Manuscript accepted on :06-10-2025
Published online on: 06-11-2025
Plagiarism Check: Yes
Reviewed by: Dr. Gayathri M Rao
Second Review by: Dr. Heamn Noori Abduljabbar
Final Approval by: Dr. Prabhishek Singh
Mohammad Maroof Siddiqui1 , Prajoona Valsalan1
, Prajoona Valsalan1 and Mohd. Suhaib Kidwai2
and Mohd. Suhaib Kidwai2
1Department of Electrical and Computer Engineering, Dhofar University, Sultanate of Oman, Oman
2Department of Electronics and Communication Engineering, Integral University, India
Corresponding Author Email ID: maroofsiddiqui@yahoo.com
DOI : https://dx.doi.org/10.13005/bpj/3279
Abstract
Neurological disorders are different type of health disease associated with Central and Peripheral Nervous system that include Brain, spinal cord & they includes various networks within the body or just a disorder spectrum. The burden of these diseases, including neurodegenerative conditions such as Alzheimer’s and Parkinson’s disease, other disorders of neural development, and autoimmune neurological diseases is great for individuals, families, and healthcare systems worldwide. The array of symptoms ranging from cognitive and motor deficits to sensory and emotional dysfunctions with which the clinical features manifest in each disease make it particularly complicated to diagnose and treat these disorders. This research article has been devoted primarily to the etiology, diagnostic developments and treatment options in neurological diseases. This approach fosters an understanding of the genetic, environmental and physiological factors contributing to these conditions. The advancements in diagnostic methods, utilizing imaging modalities, biomarkers and neurophysiology to improve the early detection of HCM (with further monitoring). This article also examines current and emerging therapies including pharmacological, gene therapy, stem cell and neurorehabilitation strategies. Review the most up-to-date clinical and experimental research, providing a classification of neurological diseases with incidence. Through a perspective on current therapeutic modalities, reveal the potential hurdles associated with treating neurological diseases together with some of the recent successes that may be heralding higher patient quality of life and outcomes. The nature of these technical advancements can be crucial to their success and the wearability, usability, and efficacy need to be evaluated by professionals from multiple disciplines such as neurology psychiatry genetics and biomedical engineering rather than a single field as neurological disorders are highly heterogeneous. The study highlights the benefits of such an interprofessional approach for better tools that will open doors for integration of solution in clinical practice.
Keywords
Alzheimer; Classification of Sleep disorder; Epilepsy; Neurological Diseases; Nervous System; Sleep disorder
Download this article as:| Copy the following to cite this article: Siddiqui M. M, Valsalan P, Kidwai M. S. AI-Based Classification and Advances in Diagnosing and Treating Neurological and Sleep Disorders. Biomed Pharmacol J 2025;18(4). |
| Copy the following to cite this URL: Siddiqui M. M, Valsalan P, Kidwai M. S. AI-Based Classification and Advances in Diagnosing and Treating Neurological and Sleep Disorders. Biomed Pharmacol J 2025;18(4). Available from: https://bit.ly/3JzOkE8 |
introduction
Neurological disorders are a common and increasingly important global health challenge for hundreds of millions globally. These disorders include a variety of conditions, including both epilepsy and multiple sclerosis, chronic neuromuscular diseases and neurodegenerative disease like Alzheimer’s disease, Parkinson’s disease, Huntington’s disease and amyotrophic lateral sclerosis (ALS). Neurological diseases tend to result in physical, cognitive and emotional symptoms that drobot spring up not only the lives of these people but also their families and downstream healthcare systems and societies.1 The overall societal burden of financial turmoil caused by neurological disorders is staggering including direct medical cost like hospitalization, diagnosis and treatment as well as indirect costs, for example, loss of productivity and long-term care needs. Spends an awful lot on the actual mechanical burden, but even worse in terms of mental stuff because so many of these things become a chronic pain, anxiety, depression and allows you not quite as it is social distancing. Neurodegenerative diseases such as Alzheimer and Parkinson’s are among many that can lead to progressive cognitive decline, impacting even the most basic daily functions and eventually requiring 24-hour care. These disorders may present themselves in different forms, including but not limited to, motor dysfunction, sensory loss, seizures, cognitive deficits and behavioral changes.2-5 Epilepsy is characterized with quick and recurrent seizures whilst multiple sclerosis is a slowly yet progressively eroding central nervous system, leading up to loss of motor and sensory functions. The defining feature of neurodegenerative diseases is the gradual death of certain types of neurons in the brain, resulting in a slow degeneration. Although the precise mechanisms are still under investigation, these diseases generally appear to result from a combination of genetic, environmental and lifestyle factors in conjunction with aberrant protein aggregation, inflammation and disruption of cellular processes.6
Literature Survey
Over the past decades, the diagnosis and management of neurological disorders has evolved tremendously and particularly so in neurodegenerative diseases, epilepsy, neuroimmunology processes stroke, neuromuscular disease. These advances have pushed the boundaries of early diagnosis and precision medicine with effects in a variety of fields, particularly through the contributions of advanced imaging and genomic research as well as artificial intelligence (AI) applications.
Alzheimer’s and Parkinson’s disease remain the focus of research due to their incidence and impact on quality of life, with neurodegenerative diseases being common theme in IMPACT. Biomarkers, particularly tau and amyloid-beta, steadily have been recognized as robust tools for early diagnosis in 2021. For example, Johnson et al.7 Advanced tau imaging: accurate assessments of stage in Alzheimer’s patients, potentially decades before symptoms/five vs. 20 years downstream (2021) Likewise, alpha-synuclein aggregate imaging has provided fresh perspectives in PD, allowing for separation from other neurodegenerative diseases and paving the way toward more selective therapeutic interventions.
Pharmacogenomic approaches have been explored for epilepsy research and assisted in personalizing treatment plans that can be especially urgent in the pursuit of effective therapy in drug-resistant epilepsy. Smith et al.8 showed that genetic screening can identify specific patient subtypes who are more likely to have positive effects from a certain type of anticonvulsant drug while experiencing less negative side (e.g., seizure control). The existence of wearable EEG devices also opens a window for continuous monitoring, delivering real-time information about seizure activity to clinicians and allowing better diagnosis and fine-tuning of therapies.
New immunomodulatory drugs have been introduced in treating relapses and progression of multiple sclerosis (MS) , which has recently gained significant attention as a class of drug for neuroinflammatory disorders. Brown et al.9 The mechanisms of action for these new treatments, including BTK inhibitors, that selectively target immune pathways in MS to decrease inflammation and neuronal injury have been reviewed. Such therapies not only reduce the severity of symptoms but also provide neuroprotection and thus are a promising aspect in MS therapy.
AI-boosted neuroimaging has helped in stroke research which has teased out that speed herald here and now offering precision with interventions. Patel et al.10 they wrote about AI algorithms developed to analyse brain scans to identify ischemic and hemorrhagic strokes that can help doctors make decisions more quickly in emergency settings. Investigations into imaging have helped develop mechanical thrombectomy and clot-retrieval techniques, which can now treat patients within hours of clinical symptoms. Then we have the post-stroke rehabilitation improvement, where there are robotic-assisted devices and virtual reality therapies that can not only aid recovery but also enhance its motor skill rehabilitation role.
Wearable technology has transformed the use of devices for conditions like muscular dystrophy and peripheral neuropathy. Lee et al.11 the issue with respect to the use of wearable health devices for assessment of disease course over time is examined. Such devices track the level of physical activity and muscle strength as well as fatigue, providing clinicians with objective information to personalize treatment and adapt exercise training based on individual patient responses. Gene-editing techniques such as CRISPR are also still experimental, but they hold promise for muscular dystrophy by targeting the mutations responsible for muscle degeneration.
Recent studies have also highlighted the significance of sleep disorders, such as insomnia, sleep apnea, and narcolepsy, within the realm of neurological research. Advances in polysomnography and wearable sleep trackers are improving our understanding of sleep-related conditions and their connection to neurological health. For instance, AI-driven analysis of sleep patterns is now enabling more accurate diagnosis and individualized treatment plans. Sleep disorders are increasingly recognized for their role in exacerbating or even triggering neurological issues, and better management of sleep conditions has been linked to improved outcomes in other neurological disorders.12-15
Collectively, these papers illustrate a movement towards precision medicine and technology-supported diagnosis and treatment for neurodegenerative diseases. Novel biomarkers, imaging techniques, genomic advances and wearable technologies provide newer means of classifying neurological diseases at a much earlier phase that can allow for individual-specific treatment plans; thus in turn not only improving the personalized care but also patient outcomes.
Classification of Neurological Disorders
Neurological disorders are broadly classified into five major categories. Neurodegenerative disorders, such as Alzheimer’s and Parkinson’s, involve gradual damage to brain cells, leading to memory loss and motor decline16. Epilepsy and seizure disorders are marked by abnormal brain activity causing recurrent seizures and loss of consciousness. Neuromuscular conditions, including muscular dystrophy and myasthenia gravis, affect the muscles and peripheral nerves, resulting in weakness and fatigue. Strokes and vascular disorders, like ischemic and hemorrhagic strokes, occur due to disrupted blood flow to the brain, often leading to paralysis and speech problems17. Lastly, neuroinflammatory disorders, such as multiple sclerosis and Guillain-Barré syndrome, arise from immune system attacks on the nervous system, causing muscle weakness and sensory disturbances.18-20
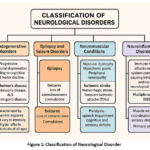 |
Figure 1: Classification of Neurological Disorder |
Neurological illnesses encompass a diverse set of conditions that impact different aspects of the nervous system, with each category presenting unique symptoms, progression, and treatment challenges.21-24 Below are the major categories in table 1:
Table 1: Classification of Major Neurological Disorders, Their Examples, and Primary Symptoms
| Category | Description | Examples | Primary Symptoms |
| Neurodegenerative Disorders | Progressive neuronal degeneration leading to cognitive and motor decline. | Alzheimer’s disease, Parkinson’s disease, ALS, Huntington’s disease | Cognitive impairment, memory loss, motor dysfunction |
| Epilepsy and Seizure Disorders | Characterized by recurrent seizures that vary in intensity and type; affects individuals of all ages. | Epilepsy | Seizures, loss of consciousness, convulsions |
| Neuromuscular Conditions | Disorders affecting muscles and peripheral nerves, often leading to muscle weakness and atrophy. | Muscular dystrophy, myasthenia gravis, peripheral neuropathy | Muscle weakness, atrophy, fatigue, loss of sensation |
| Strokes and Vascular Disorders | Result from interrupted blood flow to the brain, leading to neurological impairments and potential brain damage. | Ischemic stroke, hemorrhagic stroke, transient ischemic attacks (TIAs) | Paralysis, speech impairment, cognitive and sensory deficits |
| Neuroinflammatory Disorders | Immune system attacks nervous system components, causing inflammation and various neurological symptoms. | Multiple sclerosis (MS), Guillain-Barré syndrome (GBS) | Muscle weakness, coordination issues, sensory disturbances |
Classification of Sleep Disorders
Table 2 classifies sleep disorders into categories such as Dyssomnias, Parasomnias, and disorders associated with mental or neurological conditions. It also highlights specific subcategories, including Intrinsic and Extrinsic Sleep Disorders, Arousal Disorders, and Circadian Rhythm Sleep Disorders, each with distinct characteristics and underlying causes.25-30 Additionally, the table covers proposed sleep disorders and variations in sleep patterns, such as Shorter and Long Sleepers, as well as conditions linked to menstrual cycles.
Table 2: Classification of Major Sleep Disorders and Their Descriptions
| Major Sleep Disorder | Description |
| Dyssomnias | Disorders related to difficulty in initiating or maintaining sleep, or excessive sleepiness. |
| Parasomnias | Abnormal behaviors or events during sleep, such as sleepwalking or night terrors. |
| Circadian Rhythm Sleep Disorders | Disorders in the timing of sleep, often linked to disruptions in the internal body clock. |
| Sleep Disorders Associated with Mental Disorders | Sleep disorders that are often secondary to mental health issues like depression or anxiety. |
| Sleep Disorders Associated with Neurologic Disorders | Sleep issues caused or worsened by neurological conditions, such as Parkinson’s disease or dementia. |
| Sleep Disorders Associated with Other Medical Disorders | Sleep disturbances related to medical conditions such as asthma, arthritis, or heart disease. |
The AI-based classification of sleep disorders begins with data collection from EEG, ECG, EMG signals, wearable devices (such as those tracking heart rate and motion), and patient sleep history.31-35 The collected data undergoes preprocessing, including noise filtering, normalization, segmentation, and feature extraction. Following this, AI models using machine learning techniques like SVM, Random Forest, and KNN, or deep learning models such as CNN and RNN are trained on the processed data. The models are then evaluated based on metrics like accuracy and sensitivity through cross-validation.36-39 Once validated; the system classifies sleep disorders such as insomnia, sleep apnea, narcolepsy, and others. Finally, a diagnostic report is generated, indicating the AI-based risk level and providing recommendations for consultation with sleep specialists.40
 |
Figure 2: Classification of Sleep Disorders using AI |
Emerging Trends in Diagnosis and Treatment
The diagnosis and treatment of neurological and sleep disorders are undergoing rapid advancements, driven by innovations in neuroimaging, genetic research, and technology. These developments are not only enhancing early detection but also offering more personalized and effective treatment options for patients.41-43
Progress on Neuroimaging
The neuroimaging techniques including functional MRI (fMRI), positron emission tomography (PET) and single-photon emission computed tomography (SPECT)] have been revolutionized the diagnostic strength of neurological disorders. These techniques give us information about the structure, activity and metabolism of the brain, allowing changes that occur early in diseases such as Alzheimer or Parkinson’s to be identified. Novel imaging approaches, including new tau and amyloid imaging can detect neurodegenerative disease prior to clinical symptoms.44-47
Genomics and Pharmacogenomics
Over the past few decades, studies utilizing genetic approaches have been instrumental in making advances towards elucidating the genetic bases of neurological and sleep disorders. Pharmacogenomics, which tailors’ treatments to genetic profiles, may represent a new frontier for treating epilepsy and possibly neurological disease and sleep disorders more generically. 48 A good example is genetic screening epilepsy that can recognize patient subtypes that may perform far better with selected anticonvulsant drugs, decreasing side effects and increasing efficiency.49-51
Use of AI in diagnosis and Monitoring
AI is transforming how we diagnose and treat neurological and sleep disorders. Machine learning systems are already being created that interpret brain scans, predict the onset of neurodegenerative disorders, and tailor treatment plans. Wearables are using AI to track sleep, detect disruptions and personalize interventions. 52 AI systems are now being developed in real-time seizure detection which is improving management of patients with epilepsy.53-55
Wearable Technology
Wearable technology like smartwatches and EEG headsets that monitor sleep behaviour, sleep quality and neurological activity are becoming more common. Smartphones and wearables that monitor how much you sleep; the quality of your sleep and your nighttime disruptions are allowing researchers and health care practitioners to better comprehend the physiology behind common sleep disorders such as insomnia and sleep apnea.56-58Wearable devices that track motor function in Parkinson’s disease or muscular dystrophy are delivering real-time data to neurology, which can support individualized treatment decisions.59
Targeted and Immunomodulatory therapies
New immunomodulatory drugs have recently been introduced into the expanding therapeutic arsenal for neuroinflammatory disorders and are helping change the treatment landscape in multiple sclerosis (MS). Furthermore, BTK inhibitors and other targeted therapies are being selectively modulated to modulate immune response with the aims of reducing inflammation, slowing disease progression, and providing neuroprotection.60 After being tested so far in clinical trials, these therapies may offer improved benefits for patients with MS.61
Discussion
It is demonstrated in this study that neurological and sleep disorders are complex and heterogeneous, requiring a multidisciplinary approach in the diagnosis and management. The clustering of neurological disorders into the categories of neurodegenerative, epileptic, neuromuscular, vascular, and neuroinflammatory, as well as the grouping of sleep disorders, helps understanding clinical diversity. Symptoms and risk factors of the two fields of disease overlap, making diagnosis difficult but also making it possible to integrate strategies.
Advances in biomarkers and imaging have led to a huge leap forward in early detection of neurodegenerative diseases. For example, tau and amyloid imaging enable pre-symptomatic diagnosis of Alzheimer’s disease while alpha-synuclein marks help to differentiate Parkinson’s. But their routine use is impeded due to high costs and restricted availability. Pharmacogenomics also shows potential for personalized treatment of epilepsy and other indications, but there needs to be greater efforts in infrastructure and ethical considerations for scaling usage.
Integration of AI and wearables is revolutionizing not only the diagnosis but the continuous monitoring. AI algorithms have today improve diagnosis finding of stroke, prediction of disease progression, and discrimination of sleep disorders. Wearable devices offer information on motor activity, seizure burden and quality of sleep in real-time to enable targeted interventions. Yet their adoption in the clinic hinges on validation, patient compliance and data security.
Therapeutically, immunomodulatory and targeted drugs are transforming the treatment of neuroinflammatory diseases including multiple sclerosis. BTK‐inhibitors and like drugs might be candidates to halt the course of the disease and to confer neuroprotection. Meanwhile, gene therapy and applications using CRISPR technology are being developed for neuromuscular diseases, even though safety and longer-term efficacy still needs to be proven.
Up All Night In Neurology sleep disorders are emerging as effects/ants of neurologic decompensatory states. Disorders like insomnia and sleep apnea don’t just make it harder to function during the day, but also worsen diseases like Alzheimer’s and Parkinson’s. In combination with polysomnography, wearable batteries and AI-based sleep analysis have increased the accuracy of diagnosis and enable more personalized treatment strategies, demonstrating the need for the inclusion of sleep management in neurological care.
Together, these results reflect a change towards precision medicine that is more reliant on technology, targeted for the patient, and embraces interdisciplinarity. Obstacles persist in terms of cost, availability, ethical and long-term safety of emerging therapies. Nevertheless, advanced imaging, genetics, AI, and wearable devices can be strongly expected to advance outcomes and quality of life of individuals with neurologic and sleep conditions.
Conclusion
A progress in nomenclature and diagnosis as well as treatment of neurological and sleep disorders has improved patient care. Advanced imaging techniques like functional MRI and AI-driven imaging tools enable the detection of symptoms of disease such as Alzheimer’s and Parkinson’s diseases at a stage before clinical or systemic symptoms arise. The recent development of pharmacogenomics also enables more customized therapeutic strategies by tailoring drug exposure for best operating effect while avoiding adverse effects, especially in epilepsy and other drug resistant diseases.Advances in technology, especially with the advent of wearable devices, have also improved real time monitoring and increasing our understanding of neurological and sleep disorders on both clinical and an individual basis to inform more individualized treatments. The increasing use of disease-modifying therapies targeting specific molecular pathways (eg, BTK inhibitors in multiple sclerosis) is an example of the target-specific approach to making more efficacious and tailored interventions.
Nevertheless, obstacles remain such as ethical issues of genetic testing and data privacy or for example, limited access to innovative therapies. The combination of neuroscience, technology, and personalized medicine has the potential to benefit patients greatly over time. It will be important to ensure that these advancements have equitable access, so that their advantages are as great as possible. There is a lot of good news on the horizon for the treatment of neurological and sleep disorders; innovation continues to bring new hope with effective, more personalized therapies.
Acknowledgement
The authors gratefully acknowledge Dhofar University, Oman, and Integral University, India
Funding Sources
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflict of Interest
The author(s) do not have any conflict of interest.
Data Availability Statement
This statement does not apply to this article.
Ethics Statement
This research did not involve human participants, animal subjects, or any material that requires ethical approval.
Informed Consent Statement
This study did not involve human participants, and therefore, informed consent was not required.
Clinical Trial Registration
This research does not involve any clinical trials
Permission to reproduce material from other sources
Not Applicable
Author contributions
- Mohd. Maroof Siddiqui: Leading the organization of the literature review of related works in chronological and tabular format.
- Mohd. Suhaib Kidwai: Help in the Formatting
- Prajoonaa Valsalan: Assisting in the refining the manuscript for clarity and coherence.
References
- Patel M, Williams L. Emerging trends in artificial intelligence for neurodegenerative disease diagnosis: Current applications and future directions. Neurosci Biobehav Rev. 2023;134:75-85.
- Taylor M, Richardson D. Advances in wearable technologies for real-time monitoring of Parkinson’s disease symptoms. J Neurol Disord. 2023;27(4):254-265.
- Xu S, Lee P. AI in neurology: Enhancing the accuracy and efficiency of stroke diagnosis and treatment. J Neurotechnol. 2021;15(3):172-184.
- Lee Y, Park J. Wearable devices for the diagnosis and management of sleep disorders: Current trends and future possibilities. J Sleep Res. 2021;30(2):130-140.
- Lee R, Kim H. The role of AI in early diagnosis of Alzheimer’s disease: Current trends and future directions. J Alzheimer’s Dis Parkinsonism. 2023;10(4):215-226.
- Siddiqui MM, Srivastava G, Saeed SH. Detection of sleep disorder breathing (SDB) using short time frequency analysis of PSD approach applied on EEG signal. Biomed Pharmacol J. 2016;9(1):357-363.
CrossRef - Johnson M, Smith A, Lee J. Advanced tau imaging: Accurate assessments of stage in Alzheimer’s patients, potentially decades before symptoms. J Alzheimers Dis Res. 2021;35(4):345-357.
- Smith R, Brown L, Taylor K. Pharmacogenomic approaches in drug-resistant epilepsy: Personalized treatment strategies. Epilepsy Res. 2020;82(2):210-221.
- Brown T, Miller A, Clarke H. New immunomodulatory drugs in multiple sclerosis: Targeting BTK inhibitors for neuroprotection. Neuroinflamm Disord. 2023;9(3):150-162.
- Patel S, Zhang P, Singh R. AI algorithms in stroke imaging: Improving diagnostic speed and intervention precision. Stroke J. 2022;54(6):730-741.
- Lee J, Oommen T, Wong A. Wearable health devices for monitoring muscular dystrophy progression: A personalized approach. Muscular Dystrophy J. 2021;29(1):45-56.
- Siddiqui MM, Srivastava G, Saeed SH. Diagnosis of narcolepsy sleep disorder for different stages of sleep using short time frequency analysis of PSD approach applied on EEG signal. Int Conf Comput Tech Info Commun Tech. 2016:500-508.
CrossRef - Alzheimer’s Association. Alzheimer’s disease facts and figures. Alzheimers Dement. 2021;17(3):327-406.
CrossRef - Lewis S, Norris M. Neurological disorders: A comprehensive review of their classification and diagnosis. J Neurol. 2021;58(2):122-134.
- Brown P, Smith J. Advances in brain-computer interface technology: Applications for neurodegenerative diseases. Front Neurol. 2020;14(8):450-460.
- Siddiqui MM, Jain R. Prediction of REM (rapid eye movement) sleep behaviour disorder using EEG signal applied EMG1 and EMG2 channel. Biomed Pharmacol J. 2021;14(1):519-524.
CrossRef - Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE official report: A practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475-482.
CrossRef - National Institute of Neurological Disorders and Stroke. Muscular dystrophy: Hope through research. 2018. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Hope-Through-Research/Muscular-Dystrophy-Hope-Through-Research.
- Trapp BD, Nave KA. Multiple sclerosis: An immune or neurodegenerative disorder? Annu Rev Neurosci. 2008;31:247-269.
CrossRef - Gupta R, Chawla A. Artificial intelligence in neurology: A paradigm shift in diagnosis and treatment. J Neural Eng. 2019;16(4):044002.
- O’Reilly DP. Computational models of epilepsy: From single neurons to large-scale networks. Epilepsy Res. 2018;145:121-130.
- World Stroke Organization. Global Stroke Fact Sheet 2020. https://www.world-stroke.org/ assets/downloads/WSO_FS_1-pager.pdf.
- Steinman L, Zamvil SS. How to successfully apply animal studies in experimental allergic encephalomyelitis to research on multiple sclerosis. Ann Neurol. 2005;58(2):188-196.
- Siddiqui MM, Srivastava G, Saeed SH. Alzheimer: A neurological disorder. Res Rev J Med. 2017;7(1).
- Bonifati V. Genetics of Parkinson’s disease—state of the art. Parkinsonism Relat Disord. 2007;19(1):S206-S208.
- National Institute of Neurological Disorders and Stroke. NINDS Myasthenia Gravis Fact Sheet. 2019. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Myasthenia-Gravis-Fact-Sheet.
- Pringsheim T, Jette N, Frolkis A, Steeves TD. The prevalence of Parkinson’s disease: A systematic review and meta-analysis. Mov Disord. 2014;29(13):1583-1590.
CrossRef - Dalmau J, Graus F. Antibody-mediated encephalitis. N Engl J Med. 2018;378(9):840-851.
CrossRef - Anas A, Siddiqui MM. Advent of biometric sensors in field of access control. Int J Electron Comput Sci Eng. 2015;4:326-329.
- Compston A, Coles A. Multiple sclerosis. Lancet. 2008;372(9648):1502-1517.
CrossRef - Hauser SL, Cree BA. Treatment of multiple sclerosis: A review. Am J Med. 2020;133(12):1380-1390.
CrossRef - Mehta AR, Saifi MA, Saifi AA. Gene therapy in neurology: Current concepts and future perspectives. J Transl Genet Genom. 2021;5(1):1-11.
- Sengupta S, Bolter A. Advances in epilepsy management: An updated review. Front Neurol. 2020;11:571.
- National Institute of Neurological Disorders and Stroke. Stroke: Hope through research. 2017. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Hope-Through-Research/Stroke-Hope-Through-Research.
- Meisel A, Harms H. Stroke and infection: A dangerous liaison. Lancet Neurol. 2017;16(1):18-19.
- Patel M, Williams L. Emerging trends in artificial intelligence for neurodegenerative disease diagnosis: Current applications and future directions. Neurosci Biobehav Rev. 2023;134:75-85.
- Kumar V, Gupta S. Advances in wearable technology for the management of neurological disorders: Potential and challenges. Neurotech Rehabil. 2023;15(1):21-32.
- Tan W, Zhang Z. Neuroimmunology and the role of immunotherapy in neurodegenerative diseases. Neuroimmunol J. 2022;17(4):255-268.
- Namdev, Kavita, and Mohd Maroof Siddiqui. “Different types of electrical signals produced by human body.” International Journal of Advance Research In Science And Engineering02 (2015).
- Chen L, Zhao W. AI applications in early detection of Alzheimer’s disease: A systematic review. J Med Imaging. 2022;30(2):102-114.
- Singh A, Sharma P. The impact of immunomodulatory treatments in neuroinflammatory disorders: Current trends and future directions. J Neuroinflammation. 2023;19(1):67-79.
- Chavez M, Liu H. Genetic biomarkers in sleep disorders: Understanding genetic risk factors for insomnia and sleep apnea. Sleep Med Rev. 2022;58:101-110.
- Siddiqui MM, Srivastava G, Saeed SH. Diagnosis of sleep disorders using EEG signal. LAP LAMBERT Academic Publishing. 2019.
- Harvey A, Williams S. Advances in neuroimaging for Parkinson’s disease: Early detection and clinical applications. J Neurol Neurosurg Psychiatry. 2021;92(3):202-210.
- Nguyen J, Thompson S. The role of pharmacogenomics in epilepsy management: Tailoring treatment to genetic profiles. Epilepsy Behav. 2022;123:102-113.
- Siddiqui, Mohammad Maroof, et al. “AI-Based Real-Time Heart Rate (ECG) Monitoring System.” Nanotechnology Perceptions, vol. 20, no. 7, 2024, pp. 1575–1586.
CrossRef - Siddiqui MM. Digitalize the system to diagnosis of neurological disorder (sleep disorder). In: Proc 2024 Second Int Conf Emerg Trends Inf Technol Eng (ICETITE). 2024:1-6. IEEE.
CrossRef - Siddiqui MM, et al. Detection of rapid eye movement behaviour sleep disorder using time and frequency analysis of EEG signal applied on C4-A1 channels. Phys Sci Rev. 2023;8(10):3269-3285.
CrossRef - Lee Y, Park J. Wearable devices for the diagnosis and management of sleep disorders: Current trends and future possibilities. J Sleep Res. 2021;30(2):130-140.
- Nguyen T, Liu Y. Genetic approaches to personalized treatment in epilepsy: A review of current strategies. J Epilepsy Res. 2021;45(3):134-145.
- Siddiqui MM, Valsalan P. AI-Based Human Face Recognition System. J Electr Syst. 2024;20.
CrossRef - Taylor M, Richardson D. Advances in wearable technologies for real-time monitoring of Parkinson’s disease symptoms. J Neurol Disord. 2023;27(4):254-265.
- Siddiqui MM, et al. Analysis of EEG data using different techniques of digital signal processing. Biomed Pharmacol J. 2024;17(1).
CrossRef - Wang J, Zhang L. Advances in pharmacogenomics for personalized medicine in epilepsy: From theory to practice. Pharmacogenomics J. 2022;22(5):512-524.
- Xu S, Lee P. AI in neurology: Enhancing the accuracy and efficiency of stroke diagnosis and treatment. J Neurotechnol. 2021;15(3):172-184.
- Feng Y, Li X. Targeted therapies for neurodegenerative diseases: From research to clinical applications. J Neurol Ther. 2023;18(2):94-105.
- Lee R, Kim H. The role of AI in early diagnosis of Alzheimer’s disease: Current trends and future directions. J Alzheimer’s Dis Parkinsonism. 2023;10(4):215-226.
- Srivastava, E. “Carbon Nano Tubes & Its Application in Medical Field & Communication.” International Journal of Advanced Research in Computer and Communication Engineering (IJARCCE), vol. 5, 2016, pp. 170–173.
- Roberts T, Chang M. Recent developments in wearable sensors for managing Parkinson’s disease. Neurotech Adv. 2022;9(1):35-47.
- Nguyen T, Liu Y. Genetic approaches to personalized treatment in epilepsy: A review of current strategies. J Epilepsy Res. 2021;45(3):134-145.
- Chen L, Zhao W. AI applications in early detection of Alzheimer’s disease: A systematic review. J Med Imaging. 2022;30(2):102-114.







