Manuscript accepted on :12-03-2026
Published online on: 18-03-2026
Plagiarism Check: Yes
Reviewed by: Dr. M Mohan Varma and Dr. Nasir Abdelrafie
Second Review by: Dr. Faheema Jabbar Aboalhor
Final Approval by: Dr. Prabhishek Singh
Madyha Hassan Mahmoud1 , Kamal Upreti2
, Kamal Upreti2 , Mohammed Abdullah Jeraiby3
, Mohammed Abdullah Jeraiby3 , Rituraj Jain4*
, Rituraj Jain4* , Yahia Mjery1
, Yahia Mjery1 , Mahdi Mohammed Alnajai5
, Mahdi Mohammed Alnajai5 , Fozia Siddiq Otaif1
, Fozia Siddiq Otaif1 and Mohammad Shane Alam1
and Mohammad Shane Alam1
1Department of Medical Laboratory Technology, College of Nursing and Health Sciences, Jazan University, Jazan, Saudi Arabia.
2Department of Computer Science, Christ University, Delhi NCR Campus, Ghaziabad, India.
3Department of Basic Medical Science, College of Medicine, Jazan University, Jazan, Saudi Arabia.
4Department of Information Technology, Marwadi University, Rajkot, Gujarat, India.
5Laboratory Department, Jazan University Hospital, Jazan University, Jazan, Saudi Arabia.
Corresponding Author E-mail: jainrituraj@yahoo.com
DOI : https://dx.doi.org/10.13005/bpj/3385
Abstract
Helicobacter pylori (H. pylori) is a common gastric pathogen that is linked to peptic ulcers, gastric cancer and systemic disorders. There is emerging evidence of an association between infection with H. pylori and chronic kidney disease and non-alcoholic hepatic steatosis, and possible renal and hepatic involvement. This study was conducted to assess the relationship between H. pylori and kidney and liver function changes in Saudi Arabian people. Blood samples were collected from 82 participants divided into two groups, namely H. pylori-infected and non-infected. Biochemical analyses were done to determine kidney (creatinine, urea, sodium and potassium) and liver function (ALT, AST, ALP, total protein and albumin). A total of 82 participants were included in the study, of whom 42 (51.2%) tested positive for Helicobacter pylori infection, while 40 (48.8%) were non-infected and served as the control group. Liver enzyme levels (ALP (64.00), AST (21.40), ALT (21.26) and GGT (20.78)) were normal and did not differ significantly between groups (p > 0.05). Regression analysis showed a significant relationship between H. pylori infection and high creatinine (OR = 6.38, p = 0.018). Borderline correlations were found for GGT (OR = 1.179, p = 0.092), uric acid (OR = 2.661, p = 0.061), and the electrolytes and lipid profiles showed no significant variation. H. pylori infection was significantly related to elevated creatinine levels, and may be affecting renal function. Most liver and electrolyte parameters were not affected. Further studies with larger cohorts are required in order to confirm these findings.
Keywords
Gastric infection; Helicobacter pylori; Kidney function test; Liver function test; Non-alcoholic fatty liver disease
Download this article as:| Copy the following to cite this article: Mahmoud M. H, Upreti K, Jeraiby M. A, Jain R, Mjery Y, Alnajai M. M, Otaif F. S, Alam M. S. The Impact of Helicobacter Pylori Infection on Renal and Hepatic Function Parameters in Saudi Arabi, A Case-Control Study. Biomed Pharmacol J 2026;19(1). |
| Copy the following to cite this URL: Mahmoud M. H, Upreti K, Jeraiby M. A, Jain R, Mjery Y, Alnajai M. M, Otaif F. S, Alam M. S. The Impact of Helicobacter Pylori Infection on Renal and Hepatic Function Parameters in Saudi Arabi, A Case-Control Study. Biomed Pharmacol J 2026;19(1). Available from: https://bit.ly/4rCcZHO |
Introduction
A gram-negative, spiral, microaerobic, microscopic bacterium, Helicobacter pylori is a bacterium that inhabits the gastric lining of a human stomach and reproduces in the mucus layer.1 It is found almost in half of the world population, and its prevalence has been reported to be more abundant in developing nations and those in low socioeconomic status.2 The route of transmission is mostly the fecal-oral route that happens by contaminated food and water, but oral-oral transmission that is facilitated by saliva and vomitus has also been reported.3,4 H. pylori has been designated as a Group 1 carcinogen by the International Agency for Research on Cancer because of its role in the pathogenesis of chronic gastritis, peptic ulcer disease, and gastric adenocarcinoma.5 It is still among the major etiological factors of upper gastrointestinal illness and a major cause of death that is related to gastric cancer across the globe.6,7 The wide range of gastric and extragastric illnesses that is related to the infection of H. pylori is summarized in Figure 1.
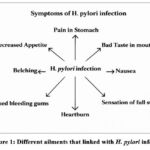 |
Figure 1: Different ailments that linked with H. pylori infectionClick here to view Figure |
In addition to its established gastric role, there is mounting evidence to indicate H. pylori infection can have a systemic effect by providing low-grade inflammation, oxidative stress, and immune activation. Nutritional, hygienic, behavioral, and socioeconomic factors have been defined as some of the determinants of infection risk to the epidemiological investigations.8,9 The determinants in the form of these influencing factors are depicted in Figure 2. The prevalence is reportedly highly heterogeneous in Saudi Arabia, with the highest percentage of 96 or 10.2 because of the heterogeneity of the population and the environment.9 This high prevalence highlights the importance of discovering the possible extragastric impact in this population.
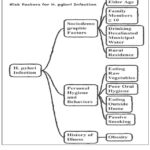 |
Figure 2: various factors that influence the H. pylori in infectionClick here to view Figure |
There is an emerging evidence that H. pylori infection can be a cause of renal pathology. It has been reported to have associations with diabetic nephropathy, membranous nephropathy, Henoch-Schonlein purpura nephritis and immunoglobulin A nephropathy.10 The observational studies also indicate that infected persons might have an increased risk of further renal impairment than the non-infected controls.11 It suggests immune complex deposition, endothelial dysfunction, systemic cytokine release, and vascular inflammation as the proposed pathophysiological mechanisms that may damage the integrity of glomeruli and the dynamics of renal filtration.12 Despite the conflicting results, these observations suggest the possibilities that chronic H. pylori infection may be a systemic inflammatory regulator of renal biochemical parameters. Equally, hepatic involvement has been researched more. Systemic oxidative stress, inflammatory cytokine, and immune dysregulation have been linked to chronic H. pylori infection and could result in non-alcoholic fatty liver disease (NAFLD), cirrhosis, and potentially hepatocellular carcinoma.12,13 Among the metabolic dysfunctions associated with the infection, there are insulin resistance and metabolic syndrome, which are central to NAFLD pathogenesis.13 High concentrations of pro-inflammatory cytokines like tumor necrosis factor-alpha (TNF-a) can contribute to the increased inflammation of the hepatic tissue, and low adiponectin concentrations can induce lipid deposition in hepatocytes.14 Moreover, the change in the composition of gut microbiota caused by the infection with H. pylori can promote systemic inflammation and increase hepatic metabolic imbalance.15 Although increasing evidence has been provided on such extragastric manifestations, objective biochemical assessment of renal and hepatic parameters among the infected individuals remains scanty especially among the population of the Middle East. Knowledge of the presence of quantifiable changes in kidney and liver functional tests in association with infection would help give knowledge about early involvement of the systemic conditions and translation to humans. Thus, the current research was carried out to determine the association between H. pylori infection and renal and hepatic biochemical levels in adult Saudi Arabians.
Materials and Methods
This analytical cross-sectional study was conducted between 2024 and 2025 at Jazan University Hospital and the College of Nursing and Health Sciences, Saudi Arabia, to investigate the association between Helicobacter pylori infection and renal and hepatic biochemical parameters. Ethical approval was obtained from the Local Committee for Research Ethics, Jazan University (Approval No.: REC-46/08/1378, dated 18 February 2025), and written informed consent was obtained from all participants.
A total of 82 adults aged 20–45 years were enrolled and categorized into two groups based on infection status: 42 H. pylori-positive individuals and 40 non-infected controls. Individuals with known hypertension, hepatitis B or C, chronic liver disease, chronic kidney disease, or current use of hepatotoxic or nephrotoxic medications were excluded to minimize confounding influences on biochemical parameters.
Diagnosis of Helicobacter pylori
Infection status was determined using the non-invasive ¹⁴C-Urea Breath Test (UBT) according to manufacturer guidelines (Anhui Jinren Medical Instrument Co., Ltd., China).16 Participants fasted for at least 3 hours before ingesting 1 µCi of ¹⁴C-urea dissolved in 30 mL of lukewarm water. After 15 minutes, breath samples were collected using a Breath Test Card and analyzed by a ¹⁴C-UBT analyzer to measure radioactivity expressed as disintegrations per minute (dpm). Infection was defined as:
Biochemical Assessment
Approximately 4 mL of venous blood was collected under aseptic conditions and centrifuged to obtain serum. Biochemical analyses were performed using the Beckman Coulter DXC 700 AU automated chemistry analyzer following calibrated enzymatic and colorimetric assay protocols.
Renal parameters included serum creatinine, urea, and uric acid. Hepatic parameters included alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), gamma-glutamyl transferase (GGT), total protein, and albumin. Electrolytes (Na⁺, K⁺, Cl⁻, phosphate, magnesium) and lipid profile markers (HDL, LDL, triglycerides) were also measured.
Serum creatinine concentration was interpreted as an indicator of glomerular filtration efficiency, where creatinine clearance is inversely related to renal impairment:
Statistical Analysis
Data were analyzed using IBM SPSS Statistics version 29. Continuous variables were expressed as mean ± standard deviation (SD), calculated as:
Group comparisons between infected and non-infected participants were performed using the Independent Samples t-test:
To evaluate independent associations between biochemical parameters and infection status, binary logistic regression was applied using the model:
where represents the probability of H. pylori infection and denotes predictor variables. Adjusted odds ratios (OR) were derived from:
A p-value < 0.05 was considered statistically significant.
Results
Our study assessed the relation between H. pylori Infection and kidney & liver function test in KSA (See Table 1)
Participants were recruited from adults attending Jazan University Hospital during the study period. Inclusion criteria included individuals aged 20–45 years who provided informed consent and underwent testing for Helicobacter pylori infection using the ¹⁴C-Urea Breath Test. Individuals with chronic liver disease, chronic kidney disease, hepatitis B or C, hypertension, or those using hepatotoxic or nephrotoxic medications were excluded to reduce confounding effects on biochemical parameters. Table 1 shows that a total of 82 individuals were included in this study, with females representing the majority (n=50, 61.0%) and males comprising the remainder (n=32, 39.0%). Regarding H. pylori test results, more than half of the participants tested positive (n=42, 51.2%), while the remaining tested negative (n=40, 48.8%).
Table 1: Gender Parameters and the H-Pylori Prevalence of participants
| Frequency N (%) | ||
| Gender | Female | 50 (61.0) |
| Male | 32 (39.0) | |
| H-Pylori Test among Patients | Negative | 40 (48.8) |
| Positive | 42 (51.2) | |
Table 2 shows the laboratory findings among participants, categorized by liver, renal/metabolic, electrolytes/minerals, and lipid parameters. Liver enzymes such as ALP (mean = 64.00, SD = 25.31), AST (mean = 21.40, SD = 13.14), ALT (mean = 21.26, SD = 12.14), and GGT (mean = 20.78, SD = 16.95) were all within normal adult reference ranges, indicating no overt hepatic dysfunction. Similarly, albumin (mean= 4.36g/dL) and total protein (mean= 7.44g/dL) were within expected limits. For renal/metabolic markers, creatinine (mean=0.78 mg/dL) and uric acid (mean=5.12 mg/dL) were within normal limits, although urea (mean=23.63 mg/dL) was higher than the usual upper limit and therefore evidence for early renal strain or a dietary influence for this case may be applicable. Electrolytes were relatively normal except for chloride (mean 112.4 mmol/L) which was higher than usual and further exploration was necessary. Lipid profile showed desirable level of HDL (mean = 54.36 (mg/dL)) but LDL (mean = 122.83 (mg/dL)) was above the optimal level indicating potential cardiovascular risk.
Table 2: Labs Parameters among the Participants
| System | Labs | Mean (SD) | Observed Range | Typical Adult Normal Range † |
| Liver‑function | ALP (U/L) | 64.00 (25.31) | 30 – 128 | 40 – 129 |
| AST (U/L) | 21.40 (13.14) | 6.8 – 65.0 | 5 – 34 | |
| ALT (U/L) | 21.26 (12.14) | 7.7 – 72.5 | 5 – 40 | |
| GGT (U/L) | 20.78 (16.95) | 7.7 – 75.0 | 7 – 49 | |
| Albumin (g/dL) | 4.36 (0.34) | 3.37 – 4.90 | 3.5 – 5.0 | |
| Total Protein (g/dL) | 7.44 (0.52) | 6.30 – 8.48 | 6.3 – 8.2 | |
| Renal / Metabolic | Urea (mg/dL) | 23.63 (9.55) | 4.97 – 52.98 | 7 – 20 |
| Creatinine (mg/dL) | 0.78 (0.23) | 0.18 – 1.27 | 0.6 1.2 | |
| Uric Acid (mg/dL) | 5.12 (1.26) | 3.14 – 6.70 | 3.4 –7.0 | |
| Electrolytes & Minerals | Sodium (mmol/L) | 138.24 (4.24) | 116 – 144 | 135 145 |
| Potassium (mmol/L) | 4.16 (0.44) | 3.5 – 6.1 | 3.5 – 5.1 | |
| Chloride (mmol/L) | 112.4 (38.74) | 101 – 306 | 98 – 107 | |
| Phosphate (mg/dL) | 3.59 (0.82) | 1.21 – 5.50 | 2.5 – 4.5 | |
| Magnesium (mg/dL) | 1.98 (0.15) | 1.71 – 2.30 | 1.7 – 2.2 | |
| Lipid Profile | HDL (mg/dL) | 54.36 (14.83) | 33.64 – 97.00 | ≥ 40 |
| LDL (mg/dL) | 122.83 (26.97) | 63 – 164 | < 100 optimal | |
| Triglycerides (mg/dL) | 91.41 (39.00) | 44 – 179.79 | < 150 |
Table 3 presents the correlation between the presence or absence of H pylori infection with kidney and liver function test results. Participants who were positive for H. pylori had slightly lower mean values for liver enzymes: ALP (62.82 U/L vs. 65.25 U/L), AST (20.39 U/L vs. 22.46 U/L), ALT (19.79 U/L vs. 22.80 U/L) and GGT (19.86 U/L vs. 21.41 U/L) than participants who were negative for H. pylori but none of these differences were statistically significant (p > 0.05). Similarly, kidney function markers such as urea (23.00 mg/dL vs. 24.23 mg/dL), creatinine (0.78 mg/dL vs. 0.79 mg/dL) and uric acid (5.05 mg/dL vs. 5.16 mg/dL), also showed no significant differences. Electrolyte and mineral levels such as sodium, potassium, chloride, phosphate and magnesium had minimal variation between groups with no significant associations. Lipid profile parameters such as HDL, LDL and triglycerides were also found not to show significant difference between the two groups. Overall, H. pylori infection was not related to abnormal kidney or liver function in this sample.
Table 3: Relation between Helicobacter Pylori Infection & Kidney & Liver function Test
| System | Lab | H-Pylori Test | ± Sig.Values | |
| NegativeMean (SD) | PositiveMean (SD) | |||
| LFT | ALP (U/L) | 65.25 (18.44) | 62.82 (30.93) | 0.769 |
| AST (U/L) | 22.46 (17.96) | 20.39 (6.14) | 0.629 | |
| ALT (U/L) | 22.80 (13.34) | 19.79 (11.01) | 0.343 | |
| GGT (U/L) | 21.41 (19.04) | 19.86 (14.20) | 0.821 | |
| Total Protein (g/dL) | 7.46 (0.51) | 7.42 (0.56) | 0.441 | |
| Albumin (g/dL) | 4.30 (0.39) | 4.43 (0.26) | 0.212 | |
|
RFT |
Urea (mg/dL) | 24.23 (12.21) | 23.00 (5.88) | 0.456 |
| Creatinine (mg/dL) | 0.79 (0.21) | 0.78 (0.25) | 0.711 | |
| Uric Acid (mg/dL) | 5.16 (1.24) | 5.05 (1.37) | 0.935 | |
| Electrolytes & Minerals | Na (mmol/L) | 137.72 (5.53) | 138.78 (2.23) | 0.822 |
| K (mmol/L) | 4.08 (0.29) | 4.25 (0.55) | 0.856 | |
| Cl (mmol/L) | 117.13 (50.42) | 105.55 (1.51) | 0.365 | |
| Phosphate (mg/dL) | 3.44 (0.83) | 3.84 (0.79) | 0.256 | |
| Magnesium (mg/dL) | 1.99 (0.17) | 1.97 (0.14) | 0.710 | |
| Lipid Profile | HDL (mg/dL) | 58.33 (18.51) | 52.10 (12.47) | 0.356 |
| LDL (mg/dL) | 121.29 (36.16) | 123.91 (20.46) | 0.851 | |
| Triglycerides (mg/dL) | 80.43 (33.93) | 97.33 (41.53) | 0.369 | |
(±) Independent T Test
Table 4 discusses liver function test values with respect to infection by H. pylori. Whilst none of the predictors were statistically significant, important trends suggested that H. pylori infection may affect liver enzyme profile. Specifically, higher levels of GGT were associated with higher odds of H. pylori infection (OR=1.179, 95% CI: 0.974-1.428), and this indicates that infection may increase GGT, however, the association was borderline (p=0.092). AST also displayed a positive association (OR = 1.091) and it may be possible that infection is associated with elevated AST levels. In contrast, ALT showed an inverse relationship (OR= 0.739, 95% CI: .482-1.133) indicating that H. pylori may be associated with lower levels of ALT. Other markers such as ALP, albumin and total protein did not show any significant predictive value.
Table 4: LFT’s as the Adjusted Predictor of Helicobacter-Pylori Infection
| B | Sig. | Exp(B) | 95% CI | ||
| Lower | Upper | ||||
| ALP (U/L) | -.013 | .790 | .987 | .898 | 1.085 |
| AST (U/L) | .087 | .191 | 1.091 | .958 | 1.243 |
| ALT (U/L) | -.303 | .165 | .739 | .482 | 1.133 |
| GGT (U/L) | .165 | .092 | 1.179 | .974 | 1.428 |
| Albumin (g/dL) | .433 | .810 | 1.542 | .045 | 52.572 |
| Total Protein (g/dL) | 2.922 | .368 | 18.571 | .032 | 10737.659 |
| Constant | -15.327 | .223 | .000 | ||
The adjusted renal function predictors of H. pylori infection are shown in Table 5. Notably, creatinine was a significant predictor (B=15.670, p=0.018), with an odds ratio of 6.38 (95% CI: 1.50-27.20), so people infected with H. pylori are more than six times likely to have high creatinine levels, which may indicate an association between H. pylori infection and impaired renal function. Uric acid was also found to be positively associated with H. pylori (OR 2.661, p 0.061), suggesting an association with an increased uric acid level of infected individuals, although it was not statistically significant. On the other hand, urea was negatively linked to H. pylori infection (OR = 0.880, p = 0.173), with a possible tendency toward reduced urea levels, but again non-significant.
Table 5: RFT’s as the Adjusted Predictor of Helicobacter-Pylori Infection
| B | Sig. | Exp(B) | 95% CI | ||
| Lower | Upper | ||||
| Urea (mg/dL) | -.128 | .173 | .880 | .731 | 1.058 |
| Creatinine (mg/dL) | 15.670 | .018 | 6.38 | 1.4992 | 27.20 |
| Uric Acid (mg/dL) | .979 | .061 | 2.661 | .954 | 7.423 |
| Constant | -6.862 | .038 | .001 | ||
Table 6 shows the electrolytes and mineral levels as adjusted predictors of Helicobacter pylori infection. None of the parameters were statistically significant (all p values > 0.05), but some trends are interesting. Potassium had a significant positive association (OR = 5.93, p = 0.255) indicating that infection by H. pylori may be associated with higher odds of having higher levels of potassium, though the confidence interval (0.277 to 126.805) was wide (high) due to high levels of uncertainty. Magnesium also had an increased odds ratio (OR = 1.97), but with very imprecise results (95% CI: 0.000-9670.096; p = 0.875), making the finding statistically unreliable. Chloride showed a negative association (OR = 0.552, p = 0.104) and may show a tendency towards lower values in case of H. pylori-positive individuals. Similarly, phosphate was inversely related (OR=0.150) (although not significantly p=0.272). Sodium levels (OR 0.996, p 0.973) showed no meaningful effect.
Table 6: Electrolytes & Minerals Labs as the Adjusted Predictor of Helicobacter-Pylori Infection
| B | Sig. | Exp(B) | 95% CI | ||
| Lower | Upper | ||||
| Na (mmol/L) | -.004 | .973 | .996 | 779 | 1.273 |
| K (mmol/L) | 1.780 | .255 | 5.927 | .277 | 126.805 |
| Cl (mmol/L) | -.594 | .104 | .552 | .270 | 1.129 |
| Phosphate (mg/dL) | -1.900 | .272 | .150 | .005 | 4.427 |
| Magnesium (mg/dL) | .679 | .875 | 1.972 | .000 | 9670.096 |
| Constant | 60.418 | .185 | 1.7*1016 | ||
Table 7 shows the adjusted effect of lipid profile parameters on Helicobacter pylori infection. Triglycerides showed a positive association (OR = 1.047, p = 0.149), suggesting that H. pylori infection may increase the odds of elevated triglyceride levels, though this did not reach statistical significance. HDL also had a slight positive association (OR = 1.015, p = 0.786), implying marginally higher HDL levels in infected individuals. In contrast, LDL demonstrated a weak negative association (OR = 0.988, p = 0.709), indicating a trend toward lower LDL levels among those with H. pylori.
Table 7: Lipid Profile as the Adjusted Predictor of Helicobacter-Pylori Infection
| B | Sig. | Exp(B) | 95% CI | ||
| Lower | Upper | ||||
| HDL (mg/dL) | .014 | .786 | 1.015 | .915 | 1.125 |
| LDL (mg/dL) | -.012 | .709 | .988 | .927 | 1.053 |
| Triglycerides (mg/dL) | .046 | .149 | 1.047 | .984 | 1.114 |
| Constant | -4.142 | .349 | .016 | ||
Discussion
Helicobacter pylori is a Gram-negative pathogenic organism which colonizesn the gastric mucosa and is mainly transmitted by fecal-oral or direct contact routes.17 It has been well characterized as affecting the gastrointestinal system, especially gastritis, peptic ulcer disease, and gastric malignancy,18,19 but increasing evidence indicates that chronic infection can have systemic inflammatory and metabolic effects outside the stomach.12,13 The current research tested the relationship between the infection with H. pylori and the biochemical measures that assess hepatic and renal functions in a group of Saudis. The major result was that there was a significant correlation between the infection status and the high serum creatinine with no statistically significant differences in hepatic enzymes, electrolyte balance, and lipid parameters between the groups.
Hepatic Biochemical Parameters and Inflammatory Modulation
In the present study, the serum levels of ALP, AST, ALT and GGT were within the normal ranges of the reference ranges of both the infected and the non-infected subjects. Even though it was found that slightly lower mean values are obtained in H. pylori-positive individuals these differences were not statistically significant. A logistic regression analysis also established the lack of significant independent relationship between infection status and hepatic enzyme changes. The results are in line with the earlier reports that have shown varied and dissimilar hepatic involvement in H. pylori infection. As is found, the direct bilirubin levels of NAFLD were found to be increased among infected individuals, but ALT and total bilirubin did not change, indicating a possible hepatic inflammation that was reversible with eradication therapy.20 This is also found to have been increased among infected individuals as opposed to an increase in ALT and total bilirubin, which implies that inflammation of the liver was selective and not a result of overt hepatocellular damage.15 Mechanistically, chronic H. pylori infection can trigger systemic cytokine release such as tumor necrosis factor-alpha (TNF-a) and interleukin-6 and oxidative mediators, which can lead to changes in hepatic lipid metabolism and insulin signaling pathways in otherwise healthy persons.13,14 But the lack of significant enzyme increase in our cohort indicates that infection may not be sufficient to cause observable hepatocellular injury in otherwise healthy persons. It may develop hepatic effects which are only clinically evident when combined with metabolic comorbid conditions like obesity or insulin resistance.
Renal Function and Creatinine Elevation
Unlike hepatic parameters, it was observed that H. pylori infection was statistically related with high serum creatinine level. Logistic regression analysis revealed that those with the infection were more than six times more likely to be having an elevated creatinine than the controls who were not infected. This observation indicates the possibility of the correlation of chronic infection with early renal functional change. Past studies have also reported the correlations between H. pylori and renal impairment. it is identified a correlation between H. pylori infection and diminished estimated glomerular filtration rate (eGFR).21 it is also demonstrated a correlation between active infection and elevated albumin-creatinine ratio, which supports the hypothesis that H. pylori can be a cause of glomerular injury.12 The pathophysiological processes behind this association could be a systemic inflammation that is chronic, endothelial dysfunction, and deposition of immune complexes. The sustained cytokine stimulation of the process may lead to the endothelial injury of the vascular structures and microcirculatory impairment of the glomerulus, which may compromise filtration efficiency.12 It has also been suggested, that molecular mimicry and immune-mediated processes are contributory factors to nephropathy in the infected individuals. The increased creatinine observed in this study could thus be an early indication of biochemical evidence of subclinical renal involvement. Although the independent sample t-test did not reveal a statistically significant difference in mean creatinine levels between infected and non-infected groups, logistic regression analysis identified creatinine as a significant predictor of H. pylori infection. This difference may arise because regression analysis evaluates the association between creatinine values and infection probability across the entire dataset rather than relying solely on group mean comparisons.
Electrolyte and Mineral Homeostasis
The electrolyte and mineral parameters analysis did not show statistically significant relations with the infection status. Despite some small trends to be noticed especially the ones with potassium and chloride levels, they were not significant. Such results are inconsistent with the reported results, which found the concentration of sodium, potassium, and chloride to be significantly lower in infected people.22 Study variation can be related to differences in study groups, severity of infection, comorbidity, or sample size. The fact that there was no electrolyte imbalance in our study indicates that simple H. pylori infection might not have any significant implication on systemic mineral homeostasis.
Lipid Profile and Metabolic Implications
The current research has no substantial linking between the presence of H. pylori infection and the lipid parameters such as HDL levels, LDL levels or triglycerides. Though triglycerides had a weak positive trend and LDL was weakly negative with people who are infected, these results were not statistically important. These findings are contrary to the meta-analysis where the LDL and total cholesterol levels were found to be higher and the HDL levels were reduced among infected groups.23 This difference could be related to the difference in demography, or metabolic conditions of the individuals, nutritional factors or methodological error. Perhaps, dyslipidemia in H. pylori is more intense in the population with developed metabolic syndrome than in quite healthy groups.
Clinical and Translational Implications
The clinical implication of this study that is of the most clinical interest is the correlation between the presence of the H. pylori infection and the high serum creatinine. Even though the causation is not possible because of the cross-sectional design, the information indicates the presence of a possible role of chronic infection in subtle changes of renal functional alterations. Providing these results are validated in longitudinal studies, these findings may justify regular monitoring of renal biomarkers in infected people. Moreover, prospective interventional research that quantifies renal functioning prior to and post eradication treatment can help to determine whether a renal shift because of infection is reversible, thus enhancing the translational applicability of the findings.
Limitations
There are several limitations of this study. The cross-sectional design of this study prevents the establishment of the causal relationships between the Helicobacter pylori infection and the changes in the liver or kidney function. The confounding variables like the dietary habits, comorbid conditions, medication use, and the lifestyle factors were also did not controlled in this study which could influence the lab parameters in participants. Additionally, this study did not assess the duration or severity of the H. pylori infection, which may impact the biochemical outcomes. Finally, single-center data limits population-wide applicability across Saudi Arabia.
Conclusion
The current research indicates that serum creatinine level is closely related to Helicobacter pylori infection, and thus there is a possibility of the existence of a relationship between chronic gastric infection and the early changes in renal functional activity. Although hepatic enzymes, electrolyte balance, and lipid parameters did not demonstrate any significant changes between infected and non-infected people, the observed renal association demonstrates the potential of subclinical systemic involvement by inflammatory or endothelial mechanisms. The evidence confirms this idea that the H. pylori infection can go beyond the localized gastric pathology and have quantifiable biochemical impacts on renal physiology. Even though the study cannot be said to be causal because it is cross-sectional in nature, the findings should not be ignored to indicate that longitudinal and interventional studies are required to communicate that eradication therapy can alleviate renal changes associated with infection. The potential clinical and translational relevant outcome of renal biomarker changes in infected individuals could be achieved through early detection.
Acknowledgement
The authors would like to express their sincere gratitude to the administration of Jazan University and Jazan University Hospital for providing laboratory facilities and institutional support for conducting this study. The authors also thank all participants who voluntarily contributed to this research. Their cooperation and participation were essential for the successful completion of this work.
Funding Sources
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflict of Interest
The author(s) do not have any conflict of interest
Data Availability Statement
This statement does not apply to this article
Ethics Statement
Ethical approval was granted by the Local Committee for Research Ethics, Jazan University (REC-46/08/1378; 18 February 2025). Written informed consent was obtained from all participants. No animal subjects were involved.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Clinical Trial Registration
This research does not involve any clinical trials.
Permission to reproduce material from other sources
Not Applicable
Author Contributions
- Madyha H. Mahmoud: Conceptualization, Methodology, Formal Analysis, Writing – Original Draft, Validation.
- Kamal Upreti: Conceptualization, Statistical Analysis, Methodology, Writing – Review & Editing, Supervision.
- Mohammed Abdullah Jeraiby: Investigation, Data Collection, Validation, Writing – Review & Editing.
- Rituraj Jain: Data Curation, Visualization, Statistical Interpretation, Writing – Review & Editing.
- Yahia Mjery: Investigation, Laboratory Analysis, Validation, Writing – Review & Editing.
- Mahdi Mohammed Alnajai: Resources, Laboratory Supervision, Data Verification.
- Fozia S. Otaif: Data Collection, Literature Review, Writing – Review & Editing.
- Mohammad Shane Alam: Supervision, Project Administration, Critical Revision of the Manuscript.
References
- Hooi JKY, Lai WY, Ng WK, et al. Global prevalence of Helicobacter pylori infection: systematic review and meta-analysis. Gastroenterology. 2017;153(2):420-429. doi:10.1053/j.gastro.2017.04.022
CrossRef - Mitchell H, Katelaris P. Epidemiology, clinical impacts and current clinical management of Helicobacter pylori infection. Med J Aust. 2016;204(10):376-380. doi:10.5694/mja16.00104
CrossRef - Diaconu S, Predescu A, Moldoveanu A, Pop CS, Fierbințeanu-Braticevici C. Helicobacter pylori infection: old and new. J Med Life. 2017;10(2):112-117.
- Amaral O, Fernandes I, Veiga N, et al. Living conditions and Helicobacter pylori in adults. Biomed Res Int. 2017;2017:9082716. doi:10.1155/2017/9082716
CrossRef - International Agency for Research on Cancer. Schistosomes, Liver Flukes and Helicobacter pylori. IARC; 1994. IARC Monogr Eval Carcinog Risks Hum. Vol 61.
- Moss SF. The clinical evidence linking Helicobacter pylori to gastric cancer. Cell Mol Gastroenterol Hepatol. 2017;3(2):183-191. doi:10.1016/j.jcmgh.2016.12.001
CrossRef - Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide. CA Cancer J Clin. 2021;71(3):209-249. doi:10.3322/caac.21660
CrossRef - Shu L, Zheng PF, Zhang XY, Feng YL. Dietary patterns and Helicobacter pylori infection in Chinese adults aged 45-59 years. Medicine (Baltimore). 2019;98(2):e14113. doi:10.1097/MD.0000000000014113
CrossRef - Monno R, De Laurentiis V, Trerotoli P, Roselli AM, Ierardi E, Portincasa P. Helicobacter pylori infection: association with dietary habits and socioeconomic conditions. Clin Res Hepatol Gastroenterol. 2019;43(5):603-607. doi:10.1016/j.clinre.2018.10.002
CrossRef - Kountouras J, Papaefthymiou A, Polyzos S. A, Deretzi G, Vardaka E, Soteriades E. S, Tzitiridou-Chatzopoulou M, Gkolfakis P, Karafyllidou K and Doulberis M. Impact of Helicobacter pylori-related metabolic syndrome parameters on arterial hypertension. Microorganisms, 2021; 9(11): 2351. DOI: 10.3390/microorganisms9112351.
CrossRef - Hata K, Koyama T, Ozaki E, et al. Assessing the relationship between Helicobacter pylori and chronic kidney disease. Healthcare (Basel). 2021;9(2):162. doi:10.3390/healthcare9020162
CrossRef - Balat M, Fahmy Zanaty M, El-Antouny N, Ahmed H. Association between proteinuria and active Helicobacter pylori infection in non-diabetic patients. Zagazig Univ Med J. 2019;25(1):79-84.
CrossRef - Xu G, Ma S, Dong L, Mendez-Sanchez N, Li H, Qi X. Relationship of Helicobacter pylori infection with nonalcoholic fatty liver disease: a meta-analysis. Can J Gastroenterol Hepatol. 2023;2023:5521239. doi:10.1155/2023/5521239
CrossRef - Anozie EEB, Nwaogu LA, Iheme AI, Anozie AJI. Biochemical changes associated with H. pylori infection in humans. World J Adv Res Rev. 2024;22(1):1546-1556. doi:10.30574/wjarr.2024.22.1.1224
CrossRef - Abdulhamid A, Venkat D. Abnormal liver enzymes due to H. pylori infection. Am J Gastroenterol. 2018;113(Suppl):S1285.
CrossRef - Pan W, Zhang H, Wang L, et al. Association between Helicobacter pylori infection and kidney damage in patients with peptic ulcer. Ren Fail. 2019;41(1):1028-1034. doi:10.1080/0886022X.2019.1683029
CrossRef - Chen X, Fu J, Jin K, Yang Z, Qian Y, Mei K, Wang Y, Min J, Du Y, Zhu Z and Li S. Overweight and Helicobacter pylori infection: a correlation in metabolic dysfunction-associated fatty liver disease. Cell. Infect. Microbiol., 2025; 15: 1565298. DOI: 10.3389/fcimb.2025.1565298.
CrossRef - Elshair M, Ugai T, Oze I, et al. Impact of socioeconomic status and sibling number on Helicobacter pylori prevalence: a cross-sectional study. Nagoya J Med Sci. 2022;84(2):374-387. doi:10.18999/nagjms.84.2.374
- Reyes VE. Helicobacter pylori and its role in gastric cancer. Microorganisms. 2023;11(5):1312. doi:10.3390/microorganisms11051312
CrossRef - Chen C, Zhang C, Wang X, et al. Helicobacter pylori infection may increase NAFLD severity via metabolic and inflammatory pathways. Eur J Gastroenterol Hepatol. 2020;32(7):857-866. doi:10.1097/MEG.0000000000001601
CrossRef - Wang X, Jia Z, Zhang Y, Kou C, Jiang J. Association of Helicobacter pylori infection with estimated glomerular filtration rate. Infect Genet Evol. 2021;96:105102. doi:10.1016/j.meegid.2021.105102
CrossRef - Aburahma NNA, Kadhim NA. Changes of serum electrolytes and vitamin C levels in patients infected with Helicobacter pylori. Iraqi J Sci. 2023;64(8):3793-3798. doi:10.24996/ijs.2023.64.8.6
CrossRef - Gaonkar A, Zahiruddin QS, Shabil M, et al. Association of Helicobacter pylori infection and risk of dyslipidemia: a systematic review and meta-analysis. JGH Open. 2025;9(3). doi:10.1002/jgh3.70128
CrossRef
Abbreviations List
H. pylori – Helicobacter pylori, UBT – Urea Breath Test, ¹⁴C-UBT – Carbon-14 Urea Breath Test, ALT – Alanine Aminotransferase, AST – Aspartate Aminotransferase, ALP – Alkaline Phosphatase, GGT – Gamma-Glutamyl Transferase, LFT – Liver Function Test, RFT – Renal Function Test, Na⁺ – Sodium, K⁺ – Potassium, Cl⁻ – Chloride, HDL – High-Density Lipoprotein, LDL – Low-Density Lipoprotein, SD – Standard Deviation, OR – Odds Ratio, CI – Confidence Interval, eGFR – Estimated Glomerular Filtration Rate, TNF-α – Tumor Necrosis Factor Alpha, NAFLD – Non-Alcoholic Fatty Liver Disease, SPSS – Statistical Package for the Social Sciences, REC – Research Ethics Committee







