Manuscript accepted on :04-07-2025
Published online on: 03-09-2025
Plagiarism Check: Yes
Reviewed by: Dr. Anjaneyulu Vinukonda
Second Review by: Dr. Sohayla Mohamed Elsherbini Attalla
Final Approval by: Dr. Mariia Shanaida
Department of Zoology, Gauhati University, Assam, India
Corresponding Author E-mail:aashishdutta.glt@gmail.com
DOI : https://dx.doi.org/10.13005/bpj/3235
Abstract
Traditional knowledge trapped amongst ethnic groups require appropriate documentation for resource conservation purpose and also invites authentic scientific validation. The study is henceforth directed towards documenting the traditional knowledge of herbal formulations utilized by tea tribes of Titabor sub-division of Jorhat district along with performing of a comparative analysis of these formulations used by the tea tribes of the entire Assam. Survey was conducted in tea garden areas of Titabor sub-division and in-depth literature exploration involving diverse articles published on ethno-pharmacology of therapeutic plants utilized by tea tribes of Assam was performed utilizing following keywords:- Medicinal plants, Herbal Formulations, Tea Tribes and Assam. Information about a total of 10 herbal formulations (5-Mono-Herbal Formulations/5-Poly-Herbal Formulations) were obtained through proper consultation from January 2022 to July 2022. Performing comparative analysis revealed that herbal formulations (91% were MHFs and 9% were PHFs) were used for treating human diseases like jaundice (20%), rhematoid arthritis (16%) and respiratory diseases (13%) with around 37% preparation in paste or powdered form while 32% correspond to liquid form or juice. Majority of them are being administered orally (78%) and topically (22%). Around 8% of these plants belong to Lamiaceae family followed by Fabaceae (7%) and Asteraceae (5%) while leaves (35%), bark/roots (10%) and whole plant (8%) were mostly used. Successful pre-clinical and clinical trials involving these formulations for treating respective disorder will lead to patenting and commercialization in turn causing benefit sharing with the community.
Keywords
Documentation; Ethno-pharmacology; Herbal Formulations; Survey; Tea tribes
Download this article as:| Copy the following to cite this article: Das M, Dutta A. Preliminary Study of Ethno-medicinal Practices of the Tea Tribes in Titabor Sub-division of Jorhat District, Assam. Biomed Pharmacol J 2025;18(3). |
| Copy the following to cite this URL: Das M, Dutta A. Preliminary Study of Ethno-medicinal Practices of the Tea Tribes in Titabor Sub-division of Jorhat District, Assam. Biomed Pharmacol J 2025;18(3). Available from: https://bit.ly/41yBqfg |
Introduction
India is regarded as one of the leading producers of medicinal plants specifically the North-eastern region which is one of the wealthiest bio-diversity region with numerous rare and endemic species.1,2 North-East India especially Assam is considered as the paradise for ethno-botanists with enormous vegetational wealth owing to topography and climatic conditions with more than 150 tribes existing in the state with the tea tribes being one amongst them.3 A rich diversity of both the population and flora in the state have provided an edge to its inhabitants since ancient times. Traditional knowledge has played a significant role in conservation of resources, mostly of indigenous plant species important for indigenous ethnic communities.4,5 Ethnic groups possess significant traditional medicine knowledge which requires appropriate documentation.6 Around 65% of Indian population is dependent upon traditional therapies.7 The tea tribes are multi-ethnic tea garden workers with many sub-tribes pre-dominantly found in different districts of Upper Assam.
Authentic record-keeping of traditional knowledge of tea communities is important in understanding the usage of medicinal plants in a specific region which primarily ensures the preservation of native cultural heritage from being lost. Furthermore it can be considered as an essential tool for carrying out extrapolative research in the field of bioactive studies on specific plant species which might land us in discovering active pharmaceutical ingredients with promising dug candidate properties.8,9 This kind of study also aids in the investigation along with enumeration of the remarkable role played by pharmacologically important plant species within local socio-cultural context.10 Henceforth the present study is a preliminary work encompassing the formulations utilized by the tea tribes of Titabor sub-division of Jorhat district, Assam as well as a comparative analysis of the traditional knowledge amongst tea tribes spread across Assam.
Materials and Methods
Survey was conducted in tea garden areas inhabited by the local tea tribes of Titabor sub-division (Latitudes 26o5462’ N and 26o5441’ N and Longitudes 94o12709’ E and 94o14890’ E) of Jorhat district. Data was collected through personal communication, interviews, discussions and observation. The respondents were mostly the traditional healers. Documentation was performed through interviews conducted with the aid of modified semi-structured questionnaire.11,12 The information about plants and plant parts utilized, procedure of preparation, mode of administration and dosage were noted. Additionally, information like the symptoms of diseases, age group, gender of patients and recovery percentage were also recorded.
 |
Figure 1: Semi-structured questionnaire (slightly modified) for documenting information on medicinal plants.11 |
Furthermore, an in-depth literature exploration involving a structured electronic and library search of different indexed and non-indexed journals and diverse articles published on ethno-pharmacology of medicinal plants involving databases like Scopus, Research gate, ScienceDirect, PubMed, Google Scholar used by tea tribes of Assam was performed for a comparative analysis on the disease type, type of formulation, type of preparation, mode of administration, families of plants used and plant part used. The researchers have used the following keywords or a combination of the following for extracting information:-
Medicinal plants
Herbal Formulations
Tea Tribes
Assam
Human diseases
Results
Socio demographic data, plant samples and dosages
Conduction of thorough survey involving documentation of ethno-pharmacological knowledge landed us with interaction with the tea tribes of Titabor sub-division of Jorhat district, Assam. Although not all the healers were interested in sharing their knowledge thereby remaining sceptical about the unethical commercialization of their formulations while some shared their knowledge willingly. The demographic features of respondents of the survey area is being depicted in Table 1.
Table 1: Demographic characteristics (n=10) of respondents in the study area
| Characters | Frequency | |
| Gender | Male | 8 |
| Female | 2 | |
| Age | <30 years | 0 |
| 30-60 years | 4 | |
| >60 years | 6 | |
|
Education |
Primary | 6 |
| Secondary | 3 | |
| Education above higher secondary | 1 | |
| Religion | Hindu, Christian | |
| Years of experience | 0-10 years | 7 |
| >10 years | 3 | |
The data revealed that 80% of the healers were male while remaining (20%) were female. Age of the healers was between 30-73 years. Most of them had little formal education while only a few had the desirable qualification. A total number of 10 herbal formulations (MHFs/PHFs) were mentioned by the respondents utilized for the treatment of various human disorders (Table 2).
Survey and Documentation of traditional knowledge
The different herbal formulations prescribed by the healers is being listed in Table 2.
 |
Table 2: Herbal Formulations (Mono/Poly) used for treatment of human diseases. |
 |
Figure 2: Herbal formulations used by the tea tribes of in Titabor sub-division |
Comparative analysis of traditional knowledge
While analysing the traditional knowledge amongst the tea tribes of Assam performed through in-depth literature review, the different disorders, the type of formulations, herbal preparation forms, mode of administration, families of the plants used in these formulations and plant parts used in these formulations were taken into account and represented through Fig. 3, 4, 5, 6, 7 and 8 respectively.
 |
Figure 3: Bar graph showing the human diseases treated by herbal formulations |
 |
Figure 4: Bar graph depicting the herbal formulation types used for treating human diseases. |
 |
Figure 5: Bar graph showing the different forms of herbal formulations. |
 |
Figure 6: Bar graph showing the proportion of the different modes of administration of the herbal formulations. |
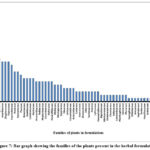 |
Figure 7: Bar graph showing the families of the plants present in the herbal formulations. |
 |
Figure 8: Bar graph showing the plant parts used in herbal formulations (in percentage). |
While performing the comparative analysis, it was found that jaundice (20%) is mostly targeted followed by rheumatoid arthritis (16%) and respiratory disorders (13%) (Fig. 3) while around 91% of the herbal formulations targeting the different disorders affecting the tea tribes of Assam are MHFs while remaining 9% correspond to PHFs as depicted through Fig. 4. Furthermore it has also been revealed through this study that most herbal formulations used by tea tribes are administered in paste or powder form (37%), followed by liquid form (32%) and decoction (13%) (Fig. 5). Around 78% of the formulations are administered orally (improved absorption, avoidance of molecular interaction and targeted efficacious action) while remaining 22% of them have topical administration (massage/bath/inhalation) (Fig. 6). The plants utilized in preparing these herbal formulations mostly belong to Lamiaceae family (8%) followed by Fabaceae (7%), Asteracae (5%), Apiaceae (4.44%), Acanthaceae (4.1%), Zingiberaceae (4.1%) and Piperaceae (4.1%) as visualized through Fig. 7. As leaves harbour a major proportion of bioactive compounds in them, they are being used mostly utilized in constituting the formulations (35%) followed by the utilization of bark/root (10%) and whole plant (8%) (Fig. 8).
Discussion
The survey, documentation and comparative analysis of the traditional knowledge trapped in the tea tribes of Assam appears to be a very mild yet significant step in transcending the ethno-pharmacological knowledge from these tribal communities to the scientific community. In fact the study functions in bridging the knowledge gap and as such opens up naive formulations for scientific authentication and validation which in long run might lead to development of herbal drugs. The study disclosed the pre-dominance of male traditional healers (80%) with female healers accounting for remaining 20% with majority having little formal education. As reported by the healers, some of them have been taught about these formulations by their fore-fathers (grand-father) while others claim of learning about the formulations in their dreams.
As visualized from Table 2, almost all the plants prescribed by the healers have respective therapeutic property for its usage in the form of herbal formulation for treating specific disease as scientific experiments carried out validates and henceforth substantiates the claims of these healers, for example, the chloroform fraction of the methanolic Drymaria cordata leaf extract demonstrated hepato-protective effect in Mono-Sodium Glutamate (MSG)-induced rat liver injury,13 while the essential oils from Piper nigrum reversed the CCl4-enhancedhepatic marker enzymes [alanine transaminase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (AKP) and malondialdehyde (MDA],14 and Zinziberofficinale also exerted hepato-protective effect in HgCl2 induced hepatoxic rat livers.15 The fact that the seeds of T. arjuna is being used in jaundice correlates to its remarkably high anti-oxidant potential.16 Experimental evidence suggests the capability of a triterpenoid isolated from Centella asiatica, asiatic acid in lowering inflammatory disorders while the anti-nociceptive and anti-inflammatory property of Tagetes erecta leaf extract was manifested in rat and mice model.17,18 Even Cannabis sativa stem extract showed both anti-bacterial (Staphylococcus aureus) and anti-fungal activity (A. niger, Aspergillus parasiticus and Aspergillus oryzae).19,20 Ethanolic Pouzolzia zeylanica extract demonstrated anti-fungal activity against Blastomyces dermatitides, Microsporum spp., Candida albicans, Trichophyton spp.etc.,21 while topical garlic (Allium sativum) extract application is efficacious against psoriasis, alopecia areata, keloid scar, wound healing, cutaneous corn, leishmaniasis, skin aging and rejuvenation.22 A capsular Phyllanthus niruri dosage (500 mg twice daily) in alcoholic hepatitis patients ameliorated the total antioxidant levels along with an appetite stimulant activity compared to a placebo justifying its usage as a herbal formulation by the healers.23 Furthermore, methanolic Drymaria cordata extract exhibited significant anti-tussive activity comparable to that of codeine phosphate, a prototype anti-tussive agent in a concentration-dependent manner.24 The different root and rhizome solvent extracts viz. ethanolic, chloroform, aqueous, petroleum ether extract of Cyperus rotundus exhibited anti-oxidant activity in terms of percent inhibition of haemoglobin glycosylation,25 while rhizome ethanolic extract is reported to be more efficacious against Staphylococcus epidermidis, Bacillus cereus and Pseudomonas aeruginosa.26 The leaf and bark extracts of Azadirachta indica possess significant anti-oxidant property with the bark being more potent with high phenolic content,27 while the methanol and chloroform extracts were found to be more efficient than the conventional antibiotics against Staphylococcus aureus and P. Aeruginosa.28 The chloroform seed extract of Caesalpinia bonduc demonstrates anti-oxidant activity,29 while the aqueous and ethyl acetic acid C. bonduc seed extracts demonstrates significant anti-fungal activity against numerous fungi including C. albicans and Aspergillus niger.30 The essential oils of Solanum spirale Roxb. unripe fruits and leaves demonstrated anti-bacterial activity against Mycobacterium tuberculosis H37Ra, Escherichia coli and Staphylococcus aureus while the anti-oxidant potential demonstrated by the methanolic shoot and berry extract of Solanum spirale Roxb. is attributable to their flavonoid and phenolic content.31,32,33 Furthermore the amalgamation of Ocimum tenuiflorum and Azadirachta indica leaves aid in lowering diabetic symptoms and blood pressure of non insulin dependent male diabetic individuals.34 Even Piper nigrum which contains piperine is found to alleviate hypertension in wistar rats.35 The ethanolic leaf extract of Psidium guajava inhibited E. coli and Salmonella enteridis growth with ZOI diameters in the range of 10-15 mm at 50 mg/disk.36 The plant species in these formulations definitely possess therapeutic potential owing to the presence of phyto-compounds in them. The fact that the healers have been able to preserve this knowledge and transcend it through time by prescribing them for treatment of various disorders is truly remarkable as each of these formulations target a specific disease. Furthermore the manner of preparation, dosage prescribed and diet restrictions associated with their prescription adds value to the formulation’s therapeutic property exhibition. Diet restrictions are useful because the compounds in those diets might hinder mechanism of action, delay recovery, minimize effectiveness, induce allergic reactions and even prevent interactions with other compounds. Moreover the traditional knowledge trapped in these tea communities definitely pave way for proper clinical trials for treating the respective disease post successful pre-clinical trials. When such formulations successfully cross the barriers (pre-clinical and clinical trials), these can be incorporated to form a herbal drug with reduced side effects, equivalent efficacy and higher acceptability as compared to allopathic medicines to treat various human diseases. These herbal drugs are safe and produce desired pharmacological effects, making them one of the highly selected drugs of choice. The commercialization of the herbal drug following successful trials will also lead to benefit sharing with these respondents/traditional healers and generation of livelihood for them.
Jaundice (20%), rheumatoid arthritis (16%) and respiratory disorders (13%) are the three most formulation targeted diseases (Fig. 3). The reason for jaundice mostly treated might be because of the inadequate nutrition and substandard living conditions living conditions of the tea tribes with tremendous water scarcity and deteriorating water quality. Furthermore poor sanitary conditions and low personal hygiene add to the causation of jaundice.37 Studies have identified a high prevalence of hemoglobinopathies, such as sickle cell anaemia and β-thalassemia, amongst tribals working in Assam’s tea gardens. These genetic disorders can lead to anaemia, which may strain liver function and potentially contribute to jaundice.38 Secondly, rheumatoid arthritis, an auto-immune disorder is being targeted as the repetitive and strenuous nature of perform physically demanding tasks, such as plucking tea leaves for long hours, bending, and carrying heavy loadscan put immense strain on the joints, which may exacerbate or potentially trigger autoimmune responses, especially in individuals who are genetically predisposed to RA. Thirdly even the respiratory disorders like tuberculosis are affecting the tea population in a remarkable manner for which the formulations are also being designed.39
Mostly MHFs (91%) are prepared for treating the disorders while a meagre 9% formulations are PHFs (9%) as certain issues concerning the sources and manufacturing processes, patients, drug-herb interaction and toxicity arise with respect to PHFs.40 Moreover these MHFs are easier to study, standardize and understand in terms of pharmacological effects and mechanisms while the clinical reproducibility of most of the ayurvedic PHFs is difficult to accomplish pushing for the usage of MHFs.41 Majority of these formulations are administered in paste (improved absorption, topical application, easy to use) or powdered form (longer shelf life, precise dosage, versatility) (Fig. 5).
Furthermore oral administrations account for 78% owing to improved absorption, avoidance of molecular interaction and targeted efficacious action while remaining 22% of them have topical administration (massage/bath/inhalation)(Fig. 6). As visualized through Fig. 7, the plants belonging to Lamiaceae family (8%) followed by Fabaceae (7%) and Asteracae (5%) are utilized in herbal formulations. The plants belonging to Lamiaceae family harbour an array of bio-active compounds like phenolic acids, flavonoids, alkaloids and other phyto-chemicals including omega-3,42 which are responsible for exhibiting the required therapeutic properties in turn making them use in these herbal formulations. Moreover these herbal formulations make use of leaves as a major proportion of bioactive compounds are being present in the leaves (35%) followed by bark/root (10%) and whole plant (8%) (Fig. 8).
Research in ethno-pharmacology has gained quite attention for the fact these herbal medicines come with added benefits compared to allopathic ones in the market. Furthermore the ethno-medicinal researchers form the base for the development of novel herbal drug formulations. Prompt urbanization has led to the undermining of traditional knowledge which has an immediate need for conservation. However the traditional fermented foods prepared by these communities also ameliorate digestibility, detoxification, and overall nutrition content which in turn is human health beneficial.43 Thus, ethno-medicinal study indeed paves the way for developing traditional as well as modern drugs for the welfare of the human society.
Conclusion
The present study is significant in the sense that it emphasizes on the ethno-medicinal utilization of most of the recorded plant species that have an important role in providing primary health care to the community. As all the prescribed plant species in the formulations possess scientifically validated therapeutic properties, the usage of these species in treating human disorders have been successfully justified. Total documentation of the medicinal plants used by these tea tribes is far from complete. Furthermore authentic scientific validation of the claims of these tribes may lead to the development of herbal drugs. Commercialization of these drugs in turn will bring about benefit sharing with the tea tribes/traditional healers. Henceforth extrapolative comprehensive and exploratory scientific studies need to be undertaken for understanding the complete picture.
Acknowledgement
The authors are thankful to the Head, Department of Zoology, DST FIST, DST PURSE, Gauhati University for providing the necessary facilities and equipments for conducting the purpose of the study. We also acknowledge Bioinformatics Infrastructure Facility, DST SERB for providing the financial support.
Funding Sources
The authors acknowledge the DST SERB ECR Grant with Sanction Number: ECR12016/000809 dated 7th March 2017 for provision of financial support.
Conflict of Interest
The authors do not have any conflict of interest.
Data Availability Statement
This statement does not apply to this article.
Ethics Statement
As no experimental work was associated with the work, ethical permission is not required.
Informed Consent Statement
Consent was taken from the respondents for carrying out the study involving surveying and documentation.
Clinical Trial Registration
This research does not involve any clinical trials.
Permission to reproduce material from other sources
Not applicable
Author Contributions
- Manas Das: Conceptualization, Resources, Supervision, Methodology.
- Aashis Dutta: Data curation, Formal analysis, Methodology, Writing-original draft;
References
- Maikhuri RK, Gangwar AK. Ethnobiological notes on the Khasi and Garo tribes of Meghalaya, Northeast India. Econ Bot. 1993;47:345.
CrossRef - Mao AA, Hynniewta TM. Floristic diversity of North East India. J Assam Sci Soc. 2000;41:255–266.
- Dutta BK, Dutta PK. Potential of ethnobotanical studies in North East India: An overview. Indian JTrad.Know. 2005;4(1):7-14.
- Kayani S, Ahmed M, Sultana S, Shinwari ZK, Zafar M. Ethnobotany of medicinal plants among the communities of alpine and sub-alpine regions of Pakistan. JEthnopharmacol. 2015;164:186-202.
CrossRef - Cox PA. Will tribal knowledge survive the millennium? Sci Ernst. 2000;287:44-45.
CrossRef - Karunamoorthi K, Tsehaye E. Ethnomedicinal knowledge, belief and self-reported practice of local inhabitants on traditional antimalarial plants and phyto-therapy.J Ethnopharmacol. 2012;141:143-150.
CrossRef - Timmermans K. Intellectual property right and traditional medicine: policy dilemmas at the interface. SocSci Med. 2003;57:745-756.
CrossRef - Mahwasane ST, Middleton L, Boaduo N. An ethnobotanical survey of indigenous knowledge on medicinal plants used by the traditional healers of the Lwamondoarea, Limpopo province, South Africa. S Afr J Bot. 2013;88:69–75.
CrossRef - Rahmatullah M, Azam MNK, Rahman MM, et al. A survey of medicinal plants used by Garoandnon-Garo traditional medicinal practitioners in two villages of Tangail district, Bangladesh. Am -Eurasian J Sustain Agric. 2011;5:350–357.
- Sargin SA, Büyükcengiz M. Plants used in Ethnomedicinal practices in Gulnar district of Mersin, Turkey. J Herb Med. 2019;15:1002-1024.
CrossRef - Savithramma N, Yugandhar P, Devi P. S, et al. Documentation of ethnomedicinal information and antimicrobial validation of Thespesiapopulnea used by Yanadi tribe of Ganugapenta village, Chittoor district, Andhra Pradesh, India. J IntercultEthnopharmacol. 2017;6:158-169.
CrossRef - Banerjee S, Nayak D, Sinha A. Adivasi (Tea Tribe) worldviews of living close to wild Asian elephants in Assam, India. Conserv Biol. 2024;38(6):e14397. doi: 10.1111/cobi.14397.
CrossRef - Olowofolahan AO, Olanlokun JO, Olorunsogo OO. GCMS analysis andPhytoprotective effect of chloroform fraction of methanol leaf extract of Drymariacordata against MSG-induced lesions in specific tissues. Afr J Med MedSci. 2020;49:409-419.
- Zhang C, Zhao J, Famous E, Pan S, Peng X, Tian J. Antioxidant, hepatoprotective and antifungal activities of black pepper (Piper nigrum L.) essential oil. Food Chem. 2021;346:128845.
CrossRef - EzeukoVitalis C, NwokochaChukwuemeka R, Mounmbegna Philippe E, NriaguChinonso C. Effects of Zingiberofficinale on liver function of mercuric chloride-induced hepatotoxicity in adult Wistar rats. Electron J Biomed. 2007;3:40-45.
- Aslam N, Ahmad M, Barkat K, Abbas MK. Antioxidant and Anti-urease Activity of Various Solvent Extracts of Terminalia arjuna seeds. Br J Pharm Res. 2017;20(6).
CrossRef - Yuyun X, Xi C, Qing Y, Lin X, Ke R, Bingwei S. Asiatic acidattenuates lipopolysaccharide-induced injury by suppressing activation of theNotch signaling pathway. Oncotarget. 2018;9:15036–15046.
CrossRef - Chatterjee S, Rajaranjan S, Sharma UR, Ramesh K. Evaluation of anti-nociceptive and anti- inflammatory activities of Tageteserecta. Arch Pharm Sci Res. 2009;1:207-211.
- Borchardt JR, Wyse D, Sheaffer C, et al. Anti-microbial activity of native and naturalized plants of Minnesota and Wisconsin. J MedPlant Res. 2008;2:98-110.
- IsahqMS, Afridi MS, Ali J, Hussain MM, Ahmad S, Kanwal F. Proximate composition, phyto-chemical screening, GC-MS studies of biologically active cannabinoids and anti-microbial activities of Cannabis indica. Asian Pac J Trop Dis. 2015; 5:897-902.
CrossRef - Saha D, Paul S. Anti-fungal Activity of Ethanol Extract of Pouzolziazeylanica (L.) Benn.Inter J Pharm Teach Prac. 2012;3:272-274.
- Pezyar N, FeilyA. Garlic in dermatology. Derm Reports. 2011;3.
CrossRef - Sowjanya K, Girish C, Bammigatti C, Lakshmi NC. Efficacy of Phyllanthusniruri on improving liver functions in patients with alcoholic hepatitis: A double-blind randomized controlled trial. Indian JPharmacol. 2021;53:448-456.
CrossRef - Mukherjee PK, Saha K, Bhattacharya S, Giri SN, Pal M, Saha BP. Studies on antitussive activity of DrymariacordataWilld. (Caryophyllaceae). J Ethnopharmacol.1997;56:77-80.
CrossRef - Pal DK, Dutta S. Evaluation of the Antioxidant activity of the roots and Rhizomes of Cyperusrotundus L. Ind J Pharm Sci. 2006;68:256–258.
CrossRef - Sharma SK, Singh AP. Antimicrobial investigations on rhizomes of Cyperusrotundus Linn. Der Pharma Lett. 2011;3:427–431.
- Ghimeray AK, Jin C, Ghimire BK, Cho DH. Antioxidant activity and quantitative estimation of azadirachtin and nimbin in AzadirachtaIndica A. Juss grown in foothills of Nepal. Afr J Biotechnol. 2009;8:3084–3091.
- Garg R, Perveen S, Gupta B, Bajpai VK. Evaluation of Antibacterial Activity of Annona squamosa, Psidiumguajava and Azadirachtaindica against Pathogenic Bacterial Cultures. Int J Curr. Res Biosci. Plant Biol. 2015;2:54-58.
- Sachan NK, Verma S, Sachan AK, Arshad H. An investigation to antioxidant activity of Caesalpiniabonducella seeds. Ann Pharmacol Pharm Sci. 2010;1:88-91.
- Shukla S, Mehta A, Mehta P, Vyas SP, Bajpai VK. Preliminary phytochemical and anti-fungal screening of various organic extracts of Caesalpiniabonducella seeds. Rom Biotechnol Lett. 2011;4:1646384-1646389.
- Keawsa-ard S, Liawruangrath B, Liawruangrath S, Teerawutgulrag A, Pyne SG. Chemical constituents and antioxidant and biological activities of the essential oil from leaves of Solanum spirale. Nat Prod Commun.2012; 7:955-958.
CrossRef - Payum T, Das A, Shankar R, Tamuly C, Hazarika M. Antioxidant potential of Solanum spirale shoot and berry: a medicinal food plant used in Arunachal Pradesh. Int J Pharmtech Res. 2015;5:307-314.
- Keawsa-ard S, Liawruangrath B, Liaewruangrath S, Teerawutgulrag A, Pyne S. Anti-cancer and antibacterial activities of the isolated compounds from Solanum spirale Roxb. leaves. Chiang Mai JSci. 2016;43:546-554.
- Kochhar A, Sharma N, Sachdeva R. Effect of Supplementation of tulsi (Ocimum sanctum) and neem (Azadirachtaindica) leaf powder on diabetic symptoms, anthropometric parameters and blood pressure of non insulin dependent male diabetics. Stud Ethno Med. 2009;3.
CrossRef - Hlavackova L, Urbanova A, Ulicna O, Janega P, Cerna A, Babal P. Piperine, active substance of black pepper, alleviates hypertension induced by NO synthase inhibition. BratislLekListy.2010;111:426-431.
- Hemeg HA, Moussa IM, Ibrahim S, et al. Antimicrobial effect of different herbal plant extracts against different microbial population. Saudi J BiolSci. 2020;27:3221-3227.
CrossRef - Basu SK. A health profile of tribal India. Health Millions.1994;2:12-14.
- Teli AB, Deori R, Saikia SP. Haemoglobinopathies and β-Thalassaemia among the Tribals Working in the Tea Gardens of Assam, India. J ClinDiagnRes.2016;10:19-22.
CrossRef - Medhi GK, Hazarika NC, Shah B, Mahanta J. Study of health problems and nutritional status of tea garden population of Assam. Indian J Med Sci.2006;60:496-505.
CrossRef - Thamanna P, Prasanth MLL. Comparative review on polyherbal and monoherbal cosmetic formulations. J Chem Sci. 2023;3:32-35.
CrossRef - Parasuraman S, Thing GS, Dhanaraj SA. Polyherbal formulation: Concept of ayurveda. Pharmacogn Rev. 2014;8:73-80.
CrossRef - Chakrabartty I, Mohanta YK, Nongbet A, et al. Exploration of Lamiaceae in Cardio Vascular Diseases and Functional Foods: Medicine as Food and Food as Medicine. Front Pharmacol.2022;13:894814.
CrossRef - Yumnam H, Hazarika P, Sharma I. Metagenomic insights into traditional fermentation of rice-based beverages among ethnic tribes in southern Assam, Northeast India. Front Microbiol. 2024;15:1410098.
CrossRef








