017; 10: 289-299.







