Shaik Gundikota Javeed Ahammed1 , Pradeepkumar Bhupalam1
, Pradeepkumar Bhupalam1 , Hindustan Abdul Ahad2*
, Hindustan Abdul Ahad2* , Haranath Chinthaginjala2
, Haranath Chinthaginjala2 , Syed Rahamathulla2
, Syed Rahamathulla2 and Srividya Yadav2
and Srividya Yadav2
1Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education and Research (RIPER) - Autonomous, Ananthapuramu – 515721, AP, India.
2Department of Industrial Pharmacy, Raghavendra Institute of Pharmaceutical Education and Research (RIPER) - Autonomous, Ananthapuramu – 515721, AP, India.
Corresponding Author E-mail: abdulhindustan@gmail.com
DOI : https://dx.doi.org/10.13005/bpj/2306
Abstract
The authors aimed to give a quick reference guide for humanity about the new threat even after the COVID-19 health battle i.e., the Black fungus also baptized as Mucormycosis infection. After recovering from COVID-19, patients with diabetes mellitus and patients who have undergone steroidal treatment are more prone to black fungus infection. This review gives quick information about various types of Mucormycosis infections, risk factors, symptoms, treatment, and prevention of black fungus. The things that can be and cannot be done to eradicate the black fungus. Any sign of black nasal mucosa/sputum, fever, headache, hazy/blurred/double vision with eye pain, loss of one side sensation on face and loss in the sensation while chewing, etc., then it should not be neglected and immediately intimated to the health professionals and get treated. If black fungus is unidentified early stages and untreated in time, the patients may lose their facial/neck parts as a part of cleaning surgery. The study concludes that by maintaining hygienic conditions, health checkups, and doctors’ advice one can fight and eradicate the black fungus.
Keywords
Black fungus; Infection; Prevention; Symptoms; treatment
Download this article as:| Copy the following to cite this article: Ahammed S. G. J, Bhupalam P, Ahad H. A, Chinthaginjala H, Rahamathulla S, Yadav S. Black Fungus: A Lethal Communal Issue After Winning the Life Battle Against COVID-19. Biomed Pharmacol J 2021;14(4). |
| Copy the following to cite this URL: Ahammed S. G. J, Bhupalam P, Ahad H. A, Chinthaginjala H, Rahamathulla S, Yadav S. Black Fungus: A Lethal Communal Issue After Winning the Life Battle Against COVID-19. Biomed Pharmacol J 2021;14(4). Available from: https://bit.ly/3aBGwwA |
Introduction
The entire world is fighting with COVID-19 and presently India is battling the second wave and disturbed with this noxious transmissible virus but also other impediments that are actuality stated by the patients1. One such fatal impediment being detected in patients in India in current periods, who have verified positive for COVID-19 and are progressively improving, is a fungal disease called Mucormycosis (MM) (earlier termed as zygomycosis) familiar as “black fungus”2,3. With hundreds of cases being stated in various states of India, it has activated an extra wave of panic among the overall public. MM, is an infrequent fungal contagion, prompted by the mucormycete mold, that occurs expansively in soil, leaves, decayed wood, and putrefied manure4.
The black fungus contagion is considered by a good darkening of the skin, inflammation, black nasal mucosal, redness, ulcers, fevers, this precarious illness can also assault the lungs, eyes and even the brain, demonstrating to be lethal if left unattended5,6. It is critical to appreciate the causal factors and protruding symptoms accompanying MM, to speedily detect any imaginable cautionary signs rising in both, COVID-19 patients and other persons. These must be punctually transported to the healthcare expert so that appropriate medical management can provide and the pretentious single convalesces absolutely.
Types of Mucormycosis
The popular MM that causes infections in humans as illustrated7-10:
Rhinocerebral MM: It is a contagion in the sinuses that can feast on the brain. This form of MM is furthermost in folks with unrestrained diabetes and in persons who have had a kidney displace.
Pulmonary MM: The most joint type of MM in persons with cancer and in persons who had an organ displacement or a stem cell displacement.
Gastrointestinal MM: The more collective among younger than aged, particularly impulsive and low birth weightiness babies <1 month of age, who had antibiotics, surgery, or medications that inferior the body’s capability to combat germs and sickness.
Cutaneous MM: happens after the fungi arrive the body concluded a break in the skin (for example, after surgery, a burn, or other types of skin trauma). This is the most mutual form of MM amongst persons who do not have declining immune systems.
Disseminated MM: It arises when the contamination feasts over the bloodstream to disturb an additional part of the body. The contagion most usually disturbs the brain, but also can disturb other organs such as the spleen, heart, and skin.
MM is any fungal contagion instigated by fungi in the order Mucorales. Normally, species in the mucor, Cunninghamella genera and rhizopus, absidia are utmost frequently concerned11,12. Hyphae often considered as disease increasing in and round blood vessels and may be hypothetically lethal in diabetic or brutally immunocompromised persons.MM and “zygomycosis” are occasionally used interchangeably13. Though, zygomycota has been acknowledged as polyphyletic, and is not comprised in modern fungal arrangement systems.
Also, while zygomycosis includes Entomophthorales, MM excepts this group. MM can chief to loss of the upper jaw and occasionally even the eye14. “Patients would need to arise to positions with loss of purpose because of an absent jaw-struggle with chewing, swallowing, facial aesthetics, and loss of self-confidence15.
While prosthetic standby of the absent facial arrangements can begin once the patient stabilizes after surgery, doctors it is imperative to calm him about the convenience of such intrusions instead of leave-taking him to panic with the abrupt, unexpected loss, expanding a post-Covid stress syndrome which is previously a reality, a maxillofacial prosthodontist. Prosthetic rebuilding can be caused after surgery, but provisional solutions should be arranged even earlier operation of the jaws for enhanced long-term fallouts16.
Risk factors
Not all persons who have constricted coronavirus contagion and are on management for COVID-19 attain MM. Certain persons are more prone to getting pretentious by the fungal contagion, such as17,18
Folks with diabetes mellitus are incapable to keep blood sugar points in the interior in the usual range.
Persons with comorbid circumstances enchanting immunosuppressant steroid medicines to achieve pre-existing infections and COVID-19, over a prolonged distance of period.
Being preserved in the ICU wing of hospitals for a continued intermission period.
Having a susceptible immune system that is deteriorated owed to comorbidities such as earlier organ transplant surgeries or cancer therapy measures.
Already enchanting prescription antifungal drugs to struggle infections.
Symptoms of black fungus
The symptoms of MM while recuperating from COVID-19 are as follows19. In accumulation to continuously observing COVID-19 patients with the aforementioned ailing situations who are on management, doctors’ necessity also has an eye out for these suggestions of Mucormycosis20,21.
Distinct blackish discoloration on the connection of the nose.
Further worsening of breathing roles, with torso aching, pleural effusion, and blood cough or hemoptysis.
Hazy vision, with objects blurred or in double, with eye pain.
Irregular thrombosis, sideways with skin wound and impairment or necrosis of skin.
Pain on solitary one side of the face, cheekbones, with the non-existence of sensation and protruding.
Protuberant sore in teeth, jawbone, humiliating of tooth structures.
Sinusitis, sideways with obstruction of the nasal tract and bloody or blackish nasal mucus expulsion.
Signs and symptoms
MM recurrently contaminates the sinuses, brain, or lungs. While contagion of the oral crater is the furthermost common form of MM, the fungus can also contaminate the gut and skin. In erratic instances, the maxilla may be pretentious by MM. The major blood vessel supply of maxillofacial areas typically prevents fungal infections, though more contagious fungi, such as those accountable for MM, can often overwhelm this trouble22,23.
If the illness includes the brain, then indications may comprise a partial headache, fiscal pain, pyrexia, nasal cramming that improvements to black ejection, and serious sinusitis with ophthalmic puffiness. Exaggerated skin may seem comparatively normal during the initial phases of contagion. This skin rapidly becomes reddened and may be swollen before ultimately turning black because of tissue decease. Other forms of MM may include the lungs, skin, or be prevalent through the body; indications may also comprise difficulty breathing, and tenacious cough. In cases of tissue disease, there might be nausea and vomiting, coughing up blood, and abdominal pain24.
The symptoms of MM also be contingent on every part by the fungus is mounting25-28. The facial images of pre and post-operative black fungus patients as shown in fig.1.
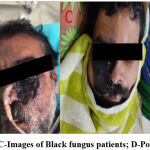 |
Figure 1: A, B and C-Images of Black fungus patients; D-Post operative patient |
Symptoms of Rhinocerebral MM
One-sided facial inflammation
Headache
Nasal or sinus cramming
Black grazes on mouth and nose
Fever
Symptoms of pulmonary MM
Fever
Cough
Chest pain
Shortness of breath
Symptoms of Cutaneous MM
Blisters or ulcers, and the ill area on the skin may turn black.
Other symptoms comprise pain, balminess, extreme soreness, or bump at the wound.
Symptoms of gastrointestinal MM
Abdominal pain
Nausea and vomiting
Gastrointestinal bleeding
Symptoms of disseminated MM
Classically happens in persons’ sick with other medical situations, so it’s stimulating to know which indications are connected to MM.
Patients with dispersed infection in the brain can advance mental position changes.
Treatment for the MM
After the diagnosis of MM is inveterate, then the instant management approach is to suggest antifungal medicines, to be reserved either orally if the contagion is still slight, or managed via injections in more aggressive cases, to the patient. These controlling prescription drugs own the capability to board the fungal samplings in the body and slow down their rapidity of dispersion within the system, as well as entirely control their disparaging movement.
This guarantees condensed impairment to bodily organs, thwarts fungal contagion entirely, averting grave difficulties and fatal consequences. It is directed to observe blood glucose levels even after the originally corona positive patient with diabetes mellitus has tested negative for COVID-19 and pursue medical care at once if there is an unexpected spike in blood sugar interpretations29.
Furthermore, medications may be expected to treat other pre-existing illnesses, such as diabetes, to lighten its concomitant symptoms. In conditions where serious impairment has happened in bodily tissues, surgical procedures are completed, to remove these fungal balls. Upon acceptance of all required corrective processes, the doctor keeps a check on the patient, to safeguard MM fungal contagion does not persist and assurance effective management, total repossession of the patient30.
Prevention of MM
Furthermore, simple precautionary procedures go a long way in dropping the probabilities of obtaining MM post-COVID-19 retrieval, such as31,32:
Guaranteeing personal hygiene by bathing and cleaning the body carefully, mainly after recurring home from work, employed out or staying neighbors, relatives, friends.
Tiring face masks and face safeguards when working in muted polluted environments such as manufacture sites.
Susceptible groups include persons who have health complications or take medications that inferior the body’s capability to combat germs and illness. These comprise those with diabetes, cancer, or persons with organ displace. Use masks if one is staying at grubby construction sites. Conserve personal hygiene comprising a detailed scrub bath. The analysis depends on the site of the supposed contagion. Treatment of MM necessities to be preserved with treatment antifungal medication. Sometimes subsequent loss of the upper jaw and occasionally even an eye.
Do’s and Don’ts in MM
Some things to be done, and some avoided tackling black fungus21,33,34.
Do’s
Regulate hyperglycemia.
Observe blood sugar conditions in post-COVID-19 liberation and also in diabetics
Use clean, sterile water for humidifiers through oxygen therapy.
Use antibiotics/antifungals cautiously.
Don’ts
Stop steroidal treatment with doctors’ advice.
Do not miss threatening signs and symptoms.
Do not deliberate all the cases with a congested nose as cases of bacterial sinusitis, predominantly in the scenery of immunosuppression and/or COVID-19 patients on immune-modulators.
Do not vacillate to seek destructive inquiries, as suitable (KOH staining & microscopy, culture) for perceiving fungal etiology.
Do not lose critical time to recruit management for MM.
After recuperating from coronavirus, one must closely observe and must not miss any warning signs and symptoms stated above, as the fungal contagion is originated to appear even weeks or months after retrieval.
Conclusion
Black fungus (Mucormycosis) infection will attack patients who recovered from COVID-19. Patients with diabetes mellitus and who took steroidal therapy are more affected by a black fungus infection. Patients who observed any symptoms of black nasal mucosa/sputum discharge, fever, headache, hazy/blurred/double vision with eye pain, loss of one side sensation on face and loss in the sensation while chewing, etc., should come under medical supervision and get treated. The study concludes that by upholding hygienic environments, health examinations, and doctors’ counsel one can contest and exterminate black fungus.
Acknowledgments
None
Conflict of Interests
None
Funding Source
None
References
- Cao, X. COVID-19: immunopathology and its implications for therapy. Nature Reviews Immunology, 20(5), 269–270. (2020). https://doi.org/10.1038/s41577-020-0308-3
CrossRef - Selbmann, L., Pacelli, C., Zucconi, L., Dadachova, E., Moeller, R., de Vera, J. P., & Onofri, S. Resistance of an Antarctic cryptoendolithic black fungus to radiation gives new insights of astrobiological relevance. Fungal Biology, 122(6), 546–554. (2018). https://doi.org/10.1016/j.funbio.2017.10.012
CrossRef - Chowdhary, A., Agarwal, K., & Meis, J. F. Filamentous Fungi in Respiratory Infections. What Lies Beyond Aspergillosis and Mucormycosis? PLOS Pathogens, 12(4), e1005491. (2016). https://doi.org/10.1371/journal.ppat.1005491
CrossRef - Seena, S., Bärlocher, F., Sobral, O., Gessner, M. O., Dudgeon, D., McKie, B. G., Chauvet, E., Boyero, L., Ferreira, V., Frainer, A., Bruder, A., Matthaei, C. D., Fenoglio, S., Sridhar, K. R., Albariño, R. J., Douglas, M. M., Encalada, A. C., Garcia, E., Ghate, S. D., . . . Graça, M. A. Biodiversity of leaf litter fungi in streams along a latitudinal gradient. Science of The Total Environment, 661, 306–315. (2019). https://doi.org/10.1016/j.scitotenv.2019.01.122
CrossRef - de Regt, M. J. A., Murk, J. L., Schneider-Hohendorf, T., Wattjes, M. P., Hoepelman, A. I. M., & Arends, J. E. Progressive multifocal leukoencephalopathy and black fungus in a patient with rheumatoid arthritis without severe lymphocytopenia. JMM Case Reports, 3(4). (2016). https://doi.org/10.1099/jmmcr.0.005053
CrossRef - Maitip, J., Zhang, X., Tan, K., Thai, P. H., Nabozhenko, M. V., Kirejtshuk, A. G., Chantawannakul, P., & Neumann, P. A scientific note on the association of black fungus beetles (Alphitobius laevigatus, Coleoptera: Tenebrionidae) with Eastern honey bee colonies (Apis cerana). Apidologie, 48(2), 271–273. (2016). https://doi.org/10.1007/s13592-016-0471-5
CrossRef - Kumar YB, Ahad HA, Haranath C, Sumanth G, Pasupuleti DS, Reddy SS. Platelet Rich Plasma Therapy: A quick note for every health care professional.Int. J. Life Sci. Pharma Res.;10(5): P84-89. (2020) https://doi 10.22376/ijpbs/lpr.2020.10.5.P84-89
- Chakrabarti, A., & Singh, R. Mucormycosis in India: unique features. Mycoses, 57, 85–90. (2014). https://doi.org/10.1111/myc.12243
CrossRef - Lin, E., Moua, T., & Limper, A. H. Pulmonary mucormycosis: clinical features and outcomes. Infection, 45(4), 443–448. (2017). https://doi.org/10.1007/s15010-017-0991-6
CrossRef - Chakrabarti, A., & Dhaliwal, M. Epidemiology of Mucormycosis in India. Current Fungal Infection Reports, 7(4), 287–292. (2013). https://doi.org/10.1007/s12281-013-0152-z
CrossRef - Gomes, M. Z. R., Lewis, R. E., & Kontoyiannis, D. P. Mucormycosis Caused by Unusual Mucormycetes, Non-Rhizopus, -Mucor, and -Lichtheimia Species. Clinical Microbiology Reviews, 24(2), 411–445. (2011). https://doi.org/10.1128/cmr.00056-10
CrossRef - Skiada, A., Pavleas, I., & Drogari-Apiranthitou, M. Epidemiology and Diagnosis of Mucormycosis: An Update. Journal of Fungi, 6(4), 265. (2020). https://doi.org/10.3390/jof6040265
CrossRef - Nucci, M., Engelhardt, M., & Hamed, K. Mucormycosis in South America: A review of 143 reported cases. Mycoses, 62(9), 730–738. (2019). https://doi.org/10.1111/myc.12958
CrossRef - Panigrahi, M. K., Manju, R., Vinod Kumar, S., & Toi, P. C. Pulmonary Mucormycosis Presenting as Nonresolving Pneumonia in a Patient with Diabetes Mellitus. Respiratory Care, 59(12), e201–e205. (2014). https://doi.org/10.4187/respcare.03205
CrossRef - Fernandez-Flores, A., Saeb-Lima, M., & Arenas-Guzman, R. Morphological Findings of Deep Cutaneous Fungal Infections. The American Journal of Dermatopathology, 36(7), 531–556. (2014). https://doi.org/10.1097/dad.0b013e31829cc6f3
CrossRef - Ajay Kumar Sahu, BS Arpita, Rekita Mohanty, Subhashree Dash, Purabi Baral, Surya Mishra, Pinki Samal, Bibekananda Pradhan, & Bhagyashree Nanda. Mucormycosis: A black fungus – post covid complication, clinical and pathogenic approaches and isolation and characterization of black fungus with correlate its current perspectives of biomedical waste management. GSC Biological and Pharmaceutical Sciences, 16(3), 059–070. (2021). https://doi.org/10.30574/gscbps.2021.16.3.0258
CrossRef - Borjian Boroujeni, Z., Shamsaei, S., Yarahmadi, M., Getso, M. I., Salimi Khorashad, A., Haghighi, L., Raissi, V., Zareei, M., Saleh Mohammadzade, A., Moqarabzadeh, V., Soleimani, A., Raeisi, F., Mohseni, M., Mohseni, M. S., & Raiesi, O. Distribution of invasive fungal infections: Molecular epidemiology, etiology, clinical conditions, diagnosis and risk factors: A 3-year experience with 490 patients under intensive care. Microbial Pathogenesis, 152, 104616. (2021). https://doi.org/10.1016/j.micpath.2020.104616
CrossRef - Vallabhaneni, S., Kallen, A., Tsay, S., Chow, N., Welsh, R., Kerins, J., Kemble, S. K., Pacilli, M., Black, S. R., Landon, E., Ridgway, J., Palmore, T. N., Zelzany, A., Adams, E. H., Quinn, M., Chaturvedi, S., Greenko, J., Fernandez, R., Southwick, K., . . . Chiller, T. M. Investigation of the First Seven Reported Cases ofCandida auris,a Globally Emerging Invasive, Multidrug-Resistant Fungus — United States, May 2013–August 2016. MMWR. Morbidity and Mortality Weekly Report, 65(44), 1234–1237. (2016). https://doi.org/10.15585/mmwr.mm6544e1
CrossRef - Gebremariam, T., Alkhazraji, S., Alqarihi, A., Wiederhold, N. P., Shaw, K. J., Patterson, T. F., Filler, S. G., & Ibrahim, A. S. Fosmanogepix (APX001) Is Effective in the Treatment of Pulmonary Murine Mucormycosis Due to Rhizopus arrhizus. Antimicrobial Agents and Chemotherapy, 64(6). (2020). https://doi.org/10.1128/aac.00178-20
CrossRef - Wagner, H. Natural products chemistry and phytomedicine in the 21st century: New developments and challenges. Pure and Applied Chemistry, 77(1), 1–6. (2005). https://doi.org/10.1351/pac200577010001
CrossRef - Pacelli, C., Selbmann, L., Moeller, R., Zucconi, L., Fujimori, A., & Onofri, S. Cryptoendolithic Antarctic Black Fungus Cryomyces antarcticus Irradiated with Accelerated Helium Ions: Survival and Metabolic Activity, DNA and Ultrastructural Damage. Frontiers in Microbiology, 8. (2017). https://doi.org/10.3389/fmicb.2017.02002
CrossRef - Seneviratne, C. J., Fong, P. H., Wong, S. S., & Lee, V. H. Antifungal susceptibility and phenotypic characterization of oral isolates of a black fungus from a nasopharyngeal carcinoma patient under radiotherapy. BMC Oral Health, 15(1). (2015). https://doi.org/10.1186/s12903-015-0023-9
CrossRef - Velasco, J., & Revankar, S. CNS Infections Caused by Brown-Black Fungi. Journal of Fungi, 5(3), 60. (2019). https://doi.org/10.3390/jof5030060
CrossRef - Etzel, R. A. What the Primary Care Pediatrician Should Know about Syndromes Associated with Exposures to Mycotoxins. Current Problems in Pediatric and Adolescent Health Care, 36(8), 282–305. (2006). https://doi.org/10.1016/j.cppeds.2006.05.003
CrossRef - Anda, C. C. O., Ndong, A. N., Ndoutoumou, P. N., & Loubana, P. M. Impact of arbuscular mycorrhizal fungus (Rhizophagus irregularis) on disease symptoms caused by the ascomycete fungus (Mycosphaerella fijiensis M.) in Black Sigatoka-resistant banana plantain. International Journal of Biological and Chemical Sciences, 14(2), 306–316. (2020). https://doi.org/10.4314/ijbcs.v14i2.1
CrossRef - Gao, P., Li, Y., Guo, Y., & Duan, T. Co-inoculation of lucerne (Medicago sativa) with an AM fungus and a rhizobium reduces occurrence of spring black stem and leaf spot caused by Phoma medicaginis. Crop and Pasture Science, 69(9), 933. (2018). https://doi.org/10.1071/cp18135
CrossRef - Aung, S. L. L., Liu, H. F., Pei, D. F., Lu, B. B., Oo, M. M., & Deng, J. X. Morphology and Molecular Characterization of a Fungus from the Alternaria alternata Species Complex Causing Black Spots on Pyrus sinkiangensis (Koerle pear). Mycobiology, 48(3), 233–239. (2020). https://doi.org/10.1080/12298093.2020.1745476
CrossRef - Selbmann, L., Grube, M., Onofri, S., Isola, D., & Zucconi, L. Antarctic Epilithic Lichens as Niches for Black Meristematic Fungi. Biology, 2(2), 784–797. (2013). https://doi.org/10.3390/biology2020784
CrossRef - Cole, S. A., Laviada-Molina, H. A., Serres-Perales, J. M., Rodriguez-Ayala, E., & Bastarrachea, R. A. The COVID-19 Pandemic during the Time of the Diabetes Pandemic: Likely Fraternal Twins? Pathogens, 9(5), 389. (2020). https://doi.org/10.3390/pathogens9050389
CrossRef - Seyedmousavi, S., Bosco, S. D. M. G., de Hoog, S., Ebel, F., Elad, D., Gomes, R. R., Jacobsen, I. D., Jensen, H. E., Martel, A., Mignon, B., Pasmans, F., Piecková, E., Rodrigues, A. M., Singh, K., Vicente, V. A., Wibbelt, G., Wiederhold, N. P., & Guillot, J. Fungal infections in animals: a patchwork of different situations. Medical Mycology, 56(suppl_1), S165–S187. (2018). https://doi.org/10.1093/mmy/myx104
CrossRef - Brandt, M. E., & Park, B. J. Think Fungus—Prevention and Control of Fungal Infections. Emerging Infectious Diseases, 19(10), 1688–1689. (2013). https://doi.org/10.3201/eid1910.131092
CrossRef - Yedire Bharath, K., Hindustan, A. A., Chinthaginjala, H., Gopavaram, S., Durga Sumanth, P., & Srilekha Surapa, R. Platelet Rich Plasma Therapy: A Quick Note for Every Health Care Professional. International Journal of Pharma and Bio Sciences, 10(5). (2020). https://doi.org/10.22376/ijpbs/lpr.2020.10.5.p84-89
CrossRef - Shin, S., Jung, S., Menzel, F., Heller, K., Lee, H., & Lee, S. Molecular phylogeny of black fungus gnats (Diptera: Sciaroidea: Sciaridae) and the evolution of larval habitats. Molecular Phylogenetics and Evolution, 66(3), 833–846. (2013). https://doi.org/10.1016/j.ympev.2012.11.008
CrossRef - Pacelli, C., Cassaro, A., Maturilli, A., Timperio, A. M., Gevi, F., Cavalazzi, B., Stefan, M., Ghica, D., & Onofri, S. Multidisciplinary characterization of melanin pigments from the black fungus Cryomyces antarcticus. Applied Microbiology and Biotechnology, 104(14), 6385–6395. (2020). https://doi.org/10.1007/s00253-020-10666-0
CrossRef








