Manuscript accepted on :26-05-2025
Published online on: 09-07-2025
Plagiarism Check: Yes
Reviewed by: Dr. Nitish Chaudhari
Second Review by: Dr. Nagham Aljamali
Final Approval by: Dr. Kamal Upreti
Hriday Kumar Biswas1 , Kanhaiya Kumar Jha1
, Kanhaiya Kumar Jha1 , Vikash Jakhmola2
, Vikash Jakhmola2 , Srishti Morris1*
, Srishti Morris1* , Pallavi Pandey2
, Pallavi Pandey2 , Anshika Rawat1
, Anshika Rawat1 and Akanksha Kumari1
and Akanksha Kumari1
1Department of Pharmaceutics, Uttaranchal Institute of Pharmaceutical Science, Uttaranchal University, Prem Nagar, Dehradun, Uttarakhand, India.
2 Department of Pharmaceutical Chemistry, Uttaranchal Institute of Pharmaceutical Science, Uttaranchal University, Prem Nagar, Dehradun, Uttarakhand, India.
Corresponding Author E-mail: srishtimorris23@gmail.com
Abstract
Artificial Intelligence (AI) is revolutionizing the field of neurology by significantly enhancing disease detection, therapeutic strategies, and patient management. Neurological disorders such as Alzheimer’s disease, Parkinson’s disease, epilepsy, and multiple sclerosis have traditionally been challenging to diagnose and treat due to their complex and heterogeneous nature. Recent advancements in AI, particularly in machine learning and deep learning, enable the analysis of neuroimaging, electroencephalogram (EEG) signals, and genomic data with high precision, facilitating early and more accurate diagnoses. Beyond diagnostics, AI contributes to the development of personalized treatment plans by integrating a patient’s genetic information, medical history, and lifestyle factors. This personalized approach improves therapeutic outcomes and minimizes adverse effects. Wearable AI-powered devices further enhance care by allowing continuous, real-time monitoring of cognitive and motor functions, enabling timely clinical interventions and adjustments in treatment protocols. Moreover, AI is transforming the drug discovery landscape. It assists in identifying novel therapeutic targets, predicting drug responses, repurposing existing drugs, and optimizing clinical trial design, thus reducing the time and cost involved in bringing new treatments to market. Despite its enormous promise, the widespread clinical integration of AI faces challenges such as data privacy concerns, the need for transparent decision-making algorithms, and the establishment of standardized regulatory frameworks. This review explores the evolving applications of AI in neurogenetics and neurology, emphasizing its role in early diagnosis, precision medicine, long-term monitoring, and drug development. Continued interdisciplinary collaboration is essential to harness AI’s full potential in improving neurological healthcare outcomes.
Keywords
Alzheimer's disease; Epilepsy; Neurogenetics; Repurposing; Sclerosis
| Copy the following to cite this article: Biswas H. K, Jha K. K, Jakhmola V, Morris S, Pandey P, Rawat A, Kumari A. Integrating AI with Neurogenetics: Applications in Precision Medicine for Neurological Disorders. Biomed Pharmacol J 2025;18(August Spl Edition). |
| Copy the following to cite this URL: Biswas H. K, Jha K. K, Jakhmola V, Morris S, Pandey P, Rawat A, Kumari A. Integrating AI with Neurogenetics: Applications in Precision Medicine for Neurological Disorders. Biomed Pharmacol J 2025;18(August Spl Edition). Available from: https://bit.ly/477DmNY |
Introduction
In recent years, the integration of artificial intelligence (AI) into neurological sciences has significantly advanced the field of precision medicine for neurological diseases. These disorders—including Alzheimer’s disease, Parkinson’s disease, epilepsy, multiple sclerosis, and various neurogenetic conditions—continue to pose complex challenges in diagnosis, management, and long-term care, as illustrated in Figure 1. Traditional diagnostic approaches, such as neuroimaging, electrophysiological recordings, and clinical assessments, although effective, are often limited by subjectivity, time constraints, and inter-observer variability.¹AI offers a transformative solution to these limitations by leveraging machine learning (ML), deep learning (DL), and other computational techniques to analyze large volumes of neurological data with unprecedented accuracy and speed.² These technologies enable nuanced pattern recognition across multimodal datasets, thereby augmenting clinician capabilities. Real-world applications underscore the growing utility of AI in neurology. For instance, in a study conducted by Titano et al., a deep learning algorithm was employed to detect acute neurologic events in head CT scans with an accuracy rivaling expert radiologists, thus facilitating faster triage in emergency settings.³ Similarly, AI-based electroencephalography (EEG) models have been utilized to predict epileptic seizures with high precision, enabling timely intervention and improved quality of life for epilepsy patients.⁴ In the domain of neurogenetics, AI has been used to analyze whole-genome sequences and identify rare mutations associated with hereditary conditions like Huntington’s disease and familial ALS, offering targeted diagnostic and therapeutic strategies.⁵ AI’s contribution also extends to disease monitoring and therapeutic management. Wearable technologies embedded with AI, such as smartwatches and motion sensors, continuously track motor symptoms in Parkinson’s disease patients. For example, the Parkinson’s Kineti Graph (PKG) has shown clinical utility in assessing bradykinesia and dyskinesia, allowing neurologists to fine-tune dopaminergic therapies in real time.⁶ Additionally, AI-driven mobile applications like “Rejoyn” have demonstrated the ability to deliver personalized cognitive-behavioral therapy for depression through adaptive neurofeedback, showing clinical improvements without adjunct psychotherapy or medications. ⁷Moreover, AI-based predictive modeling is reshaping how neurological diseases are managed longitudinally. Studies employing convolutional neural networks (CNNs) on MRI data have successfully predicted the progression of multiple sclerosis and brain atrophy patterns in early Alzheimer’s disease, paving the way for preemptive care.⁸ This paper aims to explore the transformative role of AI in neurogenetics and its practical impact on driving personalized treatment strategies in neurology. By examining the theoretical frameworks, methodologies, and validated clinical applications of AI, we provide a comprehensive overview of how this technology is revolutionizing diagnostics, therapeutics, and research in neurological sciences. As AI continues to evolve, it holds immense promise in redefining early intervention strategies, improving patient outcomes, and facilitating the development of novel therapeutic pathways for complex neurological disorders.⁹
 |
Figure 1: Shows applications of AI in Neurology 1 |
Novelty and Contribution of the Study
This manuscript provides a comprehensive and up-to-date overview of the latest advancements in the application of artificial intelligence (AI) within neurology. Unlike prior studies that broadly cover AI applications, this work focuses on emerging and innovative areas such as AI-driven real-time adjustment of deep brain stimulation (DBS) to improve symptom management in Parkinson’s disease, and the development of Brain-Computer Interfaces (BCIs) that enable communication for patients with severe neurological impairments. Additionally, the manuscript highlights the integration of genetic, clinical, and imaging data through machine learning models to predict the onset of neurological disorders, allowing for earlier and more proactive intervention. It also explores AI-based speech pattern analysis as a non-invasive method for early diagnosis of Alzheimer’s disease. By synthesizing these cutting-edge developments, the manuscript offers a novel perspective on the shift toward personalized, efficient, and data-driven neurological care, thus providing valuable insights that distinguish this work from existing literature.
Artificial Intelligence in Diagnosing Neurological Disorders
Machine learning (ML), Deep Learning (DL), and advanced computational approaches, Artificial Intelligence (AI) are deeply involved in the diagnosis and management of neurological disease. Here is an overview of artificial intelligence that diagnoses neurological disorders:
Initial diagnosis and identity
a) AI techniques can image the brain similar to MRI, CT scan, and PET scans to detect neurological disorders like multiple sclerosis, Parkinson’s disease, Alzheimer’s disease, and brain tumours. Early diagnosis is superior in detecting the minute details of these techniques, which will prevent the human eye.
b) The computer can be used to interpret electroencephalogram (EEG) readings to determine epilepsy’s wave pattern and enable predicting diseases like epilepsy, towards healing, speedy cure. 9
The machine learning pattern may even diagnose minor symptoms of epilepsy even before the onset of symptoms, sometimes.
Personal medical program
AI can also be employed in tailoring the treatment plan for each patient through individual medical information such as genetics, history, and lifestyle. For instance, AI can assist in monitoring Parkinson’s disease through motor function tracking and recommended modifications in prescription or physical therapy. 10
Steer to the disease future model
Physicians can make more informed decisions regarding treatment pathways and therapy for degenerative neurological conditions like Parkinson’s disease and Alzheimer’s disease to forecast the rate of progression based on patient information. These models forecast using data from several sources of data, like genetic screening, medical history, and imaging. 11
AI employs neurogenetics
AI can search large genomic sets in an attempt to discover neurological disease genetic variants. We may learn more about disease susceptibility due to heredity with Huntington’s Disease, ALS, or inherited Parkinson’s disease. 12
Speech and language disorders
Aphasia (stroke or loss of speech following brain injury) and other speech disorders are some of the diseases for which Artificial Intelligence (AI) solutions are in the process of being created to diagnose and monitor. In an attempt to identify early signs of neurological diseases impacting cognition and speech, such AI tools monitor the language use and patterns of voice. 13
Evaluation of motor and cognitive work
Artificial intelligence (AI)-driven technology can assess motor abilities by analyzing patient movement patterns in neurological disorders such as Parkinson’s disease. For instance, machine learning algorithms can monitor gait patterns, postural stability, and tremors to determine the severity of the condition and provide objective data for tracking disease progression over time. AI also supports cognitive assessments, particularly for conditions like Alzheimer’s disease. Memory impairments, attention deficits, and executive dysfunction can be detected using AI-based cognitive evaluation tools, often even before overt clinical symptoms manifest.¹⁴
Disabled Technologies
AI can offer enabling techniques to assist patients with neurological loss in daily functioning. For instance, AI-controlled devices, brain-computer interfaces (BCIs), or Eye tracking can facilitate patients with limitations of movement. 15
Electronic Health Record (EHR) Integration
The AI is being implemented in the EHR to support clinical decision making, auto-data extraction, and detect discrepancy patterns. It enables quick diagnosis and monitoring, which is especially useful in neurological diseases where early detection and treatment are crucial. 16
Research and development of medicine
By analysing patient data and estimates, who are likely to gain from new treatments, AI can identify eligible participants for clinical trials. AIDS in the formulation of AI medicine that can specifically attack neurological disorders and forecast their efficacy in medical Advancements17.
The neurological disorders, like epilepsy, can be detected in an early stage with the help of AI-aided devices, as shown in Figure 2.
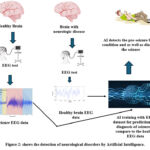 |
Figure 2: Shows the detection of neurological disorders by Artificial Intelligence. |
AI for neurological disease monitoring
Neurological illness is transforming patient monitoring with the provision of precise, individual, and real-time information regarding the progression of AI disease, the effectiveness of treatment, and overall well-being. Specifically, AI is utilized in the following ways to monitor neurological patients:
Real-time monitoring using wear balls and sensors
Wearable technology
Wearable technology powered by AI can monitor people suffering from neurological diseases such as epilepsy, multiple sclerosis, and Parkinson’s disease, and wearers, i.e., wrist and smartwatches. Such devices can monitor numerous parameters, i.e., 18
Movement and GAT
Wearable techniques can track motor functions, including shocks, stiffness, and gait abnormalities in Parkinson’s patients.
AI system confirms this information to offer insight into the disease and help adjust treatment or a drug program. 19
c)Detection of seizure
AI algorithm can analyse sensor data (eg, accelerometer and electrodermal activity sensor) for epilepsy patients to identify the beginning of the seizure. 20
Sleep and heart rhythms
The observation of vital signs such as heart rate and quality of sleep may give insight into patients’ overall wellness, as well as identify issues in patients with neurological disorders. 21,22
Table 1: shows different types of AI devices used in the diagnosis of different Neurological disorders23-26
|
Device Type |
Device Name/Example |
Neurological Data Monitored |
AI Role in Detection |
Application |
|
Wearable EEG Devices |
Muse, Emotiv Epoc+ |
Brain wave activity (EEG) |
AI analyzes EEG patterns to detect anomalies |
Early detection of epilepsy, stress monitoring |
|
AI-powered MRI Scanners |
GE SIGNA, Siemens Magnetom |
Brain structure & abnormalities |
AI detects brain lesions, atrophy, and tumors |
Alzheimer’s, Parkinson’s, and stroke diagnosis |
|
Neuroimaging Analysis Software |
QMENTA, Arterys AI |
MRI & CT scan data |
AI enhances image clarity & detects patterns |
Diagnosis of brain disorders like MS & tumors |
|
Smart Wearables for Neurological Monitoring |
NeurOptimal, Dreem 2 |
Sleep patterns & brain activity |
AI detects sleep disorders & cognitive decline |
Sleep apnea, dementia risk assessment |
|
AI-driven EMG Devices |
MyoPro, NeuroNode |
Muscle & nerve signals (EMG) |
AI detects neuromuscular disorders |
ALS, stroke rehabilitation |
|
Brain-Computer Interfaces (BCIs) |
Neuralink, OpenBCI |
Brain signals for motor control |
AI interprets brain signals for control |
Assistive tech for paralysis & neuro disorders |
|
AI-powered Eye-tracking Devices |
Tobii Pro, EyeLink 1000 |
Eye movement & cognitive response |
AI detects neurological impairments |
Early diagnosis of autism, ADHD, Parkinson’s |
|
Smart Neurological Implants |
Medtronic Deep Brain Stimulation (DBS) |
Brain electrical activity |
AI adjusts stimulation levels in real time |
Parkinson’s, epilepsy treatment |
Analysis of neuroimaging to track the development of the disease
Brain imaging
More and more, they are used to interpret brain scans (CT, MRI, and PET) to monitor the development of diseases such as Alzheimer’s, Parkinson’s, or stroke. Artificial intelligence (AI) approaches are being utilized as well. The physician can determine whether the disease is or isn’t advancing and change treatment in response via an AI program capable of detecting differences in brain anatomy over a timeline, i.e., atrophy or trauma. 27
Disease Indicator Monitoring:
AI can be used to automate the monitoring of biomarker changes from imaging examinations, potentially important in tracking diseases such as multiple sclerosis or brain tumours, and detecting new tumor formation or inflammation. 28
Cognitive Ability and Speech Voice Analysis Monitoring of Cognitive Decline
AI applications can monitor speech patterns and diagnose early indicators of motor speech degeneration or cognitive decline in neurologic diseases of speech, such as stroke or ALS. Monitoring the patient’s speech over a while can be possible with this assistance, and corresponding treatment programs may be modified accordingly. 29
Cognitive Testing Tools
Through examination of answers to questions or tasks, AI-driven programs and tools can conduct cognitive tests. To track disorders like Alzheimer’s, dementia, or other neurodegenerative diseases, such technologies can measure changes in cognitive functions such as memory, attention, and executive function. 30
AI-Powered Predictive Models for Early Warning Systems: Epilepsy Seizure Prediction
From data gathered through the use of wearables, EEG, and other sensors, AI-powered models can predict the chances of a seizure in epilepsy patients. Based on patterns detected within the data, machine learning models can predict when a seizure is likely to happen, so medical staff or caregivers can take preventive measures.
Foreseeing Disease exacerbation
Machine learning models can observe and evaluate patient data (such as laboratory tests, movement, and MRI tests) in conditions such as multiple sclerosis (MS) to predict when an escalation of flares or flare-up of signs and symptoms would occur. It can be permitted to intervene early, and it even has the potential to decrease hospitalization.31
Remote communication and monitoring of patients and physicians
Integration of Telemedicine: AI systems allow patients and healthcare professionals to communicate with one another at their convenience. Wearable devices, for instance, that track motor function and vital signs can directly send data to a physician or specialist for analysis in real-time. Even where the patient cannot physically visit the clinic, this allows them to be monitored more frequently and their treatment plans reviewed more quickly.
Virtual Patient Assistants
Virtual assistants with AI powers can help patients with neurological diseases monitor symptoms, remember medication, and adhere to their treatment regimen. By allowing frequent monitoring and intervention, if needed, these assistants can even act as an interface between the patient and physician. 32
AI-based Patient Monitoring
Healthcare is revolutionized through AI-based patient monitoring, allowing real-time observation, early detection of health change, personalized therapy, and improved outcomes. It makes use of technology such as wearables, sensors, machine learning algorithms, and predictive models for continuous observation of patients and monitoring their health status. A description of the implementation of AI for patient monitoring is provided below:
Continuous Observation by Wearable Technology
Wristwatches and physical activity monitors: Vectors of all sorts, from heart rates, oxygen in blood, sleeping habits, levels of exercise, etc., are tracked by devices like the Fitbit, Apple Watch, or physician-approved medical wearables (e.g., Biofourmis or Fitbit Health models). AI systems continuously monitor such data to look for anomalies and provide prompt alerts when a patient’s health starts degrading. For instance, a smartwatch tracking abnormal heart rhythms (arrhythmias) can alert the patient as well as the doctor to intervene early 33
Body Sensors: Ongoing health information may be accessed through wearable sensors tracking a series of physiological measurements, such as blood pressure, body temperature, respiratory rate, and blood glucose. Remote monitoring is facilitated through AI algorithms converting these signals into actionable information to alert healthcare professionals when a patient’s condition crosses beyond normal thresholds. 34
Remote Patient Monitoring (RPM)
Integration of Telemedicine: Since patients do not need to be visited physically every time, doctors can check patients’ vital signs and symptoms remotely through AI-aided real-time monitoring. This would be especially helpful for patients who have chronic conditions such as diabetes, cardiovascular illness, or neurologic disorders. 35 Example: Telehealth platforms use AI to aggregate data from monitoring devices and wearable sensors to give clinicians information about the patient’s status. If abnormal data is found (for example, an unexplained rise in blood pressure), the system will immediately signal the care provider to take action. 36
Chronic Disease Management: AI is extensively employed to remotely monitor patients with chronic diseases such as diabetes, heart failure, high blood pressure, and COPD. Artificial intelligence (AI) controls disease more effectively by continuously tracking such aspects as lung function or blood sugar. Example for illustration: AI can track the patient’s blood sugar and give real-time insulin suggestions depending on their lifestyle, diet, and sleeping patterns. 37
Early Detection and Predictive Health Monitoring
Predicting Health Events: Artificial intelligence-powered predictive algorithms sift through past and present data to predict clinical events such as seizures, heart attacks, and strokes. By tracking trends in a patient’s vital signs and medical history, predictive algorithms can alert doctors to upcoming dangers before they strike. 38 Example: In epilepsy, AI can anticipate when a seizure will take place by analysing patterns in EEG recordings or other body signals such as heart rate and movement. 39
Early Warning Systems: Through the identification of variations in vital signs, AI software can act as an early warning system for critical illnesses. AI, for instance, can monitor vital signs such as blood pressure, heart rate, and oxygen saturation in intensive care units (ICUs) to predict the risk of complications or deterioration. 40 For instance, via unusual patterns of vital signs, AI technology on intensive care unit monitors can alert caregivers to a patient’s infection or cardiac arrest risk.
Artificial Intelligence in Mental Health
Emotion Recognition and Behavioural Monitoring: AI is employed to monitor patients’ mental health through facial expression analysis, speech patterns, and even social media posts to detect tell-tale signs of depression, anxiety, and other mental disorders. These monitors warn doctors and nurses of any sign of deterioration and give real-time feedback on patients’ emotional condition. 41
Cognitive and Mood Screening: Software with artificial intelligence can regularly screen cognitive functions (such as memory, attention, and mood) and detect early warning signs of mental health crises or dementia. This is especially useful in monitoring the elderly patient or the patient afflicted with diseases like bipolar disorder or Alzheimer’s. 42
Artificial Intelligence for Post-Surgery Monitoring
Artificial intelligence surveillance can be used to monitor a patient’s recovery after surgery. This might be monitoring vital signs such as heart rate and blood pressure, monitoring for infection signs, or ensuring that the patient is following prescribed recovery protocols. For instance, AI programs can monitor improvement, monitor exercises in physical therapy, and alert healthcare professionals when patients achieve recovery milestones. 43
AI in neurosurgery
AI is mainly contributing to neurosurgery, and it can render the accuracy and results of procedures more specific. AI is changing the practice in numerous significant respects through:
Preoperative Planning
AI algorithms can examine patient information, such as MRI, CT scans, and other imaging, to aid surgeons in preparing for intricate neurosurgical operations. Using AI-enhanced imaging technology, surgeons can produce more precise 3D models of the brain, determine critical regions such as tumors, blood vessels, and other anatomy, and outline the safest route of surgery. 44
Intraoperative Assistance
AI is employed in real-time during operations to aid the surgeons. Technologies like robotic surgery systems make use of AI to achieve more accurate movement and aid surgeons to remain on the right course and orientation. For instance, robots can be used, controlled by AI, to assist in minimally invasive surgery, so it becomes achievable to have fewer incisions, less damage to tissues, and quicker healing. AI is transforming intraoperative neurosurgery by enhancing precision and safety. Technologies like augmented reality and real-time 3D mapping assist surgeons in navigating complex brain structures. AI-driven systems, such as Zeta Surgical, provide submillimetre accuracy without rigid head fixation, improving outcomes in procedures like brain biopsies and trauma surgery. 45
Surgical Navigation
Surgical navigation systems based on artificial intelligence are becoming more prevalent for tracking instruments and guiding the surgeon more precisely through the brain. Such systems can provide an overlay of important information over real-time images or the field of surgery, providing more information on instrument location and surrounding anatomy to surgeons. 46
Postoperative Monitoring
AI can also enhance postoperative care through patient monitoring for complications. AI can apply machine learning algorithms that take in patterns of patient data, such as vital signs, lab values, or neurological exams, to identify early warning signs of complications like infection or haemorrhage, which then can be treated earlier. 47
Outcome Prediction and Risk Stratification
AI can be trained to predict the likelihood of a successful operation, complications, and patient recovery to support neurosurgeons with more informed decision-making. AI, by analysing vast amounts of data from prior operations, is capable of detecting risk factors not easily identifiable to human clinicians and providing individualized care plans through predictive models. 48
Surgeon Assistive Technologies
Artificial intelligence technologies are also being used to aid neurosurgeons in certain procedures like surgical planning, decision-making, and follow-up care. For example, AI can process patient data more efficiently than a human being and enable the surgeon to concentrate on clinical decision-making and minimize mental load. 49
Robotic Assistance
Robotic systems that incorporate AI capabilities can be used to improve surgical precision and aid in precise procedures, like tumour excision or deep brain stimulation. The robots can work together with the surgeon in a manner that enables them to perform intricate movements with accuracy. An example of such a robot is the Da Vinci surgery system, which has been utilized in neurosurgery among other surgeries. 50
AI in Neurosurgical Education
Artificial intelligence technologies are being utilized in training new neurosurgeons. With AI-driven virtual or augmented reality platforms, students can carry out mock operations, practice complicated techniques, and get immediate feedback, creating an error-free experience to hone their expertise. 51
AI in Detection and Analysis of Brain Tumours
One of the most compelling applications of AI in neurosurgery is its ability to use to detect and identify brain tumours on scan pictures (i.e., MRIs and CTs). AI software can detect tumours earlier and with greater precision, even if they are small or not detectable by the human eye. AI models can assist in diagnosing the type and grade of the tumours and assist surgeons in deciding on treatments. Artificial Intelligence (AI) is revolutionizing brain tumour detection by enhancing diagnostic accuracy and interpretability. Deep learning models achieve high accuracy in classifying tumours from MRI scans. Integrating Gradient-weighted Class Activation Mapping (Grad-CAM) provides visual explanations, aiding clinicians in understanding AI decisions. This combination ensures both precision and transparency in medical diagnostics. 52
AI in neuroimaging
AI neuroimaging means applying artificial intelligence programs, like machine learning and deep learning, to scan brain images more precisely and effectively. Neuroimaging is fundamental for the diagnosis of neurological illness, planning intervention, and surgical targeting. With AI, we can enhance image interpretation quality, speed up diagnosis, and achieve personalized neurology and neurosurgery. The following are some of the ways AI is revolutionizing neuroimaging:
Computerized Image Analysis
Artificial intelligence, or deep learning, is increasingly used to computerize the analysis of neuroimaging data like MRI (Magnetic Resonance Imaging), CT scans, and PET (Positron Emission Tomography) scans. Human image interpretation may be cumbersome and subject to human error. AI can instantly identify regions of interest (ROIs), pathologies, and quantify certain brain structures with good accuracy. Tumor Detection: AI programs are capable of detecting brain tumors and their nature (e.g., gliomas, meningiomas) with greater accuracy. The system also detects minute variations in tumor size or shape, resulting in earlier detection. Lesion Detection: AI systems become trained in recognizing lesions due to stroke, multiple sclerosis (MS), or other conditions and tend to recognize patterns not readily apparent to human vision. White Matter Lesions: AI models can detect and examine white matter lesions that are linked with aging, neurological disease, and cognitive decline. 53
Segmentation of Brain Structures
Segmentation is a major process in neuroimaging where different areas of the brain (e.g., grey matter, white matter, ventricles) are delineated and annotated for comparison. Manual segmentation is labour-intensive and prone to inconsistency. AI, especially convolutional neural networks (CNNs), has tremendous potential to be used to automatically perform segmentation processes and enhance precision. Grey Matter and White Matter: AI can be utilized to accurately segment these regions and measure brain volume changes, which is beneficial in monitoring the progression of disease in the case of Alzheimer’s disease, multiple sclerosis, and schizophrenia. Subcortical Structures: AI can assist in segmenting subcortical structures (i.e., the hippocampus, thalamus, and basal ganglia), which play an important role in evaluating neurological disorders such as Parkinson’s and Huntington’s. 54
Disease Diagnosis and Classification
AI algorithms are trained on vast collections of neuroimaging scans to identify various brain disorders. The models examine patterns in the images and recognize correlations that may be challenging for human experts to recognize. Neurodegenerative Diseases: AI models can diagnose conditions like Alzheimer’s disease, Parkinson’s disease, and Huntington’s disease by identifying early brain structural and functional changes. Epilepsy: AI can help pinpoint areas in the brain vulnerable to epileptic seizures, enabling more effective surgical planning for individuals with medication-resistant epilepsy. Multiple Sclerosis (MS): AI can sort MRI scans to identify and measure MS lesions, monitor disease progress, and predict treatment outcomes. 55
Prediction of Disease Progression
AI is also increasingly utilized to forecast the course of the disease over time. Machine learning models can model disease progression using longitudinal imaging data, and this is especially useful in chronic and neurodegenerative conditions. Alzheimer’s Disease: Cognitive decline can be predicted using AI to examine MRI or PET scans and correlate these with biomarkers that are characteristic of disease progression. Stroke Recovery: AI can assess brain damage caused by a stroke and predict the recovery process, enabling clinicians to tailor rehabilitation to individual patients. 56
Functional Neuroimaging and Brain Mapping
AI is being utilized for functional neuroimaging (e.g., fMRI (functional MRI), EEG (electroencephalogram), MEG (magnetoencephalography)) to study brain activity. Functional neuroimaging allows one to learn how different brain regions communicate and coordinate with one another during various tasks. Brain Network Analysis: AI can be utilized in the brain network mapping of cognition, sensory perception, and motor control. The maps can be utilized in the comprehension of how neurological disease impacts brain connectivity. Brain-Computer Interfaces (BCIs): AI-based BCIs enable better control of prosthetics or devices by decoding patterns of brain activity. This is especially beneficial in paralysis or other motor disorders. 57
Measurement of Brain Aging and Cognitive Impairment
Machine learning methods are being applied to measure how the brain ages. Machine learning, for instance, can be applied to measure atrophy in individual brain regions (e.g., hippocampus) and relate it to deteriorating cognition, helpful for research on Alzheimer’s and other dementias. 58
Personalized Medicine
AI can handle immense volumes of neuroimaging scans and patient-related data (genomics, medical history, etc.) to aid in customized planning of treatment. This is mostly relevant for cases such as brain tumours or epilepsy, where individualized treatment depending on the patient’s status and response to therapy is needed. 59
Improved Image Quality
AI is also being used to enhance the quality of the imaging itself. For instance, denoising algorithms based on AI can decrease noise in MRI images, producing cleaner images and more visualization of minute details in brain tissue. This is especially useful in high-field MRI, where image quality is affected by noise. Super-resolution Imaging: AI algorithms can create high-resolution images from low-resolution scans, which can be especially helpful in patients who cannot have high-quality imaging because of movement or other issues. 60
AI for Imaging Biomarkers
AI also improves the identification of imaging biomarkers, or quantifiable indicators of disease or health state. In Alzheimer’s disease, for instance, AI can monitor the accumulation of amyloid plaques or tau tangles in the brain, critical biomarkers of the disease. This can translate to earlier diagnosis and improved tracking of disease progression. 61
AI in Neuroimaging Research
Artificial intelligence (AI) has proved particularly beneficial in neuroimaging studies where AI is utilized to analyse enormous data sets coming from diverse groups to gain information about the anatomy and physiology of the brain. AI algorithms can detect patterns through multiple imaging modes (e.g., integration of MRI and gene information) for researching the genes causing neurological diseases or cognitive dysfunctions. 62
Prevention of Neurological Disases
AI is also contributing greatly to the prevention and early diagnosis of neurological ailments. Essentially, AI leverages the power of sophisticated algorithms and machine learning methods to process the intricate datasets, which facilitates detection of early biomarkers and risk factors underlying different neurological disorders such as alzheimer’s disease, Parkinson’s disease, epileptic seizure, dementia, etc.63
Early Diagnosis of Alzheimer’s Disease
By interpreting the neuroimaging data, AI has played a crucial role in the early diagnosis of Alzheimer’s Disease (AD). Deep learning models, using MRI scan patterns of brain atrophy and cerebrospinal fluid levels of tau and β-amyloid proteins, have been highly accurate in diagnosing AD(Alzheimer’s disease).64 The models have achieved diagnostic accuracies of more than 95%, which shows AI’s capability to detect people at risk before clinical symptoms manifest. Mild Cognitive Impairment (MCI) is usually regarded as a prodromal stage to Alzheimer’s Disease (AD). By analysing a range of neuroimaging data, biomarkers, genetic profiles, and cognitive tests, machine learning models have been highly accurate in determining which MCI patients are most likely to develop AD. 65
Parkinson’s Disease Diagnosis
Motor and non-motor symptoms are the most important parameters to diagnose Parkinson’s disease for an AI system. For early detection and to target rehabilitation, the “Shoupa” AI system uses information from intelligent mobile devices to measure PD symptoms. Computer vision methods examine the facial expression, eye movement, and macro expressions(PD indicators) for detecting the disease. AI models are also trained to examine the handwriting pattern for disease prediction. 66
Epileptic Seizure Prediction
Since we are aware that in epileptic seizure, there is an interruption of the brain’s electrical activity, using the electroencephalogram(EEG) data, it can be simply identified. The ‘EpilNet’ AI system uses a one-dimensional convolutional neural network to process electroencephalogram (EEG) data, which predicts epileptic seizure and has attained a testing accuracy of 79.13% for five classes. This advance makes it possible to anticipate by patients and care professionals to anticipate seizure activity, raising treatment methods and data.
Retinal Imaging for the prediction of risk in dementia
The ability of AI to screen retinal images to assess dementia risk has been explored in recent studies. Early diagnosis is offered by an AI model that scans for patterns in retinal vessel patterns to detect changes associated with cognitive decline. This technique underpins strategies aimed at preserving cognitive function and allows for timely interventions. Even with these developments, there are still some difficulties present that need to be solved. Issues such as data quality, ethical considerations, and the interpretability of AI models need to be addressed. Various ongoing research projects aim to overcome these obstacles, to fully harness AI’s potential to transform neurology and improve patient outcomes. 67
AI-Driven Personalized Neurology: From Tailored Treatment to Smartwatch-Based Patient Monitoring
Artificial Intelligence (AI) and Machine Learning (ML) are reshaping neurology by enabling personalized treatment plans and continuous patient monitoring. These technologies analyze complex datasets—such as genetic profiles, neuroimaging, biomarkers, and clinical histories—to identify patterns, predict disease progression, and tailor interventions. From optimizing therapies like Deep Brain Stimulation (DBS) to integrating wearable devices for real-time tracking, AI is transforming neurological care across multiple dimensions.68
Personalized Treatment and AI-Guided Therapies
AI enables precision in diagnosing and treating neurological conditions like epilepsy, Parkinson’s disease, Alzheimer’s, and multiple sclerosis. It customizes treatment plans by selecting optimal medications and dosages, reducing side effects, and improving outcomes. For instance, in DBS for Parkinson’s disease, AI helps determine ideal electrode placements (e.g., subthalamic nucleus) and fine-tunes stimulation parameters based on the patient’s neurological profile.
AI also powers neurorehabilitation systems, adjusting robotic resistance and support in real time to enhance post-stroke motor recovery. In stroke, spinal cord injury, and traumatic brain injury (TBI), AI leverages imaging (e.g., MRI, CT, EEG) and clinical data to support early diagnosis and intervention 69
Long-Term Monitoring and Real-World Applications
AI-integrated wearables—such as smartwatches, fitness bands, and smartphones—facilitate continuous monitoring of neurological conditions. These devices can detect tremors, gait irregularities, and cognitive decline. Apps like Rejoyn offer AI-based cognitive training to reduce depressive symptoms by tapping into neuroplasticity.
Innovative brain-computer interface (BCI) systems, such as the Synchron Switch, allow paralyzed patients to communicate through neural signals. AI models adapt to brain activity, improving over time, and enhancing independence for individuals with ALS, spinal injuries, and stroke-related paralysis 70
Smartwatch Applications in Neurological and Mental Health
Smartwatches now serve as critical tools in health monitoring beyond fitness:
Cardiovascular Monitoring
Devices equipped with PPG sensors detect arrhythmias (like AFib) with high sensitivity and specificity. Some also track SpO₂, aiding in early detection of neurodegenerative diseases linked to cardiovascular dysfunctions.
Sleep Apnea Detection
Apple’s smartwatches, with integrated sensors and ML algorithms, identify respiratory pauses indicative of sleep apnea, validated by partnerships with medical companies like ResMed.
Stress and Mental Health:
By analyzing heart rate variability and respiratory patterns, smartwatches estimate stress levels and mental health states in real time. However, caution is advised due to variability in detection accuracy 71
Integration into Healthcare Systems
While smartwatches offer continuous, real-time data, effective clinical use demands trained professionals, robust data privacy frameworks, and integration into electronic health records. Collaboration between tech developers and healthcare systems is essential to address these challenges.
AI in Neurology -Neurologic Mri Data
Artificial intelligence (AI) and machine learning (ML) have greatly helped in the examination of neurological magnetic resonance imaging (MRI) data and improved diagnosis accuracy and outcomes for patients. These technologies have been used to benefit numerous applications in neurology, ranging from image acquisition and processing to classifying diseases.
AI-Augmented MRI Acquisition and Processing
The MRI acquisition process has been optimized using AI algorithms to enhance the efficiency and image quality. They aid in planning, sequence design, and artifact correction for acquisition, resulting in more accurate imaging results. The technique of conducting MRI scans has been entirely revolutionized by AI-driven MRI acquisition and processing methods that significantly enhance workflow efficiency and image quality. Radiologists can enhance each stage of the MRI procedure, ranging from initial planning through sequence design and artefact correction, using sophisticated AI algorithms. Through consideration of the individual patient anatomy and clinical indications, these algorithms facilitate better planning by ensuring that optimal imaging protocols are chosen to acquire the most relevant information. AI can automatically adjust imaging parameters, like echo and repeat times, in sequence construction, tailoring them to enhance contrast and resolution based on each patient’s specific characteristics. Due to early detection of neurological disorders, early treatment can be started by altering the lifestyle of the patient, as shown in Fig. 3.
Deep Learning Applications in Neuroradiology Deep learning (DL) is a subset of artificial intelligence (AI) and has emerged as a powerful tool in neuroradiology due to its ability to process vast amounts of complex imaging data with high accuracy.
In contrast to conventional machine learning models that involve manual feature extraction, DL algorithms, particularly CNNs, learn and detect patterns in MRI scans automatically and are thus very effective in neuroimaging applications. One of the most important benefits of DL in neuroradiology is its ability to deal with multimodal datasets. This implies that AI models can consolidate data from multiple imaging modalities, including structural MRI (sMRI), functional MRI (fMRI), diffusion-weighted imaging (DWI), and even clinical information, to give a more holistic picture of neurological disease. AI in Disease Classification, Especially in Neurology and Psychiatry 72
One of its most prominent uses is the analysis of MRI data to identify and classify several conditions. One such example is Alzheimer’s disease (AD), where AI algorithms are being applied to detect the minute structural modifications in the brain that might be difficult to see with traditional means. These models facilitate early diagnosis of AD so that interventions can be undertaken in time, and further help in monitoring the progression of the disease over time. Some review paper emphasizes the developments in deep learning, machine learning, and other AI-based methods, which improve the accuracy and efficiency in the diagnosis of Alzheimer’s. These techniques examine brain scan patterns, differentiating between healthy individuals, those with mild cognitive impairment (a precursor to AD), and Alzheimer’s patients with the full-blown disease. By integrating AI into MRI analysis, researchers and clinicians can improve diagnostic precision, reduce human error, and offer better patient outcomes. As AI continues to develop, its role in disease classification is expected to expand, potentially aiding in the detection of other neurological and psychiatric conditions, such as Parkinson’s disease, schizophrenia, and depression. 73
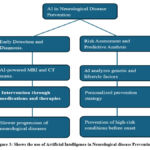 |
Figure 3: Shows the use of Artificial Intelligence in Neurological disease Prevention. |
AI in Drug Discovery and Research
Artificial Intelligence (AI) is revolutionizing the pharmaceutical industry, enabling faster, more effective, and very accurate drug research and discovery. It has historically taken years, sometimes more than a decade, to develop a new drug at an expense of billions of dollars. AI is rewriting this script by automating lengthy processes, sifting through vast data sets at record speed, and even modeling how candidate drugs will react inside the human body before starting clinical trials. One of the greatest contributions of AI is in the identification of lead drug candidates. Rather than depending on conventional trial-and-error, AI algorithms can look through millions of chemical compounds, forecast their characteristics, and identify which ones are most likely to succeed. This not only accelerates the discovery process but also cuts costs drastically. Another way AI is contributing is through drug repurposing—identifying new uses for already approved medications. This strategy gained worldwide attention during the COVID-19 pandemic when scientists utilized AI to scan available drugs for possible antiviral activity, resulting in more rapid treatments.
AI also improves clinical trials by choosing the proper patients using genetic markers, habits, and health history. This precision approach enhances trial success chances and reduces risks. In addition, AI-based models assist in forecasting possible side effects so that scientists can adjust drug formulations before human trials.
Nevertheless, as much as AI provides revolutionary benefits, challenges still exist. Guaranteeing data quality, handling ethical issues, and acquiring regulatory approvals for AI-based drug development are constant challenges. Cooperation among AI researchers, drug companies, and regulatory agencies is necessary to achieve the optimal potential of AI while ensuring patient safety and efficacy of drugs. For interested readers who want to dig deeper into this subject, several research studies offer greater insights into how AI is affecting drug discovery. These resources touch on real-world examples, success stories, and how AI is changing the face of medicine and its future.74
Increasing Target Identification and Validation
Identifying and validating biological targets is one of the most crucial steps in drug development. Before a new drug can be designed, scientists need to find the right “target”—a gene, protein, or molecular pathway that plays a key role in a disease. This is where AI is making a huge impact. Traditionally, researchers had to spend years analyzing biomedical data, conducting experiments, and testing hypotheses to identify potential drug targets. Now, AI can speed up this process by going through enormous amounts of genomic, proteomic, and clinical data to discover latent correlations between genes, proteins, and diseases. By identifying patterns that may not immediately present themselves to human scientists, AI facilitates the identification of new therapeutic targets faster and more accurately. One interesting application of this kind of methodology is the Drugs from Dirt project. AI plays a role here to screen the soil samples for novel antibiotics. Because soil has billions of microbes, many of which are producers of natural compounds with antibiotic potential, researchers rely on AI algorithms to comb through the genetic information of soil microbes for potential candidates of antibiotics. This strategy has the promise of revealing new antibiotics to fight off antibiotic-resistant bacteria, an escalating worldwide health issue. After antibiotics, AI-assisted target discovery is also applied to diseases such as cancer, neurodegenerative disease, and orphan genetic disorders. By integrating AI with large-scale biomedical databases, researchers can identify targets more accurately, minimizing the time and expense required to get new treatments into clinical trials. Nevertheless, although AI has greatly enhanced the process, challenges persist. Extensive laboratory tests and clinical studies are needed to validate AI-identified targets. Furthermore, ensuring that the training data is of good quality and diverse is essential to preventing biases in AI predictions. As AI keeps on advancing, so will its capability to open new targets for drugs, bringing about quicker, more accurate, and more targeted treatment for many diseases.75
Optimizing Lead Identification and Optimization
Artificial intelligence is transforming the process of drug discovery by speeding up the Design-Make-Test-Analyze (DMTA) loop—a foundational system that researchers apply to formulate new medicines. Conventionally, this cycle typically takes several cycles of designing new molecules for drug possibilities, crafting them in a laboratory setting, subjecting them to efficacy trials, and measuring outcomes to enhance the subsequent compound batches. All of this is a lengthy procedure requiring massive resource investments. AI, though, is changing how rapidly and effectively scientists can move through each step. One of the biggest advances of AI is in the ability to predict molecular properties before a substance is even synthesized. Rather than creating and testing thousands of molecules in the physical world, AI models can take enormous amounts of data and predict which forms are likely to produce the desired biological effects. This spares researchers from futile trial-and-error and lets them deal only with the most promising contenders, also facilitating the design of virtual compound libraries—large collections of putative drug molecules produced by computer-based methods. These computer-generated molecules can be tested in silico (computer simulations) to estimate their interaction with biological targets. This step drastically reduces the number of compounds that need to be physically synthesized and tested, speeding up the entire process. In addition, AI helps optimize synthesis routes by identifying the most efficient and cost-effective ways to create drug compounds. Traditional chemical synthesis can be complex, requiring multiple steps with varying success rates. AI-based methods read through enormous datasets of chemical reaction information to provide the optimal synthesis routes, minimizing time, expenditure, and materials lost.
Each step of the DMTA process is streamlined by AI to allow scientists to find and develop lead compounds quicker, eventually fewer iterations before reaching a drug ready for clinical tests. This not only accelerates drug development but also increases the chances of discovering breakthrough treatments faster than ever before. 76
Predicting Drug Efficacy and Safety
Machine learning (ML) is transforming drug discovery by helping researchers predict both the effectiveness and potential risks of new drug candidates before they even reach clinical trials. Conventionally, the process of drug development involves intensive laboratory and animal testing to ascertain if a compound will be effective in humans and if it will cause harmful side effects. Nevertheless, numerous drugs showing significant promise during initial trials fail later on, resulting in time lost, money wasted, and losses amounting to billions of dollars. ML is revolutionizing that by providing a more efficient and data-oriented method.
Through the analysis of enormous amounts of biological and chemical data, ML models can identify subtle patterns that reveal how a drug candidate will act within the human body. The models take into account various factors, including the molecular structure of a compound, how it interacts with proteins, and how it acts on various biological pathways. By comparing new substances to known drugs with established properties, ML can make very accurate predictions of their likely efficacy.
Perhaps the most useful application of ML here is that it can predict possible side effects early in the drug development cycle. Most drugs fail late-stage clinical trials because of unexpected toxicities or adverse effects. ML models that have been trained on past drug information can alert to potential safety issues before a compound reaches human testing. It enables researchers to adjust the chemical composition of a drug at an early stage, avoiding costly and time-intensive clinical trials. Furthermore, ML improves the choice of compounds with better success rates by favoring those that are more likely to clear regulatory approval. Rather than screening thousands of compounds blindly, scientists can target a smaller number of highly promising candidates, dramatically reducing costs and development time.
Although ML-based predictions are not infallible and still need to be confirmed by laboratory and clinical trials, they offer a valuable tool for enhancing efficiency and success rates in drug development. As these models further develop with enhanced access to quality data and improved algorithms, they will increasingly take on a key role in enabling safer and more effective drugs to reach the marketplace sooner than ever before. 77
Personalizing Medicine
AI is transforming medicine by making personalized medicine a possibility. Rather than adhering to a one-size-fits-all treatment paradigm, AI enables physicians to create highly tailored treatment plans using an individual’s specific genetic profile, medical record, lifestyle, and even real-time health information. This transition to precision medicine makes treatments more likely to succeed while minimizing the chance of side effects.
One of the greatest strengths of AI in this field is that it can examine genetic data. Each individual’s DNA has certain variations that determine how they react to medicines. Some metabolize drugs rapidly, and others experience serious side effects because of genetic variation. AI can sort through enormous genetic databases to find patterns and make forecasts about which medication will be most effective for an individual. This is especially useful in areas such as oncology, where genetic analysis through AI identifies cancer patients and recommends the most appropriate targeted therapy likely to be effective based on their tumor’s genetic makeup. Above genetics, AI also considers a patient’s entire medical history, including previous illnesses, medications, and even lifestyle components such as diet and exercise. By combining all this information, AI can suggest treatment regimens that not only work but are also tailored to an individual’s unique needs and risks. For example, in the management of chronic diseases, AI can look at long-term patterns of health to recommend adjustments in drug dosing or lifestyle modifications to avoid complications before they develop. Another promising use is AI-enabled wearable devices that monitor a patient’s health continuously in real time. These devices monitor vital signs, sense early warning signs, and give doctors real-time patient information so they can intervene in an instant if necessary. Such personalized care prevents hospitalization, enhances quality of life, and provides patients with the right care at the right time. Although there are these advances, challenges do exist. Ensuring privacy of data, incorporating AI into current healthcare systems, and reducing biases in AI models are all significant components in maximizing the potential of personalized medicine. Yet with technology’s constant progression and AI getting smarter, the healthcare future is going to be more and more customized to every patient, ensuring that treatments are more effective and, generally, better outcomes are achieved. 78,79
Enabling Drug Repurposing
AI is revolutionizing how we come up with new treatments by finding novel therapeutic applications for already-approved medicines—a process called drug repurposing. Conventionally, the process of creating a new drug from the ground up takes years in the making and billions of dollars. But AI makes it possible to significantly accelerate the process by scouring enormous amounts of medical information to discover previously unknown relationships between drugs and diseases, providing new hope to patients who require faster and more efficient treatments.80
One of AI’s greatest strengths in drug repurposing is its ability to analyze different types of biomedical data simultaneously. By examining clinical trial records, patient medical histories, genetic databases, and biochemical interactions, AI can detect patterns that humans might overlook. For example, a drug originally developed for treating high blood pressure may unexpectedly show promise in reducing symptoms of neurodegenerative diseases like Parkinson’s. Without AI, such associations might take years, or never be found at all.
One notable instance of AI-driven repurposing of drugs was in the context of the COVID-19 pandemic. Scientists employed AI to browse through lists of FDA-approved compounds to find drugs that had the potential to combat the virus. This method assisted in speeding up clinical trials of drugs already available for antiviral and anti-inflammatory purposes, quickening the roll-out of drugs for treatment amidst a global crisis.
Aside from infectious diseases, AI is also taking a pivotal role in drug repurposing for chronic diseases such as cancer, Alzheimer’s, and autoimmune diseases. Most drugs that are already available have established safety profiles, so when AI finds a new indication for them, they can usually bypass the initial phases of drug development. Not only does this save time and money, but it also raises the likelihood of success in subsequent-stage clinical trials.
But although AI represents a potent new weapon for drug repurposing, there are challenges. Precise prediction of drug-disease interactions is achieved only with high-quality data, and regulatory clearance for repurposed drugs takes time. Furthermore, pharmaceutical companies might be slow to invest in repurposing established drugs because there are few financial incentives.
Despite those challenges, AI-based drug repurposing is a significant advancement in contemporary medicine. Through identifying novel uses for approved drugs, AI is enabling life-saving medicines to reach patients sooner, more effectively, and at lower costs than ever. As AI technology advances, its contribution to expanding treatment opportunities will only increase, providing new hope in confronting some of the world’s most debilitating diseases 81.
Challenges and Ethical Issues
AI is transforming drug discovery, but its adoption in the pharma industry is not without challenges. While AI can accelerate drug development, enhance precision, and lower costs, its success is contingent upon resolving major challenges—data quality, model interpretability, and ethical issues—before it can gain traction in real-world clinical applications.
Ensuring high-quality data is one of the greatest challenges. AI models require colossal sets of data to accurately predict, but not all biomedical data is consistent, complete, and standardized. Heterogeneous data from various sources—e.g., clinical trials, electronic health records, and genomic studies—will result in biased or inaccurate AI predictions. If the data that an AI system receives is faulty, the output will also be faulty, which can result in improper drug suggestions or missed treatment chances. To counter this, improved data gathering, harmonization, and thorough validation processes are needed.
The interpretability of AI models is another big problem. Most AI-based drug discovery techniques, particularly deep learning algorithms, are “black boxes” since they give answers without properly detailing how they made their prediction. Interpretability is very important in drug discovery since researchers, physicians, and regulatory officials must know why a drug candidate is expected to be effective or safe. If recommendations generated by AI cannot be explained or justified, they would not be trusted by regulatory agencies or pharmaceutical companies. There are ongoing efforts to create explainable AI models that provide transparent justification for their predictions, so they can be used more effectively in medical decision-making.
Ethical issues, most critically around data privacy, also present a major hurdle. Drug discovery based on AI relies on large-scale availability of patient data, such as genetic data, medical history, and treatment outcomes. Although this information is precious when constructing personalized medicine, it challenges concerns regarding consent, security, and misuse. The patients must have faith in having their delicate medical data preserved and stringent control being exercised to hinder unauthorized leaks of the information and wrongful uses of the AI. An accurate balance needs to be made between data usability and privacy, such that AI both delivers and exercises the rightness necessary in medical construction.
To overcome such obstacles, sustained interaction between AI researchers, drug development scientists, clinicians, and regulatory agencies is imperative. Researchers can improve AI algorithms, clinicians can offer clinical knowledge to make sure AI follows real-world patient needs, and regulatory agencies can implement guidelines for the safe and ethical use of AI. Together, these stakeholders can overcome the shortcomings of AI in drug discovery while leveraging its potential to create life-saving therapies in record time and with optimal efficiency.
As AI evolves further, its contribution to the pharmaceutical industry will grow in significance—but only if it can surmount these challenges through equitable, open, and collective innovation.
The integration of AI in drug research and discovery is full of promise to revolutionize the world of pharmaceuticals, as it provides better treatments and enhances patient outcomes.
Challenges and Future Directions
While AI has made spectacular strides in disease classification, the integration of AI in actual clinical practice is full of challenges. A key challenge lies in dataset variability—MRI scans can vary widely based on equipment, imaging protocols, and even patient demographics. AI models optimized on one set of data do not necessarily translate as well on another, with resulting variability in diagnosis. Another problem is that there is too much validation on a large scale. Although several AI models have highly encouraging results within research environments, they must be validated on widely varying, actual patient populations so that they reliably operate in any given healthcare environment. Without strict validation, there is potential for misdiagnosis or bias, which may ultimately impact patient care. Interpretability is a second important issue. Most AI models, especially deep learning-based models, are “black boxes,” in that they offer a diagnosis or prediction without explaining clearly how they came to that conclusion. This transparency deficiency causes it to be hard for physicians to have total confidence or respond to AI-provided insights because medical decisions have to be quite certain and responsible. To transcend these challenges, continuous research and increased cooperation among AI researchers and clinicians are paramount. AI engineers can make the models more transparent and responsive, while physicians can offer insights that will help make the technology accommodate actual clinical necessities. Together, we can bring us closer to the complete integration of AI into neurological MRI analysis, ensuring early and precise disease detection for more patients across the globe.
Discussion
The integration of artificial intelligence (AI) into neurological healthcare systems represents a transformative shift toward personalized, efficient, and minimally invasive approaches. Our findings highlight the growing role of AI in various domains—ranging from diagnosis and monitoring to surgical intervention and treatment optimization.
AI in Clinical Decision Support and Early Diagnosis
AI-powered algorithms are increasingly embedded in electronic health records (EHRs) to enhance clinical decision-making. Through auto-data extraction and anomaly detection, these systems can identify critical patterns that may otherwise be missed by clinicians. This is particularly vital in neurological disorders, where early detection significantly improves patient outcomes.
Comparison with Traditional Approaches
Unlike traditional Deep Brain Stimulation (DBS), which delivers continuous electrical pulses, AI-based DBS monitors real-time brain activity and dynamically adjusts stimulation accordingly. This adaptive capability not only reduces symptoms more effectively but also minimizes side effects such as speech and gait disturbances associated with conventional DBS. Additionally, AI algorithms analyze medical imaging and patient data to detect neurological conditions like Alzheimer’s, Parkinson’s, and multiple sclerosis at earlier stages. This enables timely interventions that can slow disease progression and improve patient outcomes, representing a significant advancement over traditional diagnostic and treatment methods.
Wearables and Remote Monitoring Technologies
Our study also underscores the role of AI-enabled wearable devices in continuous monitoring of neurological conditions such as epilepsy, multiple sclerosis, and Parkinson’s disease. Data from wearables, EEG, and biosensors can be processed by machine learning models to predict seizure risk, monitor tremor progression, or track treatment efficacy.
AI in Telehealth and Real-Time Alerts
AI’s integration into telehealth platforms enhances patient surveillance. The system’s ability to flag abnormal patterns—such as a sudden rise in intracranial pressure or fluctuations in blood pressure—supports proactive care. This feature is particularly useful for managing chronic neurological conditions remotely and reducing the need for emergency interventions.
AI in Neurosurgery and Tumor Diagnostics
Our findings further indicate that AI applications in neurosurgery are advancing precision medicine. AI tools can assist in detecting brain tumors at earlier stages, classifying tumor types, and suggesting optimal surgical strategies. Additionally, AI aids in intraoperative navigation, reducing human error and improving patient safety.
Implications for Personalized Treatment
AI contributes to the personalization of treatment regimens by analyzing patient-specific variables to recommend suitable drugs, dosages, and interventions. Such customization reduces adverse effects and enhances therapeutic efficacy across a range of neurological conditions.
Limitations and Future Directions
While the potential is vast, the implementation of AI in neurology also presents challenges, including data privacy concerns, model interpretability, and the need for large, diverse datasets. Future research should focus on developing explainable AI models, ensuring equitable access to AI tools, and conducting clinical validation studies to translate algorithmic success into real-world benefits.
Conclusion
Neurological diseases remain a significant global health issue, impacting millions of lives and necessitating a multidisciplinary, collaborative strategy for diagnosis, treatment, and research. This review has emphasized the intricacies of these conditions, ranging from their underlying mechanisms to the most current innovations in diagnostic tools, treatment strategies, and new research directions. With advancements in neuroimaging technologies, biomarker identifications, and personalized medicine, healthcare workers are now able to diagnose and treat these disorders more effectively and provide patients with better and more customized treatments. AI algorithms analyse neuroimaging data to detect early signs of neurological disorders like Alzheimer’s and Parkinson’s diseases, helping in timely interventions. These predictive models assess genetic and lifestyle factors to estimate the risk of developing disorders. AI helps in personalized treatment strategies that are more effective with fewer side effects, and continuous monitoring can be possible for better management of neurological disorders. Yet, while such promising breakthroughs exist, they are also subject to challenge. The prohibitive expense of therapy, shortages in specialized treatment availability, and deficiencies in the existing knowledge base for neurodegenerative disease persist as substantial roadblocks. Overcoming them, however, will require that researchers continue to innovate through avenues like gene therapy, regenerative medicine, and AI-based diagnostics. In addition, raising public knowledge, enhancing programs for early detection, and bringing more access to advanced healthcare technology will be crucial to achieving genuine progress. In short, although we have achieved incredible progress in neurology, there is much more to be done. Progress in our knowledge of neurological disorders depends on continued cooperation among scientists, clinicians, and policymakers. By promoting innovation and providing fair access to new therapies, we are closer to a future where neurological disorders can be managed more effectively and eventually prevented, enhancing the lives of millions of people worldwide.
Acknowledgement
Authors conveyed thanks to Mr. Jitender Joshi, Chancellor, and Prof. (Dr.) Dharam Buddhi, Vice Chancellor of Uttaranchal University-Dehradun, for encouraging the work.
Funding Sources
The authors received no financial support for the research, authorship, and/or publication of this article.
Conflict of Interest
The author(s) do not have any conflict of interest.
Data Availability Statement
This statement does not apply to this article.
Ethics statement
This research did not involve human participants, animal subjects, or any material that requires ethical approval.
Informed consent statement
This study did not involve human participants, and therefore, informed consent was not required.
Clinical Trial Registration
This research does not involve any clinical trials
Permission to reproduce material from other sources
Not Applicable
Author’s Contribution:
- Hriday Kumar Biswas: Data collection and writing
- Kanhaiya Kumar Jha: Writing, Methodology
- Srishti Morris:. Review and supervision
- Pallavi Pandey: Editing, Review.
- Vikash Jakhmola: Supervision.
- Anshika Rawat: writing
- Akanksha Kumari: writing
References
- Kalani M, Anjankar A. Revolutionizing neurology: the role of artificial intelligence in advancing diagnosis and treatment. Cureus. 2024;16(6). doi:10.7759/cureus.61706
CrossRef - Vilhekar RS, Rawekar A. Artificial intelligence in genetics. Cureus. 2024;16(1). doi:10.7759/cureus.52035
CrossRef - Mishra R, Li B. The application of artificial intelligence in the genetic study of Alzheimer’s disease. Aging Dis. 2020;11(6):1567. https://doi.org/10.14336/AD.2020.0312
CrossRef - Singh A, Velagala VR, Kumar T, Dutta RR, Sontakke T. The application of deep learning to electroencephalograms, magnetic resonance imaging, and implants for the detection of epileptic seizures: a narrative review. Cureus. 2023;15(7). doi:10.7759/cureus.42460
CrossRef - Shajari S, Kuruvinashetti K, Komeili A, Sundararaj U. The emergence of AI-based wearable sensors for digital health technology: a review. Sensors. 2023;23(23):9498. https://doi.org/10.3390/s23239498
CrossRef - Dixon D, Sattar H, Moros N, et al. Unveiling the influence of AI predictive analytics on patient outcomes: a comprehensive narrative review. Cureus. 2024;16(5). doi:10.7759/cureus.59954
CrossRef - Johnson KB, Wei WQ, Weeraratne D, et al. Precision medicine, AI, and the future of personalized health care. Clin Transl Sci. 2021;14(1):86-93. https://doi.org/10.1111/cts.12884
CrossRef - Gutman B, Shmilovitch AH, Aran D, Shelly S. Twenty-five years of AI in neurology: the journey of predictive medicine and biological breakthroughs. JMIR Neurotechnol. 2024;3(1):e59556. https://doi.org/10.2196/59556
CrossRef - Reddy S, Giri D, Patel R. Artificial intelligence diagnosis of Parkinson’s disease from MRI scans. Cureus. 2024;16(4). doi:10.7759/cureus.58841
CrossRef - Maleki Varnosfaderani S, Forouzanfar M. The role of AI in hospitals and clinics: transforming healthcare in the 21st century. Bioengineering. 2024;11(4):337. https://doi.org/10.3390/bioengineering11040337
CrossRef - Palanisamy CP, Pei J, Alugoju P, et al. New strategies of neurodegenerative disease treatment with extracellular vesicles (EVs) derived from mesenchymal stem cells (MSCs). Theranostics. 2023;13(12):4138. https://doi.org/10.7150/thno.83066
CrossRef - Roberts JS, Uhlmann WR. Genetic susceptibility testing for neurodegenerative diseases: ethical and practice issues. Prog Neurobiol. 2013;110:89-101. https://doi.org/10.1016/j.pneurobio.2013.02.005
CrossRef - Zhong X. AI-assisted assessment and treatment of aphasia: a review. Front Public Health. 2024;12:1401240. https://doi.org/10.3389/fpubh.2024.1401240
CrossRef - Rana A, Dumka A, Singh R, Panda MK, Priyadarshi N, Twala B. Imperative role of machine learning algorithm for detection of Parkinson’s disease: review, challenges and recommendations. Diagnostics. 2022;12(8):2003. https://doi.org/10.3390/diagnostics12082003
CrossRef - Zhang X, Ma Z, Zheng H, et al. The combination of brain-computer interfaces and artificial intelligence: applications and challenges. Ann Transl Med. 2020;8(11):712. https://doi.org/10.21037/atm.2019.11.109
CrossRef - Al Kuwaiti A, Nazer K, Al-Reedy A, et al. A review of the role of artificial intelligence in healthcare. J Pers Med. 2023;13(6):951. https://doi.org/10.3390/jpm13060951
CrossRef - Vora LK, Gholap AD, Jetha K, Thakur RR, Solanki HK, Chavda VP. Artificial intelligence in pharmaceutical technology and drug delivery design. Pharmaceutics. 2023;15(7):1916. https://doi.org/10.3390/ pharmaceutics15071916
CrossRef - Minen MT, Stieglitz EJ. Wearables for neurologic conditions: considerations for our patients and research limitations. Neurol Clin Pract. 2021;11(4):e537-e543. https://doi.org/10.1212/CPJ.0000000000000971
CrossRef - Wu P, Cao B, Liang Z, Wu M. The advantages of artificial intelligence-based gait assessment in detecting, predicting, and managing Parkinson’s disease. Front Aging Neurosci. 2023;15:1191378. https://doi.org/10.3389/fnagi.2023.1191378
CrossRef - Yu S, El Atrache R, Tang J, et al. Artificial intelligence‐enhanced epileptic seizure detection by wearables. Epilepsia. 2023;64(12):3213-3226. doi:10.1111/epi.17774
CrossRef - Desai D, Momin A, Hirpara P, et al. Exploring the role of circadian rhythms in sleep and recovery: a review article. Cureus. 2024 Jun 3;16(6). https://doi.org/10.7759/cureus.61568
CrossRef - Jadhwani PL, Harjpal P. A review of artificial intelligence-based gait evaluation and rehabilitation in Parkinson’s disease. Cureus. 2023 Oct 16;15(10). https://doi.org/10.7759/cureus.47118
CrossRef - Kumar S. Early disease detection using AI: a deep learning approach to predicting cancer and neurological disorders. Int J Sci Res Manag. 2025;13(4):2136-2155.
CrossRef - Segato A, Marzullo A, Calimeri F, De Momi E. Artificial intelligence for brain diseases: a systematic review. APL Bioeng. 2020;4(4):–.
CrossRef - Vashistha R, Yadav D, Chhabra D, Shukla P. Artificial intelligence integration for neurodegenerative disorders. In: Leveraging Biomedical and Healthcare Data. 2019:77-89.
CrossRef - Haghayegh S, Herzog R, Bennett DA, Redline S, Yaffe K, Stone KL, Ibáñez A, Hu K. Predicting future risk of developing cognitive impairment using ambulatory sleep EEG: integrating univariate analysis and multivariate information theory approach. J Alzheimers Dis. 2025;–:13872877251319742.
CrossRef - Burgos N. Neuroimaging in machine learning for brain disorders. Machine Learning for Brain Disorders. 2023 Jul 23:253-84. http://dx.crossref.org/10.1007/978-1-0716-3195-9_8
CrossRef - Bi WL, Hosny A, Schabath MB, et al. Artificial intelligence in cancer imaging: clinical challenges and applications. CA: A Cancer Journal for Clinicians. 2019 Mar;69(2):127-57. https://doi.org/10.3322/caac.21552
CrossRef - Li R, Wang X, Lawler K, et al. Applications of artificial intelligence to aid early detection of dementia: a scoping review on current capabilities and future directions. Journal of Biomedical Informatics. 2022 Mar 1;127:104030. https://doi.org/10.1016/j.jbi.2022.104030
CrossRef - Javed AR, Saadia A, Mughal H, et al. Artificial intelligence for cognitive health assessment: state-of-the-art, open challenges and future directions. Cognitive Computation. 2023 Nov;15(6):1767-812. https://doi.org/10.1007/s12559-023-10153-4
CrossRef - Moazami F, Lefevre-Utile A, Papaloukas C, Soumelis V. Machine learning approaches in study of multiple sclerosis disease through magnetic resonance images. Frontiers in Immunology. 2021 Aug 11;12:700582. https://doi.org/10.3389/fimmu.2021.700582
CrossRef - Tsvetanov F. Integrating AI technologies into remote monitoring patient systems. Engineering Proceedings. 2024 Aug 20;70(1):54. https://doi.org/10.3390/engproc2024070054
CrossRef - Shei RJ, Holder IG, Oumsang AS, et al. Wearable activity trackers–advanced technology or advanced marketing?. European Journal of Applied Physiology. 2022 Sep;122(9):1975-90. https://doi.org/10.1007/s00421-022-04951-1
CrossRef - Ming DK, Sangkaew S, Chanh HQ, et al. Continuous physiological monitoring using wearable technology to inform individual management of infectious diseases, public health and outbreak responses. International Journal of Infectious Diseases. 2020 Jul 1;96:648-54. https://doi.org/10.1016/j.ijid.2020.05.086
CrossRef - Haleem A, Javaid M, Singh RP, Suman R. Telemedicine for healthcare: capabilities, features, barriers, and applications. Sensors International. 2021 Jan 1;2:100117. https://doi.org/10.1016/j.sintl.2021.100117
CrossRef - Perez K, Wisniewski D, Ari A, et al. Investigation into application of AI and telemedicine in rural communities: a systematic literature review. Healthcare. 2025 Feb 4;13(3):324. https://doi.org/10.3390/ healthcare 13030324
CrossRef - Dong C, Ji Y, Fu Z, et al. Precision management in chronic disease: an AI empowered perspective on medicine-engineering crossover. iScience. 2025 Mar 21;28(3). https://doi.org/10.1016/j.isci.2025.112044
CrossRef - edanki S, Dommati N, Bodapati HH, et al. Artificial intelligence powered glucose monitoring and controlling system: pumping module. World Journal of Experimental Medicine. 2024 Mar 20;14(1):87916. https://doi.org/ 10.5493/wjem.v14.i1.87916
CrossRef - Phillips SP, Spithoff S, Simpson A. Artificial intelligence and predictive algorithms in medicine: promise and problems. Canadian Family Physician. 2022 Aug 1;68(8):570-2. https://doi.org/10.46747/cfp.6808570
CrossRef - Mourid MR, Irfan H, Oduoye MO. Artificial intelligence in pediatric epilepsy detection: balancing effectiveness with ethical considerations for welfare. Health Science Reports. 2025 Jan;8(1):e70372. https://doi.org/10.1002/hsr2.70372
CrossRef - Muralitharan S, Nelson W, Di S, et al. Machine learning–based early warning systems for clinical deterioration: systematic scoping review. Journal of Medical Internet Research. 2021 Feb 4;23(2):e25187. https://doi.org/10.2196/25187
CrossRef - Zafar F, Alam LF, Vivas RR, et al. The role of artificial intelligence in identifying depression and anxiety: a comprehensive literature review. Cureus. 2024 Mar 19;16(3). https://doi.org/10.7759/cureus.56472
CrossRef - Lyall DM, Kormilitzin A, Lancaster C, et al. Artificial intelligence for dementia—applied models and digital health. Alzheimer’s & Dementia. 2023 Dec;19(12):5872-84. https://doi.org/10.1002/alz.13391
CrossRef - Yelne S, Chaudhary M, Dod K, et al. Harnessing the power of AI: a comprehensive review of its impact and challenges in nursing science and healthcare. Cureus. 2023 Nov 22;15(11). https://doi.org/ 10.7759/ cureus.49252
CrossRef - Pinto-Coelho L. How artificial intelligence is shaping medical imaging technology: a survey of innovations and applications. Bioengineering. 2023;10(12):1435. https://doi.org/10.3390/bioengineering10121435
CrossRef - Knudsen JE, Ghaffar U, Ma R, Hung AJ. Clinical applications of artificial intelligence in robotic surgery. J Robot Surg. 2024;18(1):102. https://doi.org/10.1007/s11701-024-01867-0
CrossRef - Knudsen JE, Ghaffar U, Ma R, Hung AJ. Clinical applications of artificial intelligence in robotic surgery. J Robot Surg. 2024;18(1):102. https://doi.org/10.7759/cureus.51631
CrossRef - Khalifa M, Albadawy M. Artificial intelligence for clinical prediction: exploring key domains and essential functions. Comput Methods Programs Biomed Update. 2024;100148. https://doi.org/10.1016/j.cmpbup. 2024.100148
CrossRef - Hassan AM, Rajesh A, Asaad M, Nelson JA, Coert JH, Mehrara BJ, Butler CE. Artificial intelligence and machine learning in prediction of surgical complications: current state, applications, and implications. Am Surg. 2023;89(1):25-30. https://doi.org/10.1177/00031348221101488
CrossRef - Tangsrivimol JA, Schonfeld E, Zhang M, Veeravagu A, Smith TR, Härtl R, et al. Artificial intelligence in neurosurgery: a state-of-the-art review from past to future. Diagnostics. 2023;13(14):2429. https://doi.org/10.3390/diagnostics13142429
CrossRef - Biswas P, Sikander S, Kulkarni P. Recent advances in robot-assisted surgical systems. Biomed Eng Adv. 2023;6:100109. https://doi.org/10.1016/j.bea.2023.100109
CrossRef - Riddle EW, Kewalramani D, Narayan M, Jones DB. Surgical simulation: virtual reality to artificial intelligence. Curr Probl Surg. 2024;61(11):101625. https://doi.org/10.1016/j.cpsurg.2024.101625
CrossRef - Williams S, Layard Horsfall H, Funnell JP, Hanrahan JG, Khan DZ, Muirhead W, et al. Artificial intelligence in brain tumour surgery—an emerging paradigm. Cancers. 2021;13(19):5010. https://doi.org/10.3390/ cancers13195010
CrossRef - Arabi H, AkhavanAllaf A, Sanaat A, Shiri I, Zaidi H. The promise of artificial intelligence and deep learning in PET and SPECT imaging. Phys Med. 2021;83:122-137. https://doi.org/10.1016/j.ejmp.2021.03.008
CrossRef - Andrews M, Di Ieva A. Artificial intelligence for brain neuroanatomical segmentation in magnetic resonance imaging: A literature review. J Clin Neurosci. 2025;134:111073. https://doi.org/10.1016/j.jocn.2025.111073
CrossRef - Qadri YA, Ahmad K, Kim SW. Artificial general intelligence for the detection of neurodegenerative disorders. Sensors. 2024;24(20):6658. https://doi.org/10.3390/s24206658
CrossRef - Kale MB, Wankhede NL, Pawar RS, Ballal S, Kumawat R, Goswami M, et al. AI-driven innovations in Alzheimer’s disease: Integrating early diagnosis, personalized treatment, and prognostic modelling. Ageing Res Rev. 2024;102497. https://doi.org/10.1016/j.arr.2024.102497
CrossRef - Gui XU, Chuansheng CH, Zhong-Lin LU, Qi DO. Brain imaging techniques and their applications in decision-making research. Acta Psychol Sin. 2010;42(1):120. https://doi.org/10.3724/SP.J.1041.2010.00120
CrossRef - Singh NM, Harrod JB, Subramanian S, Robinson M, Chang K, Cetin-Karayumak S, et al. How machine learning is powering neuroimaging to improve brain health. Neuroinformatics. 2022;20(4):943-964. https://doi.org/10.1007/s12021-022-09572-9
CrossRef - Cè M, Irmici G, Foschini C, Danesini GM, Falsitta LV, Serio ML, et al. Artificial intelligence in brain tumor imaging: a step toward personalized medicine. Curr Oncol. 2023;30(3):2673-2701. https://doi.org/10.3390/curroncol30030203
CrossRef - Chen Z, Pawar K, Ekanayake M, Pain C, Zhong S, Egan GF. Deep learning for image enhancement and correction in magnetic resonance imaging—state-of-the-art and challenges. J Digit Imaging. 2023;36(1):204-230. https://doi.org/10.1007/s10278-022-00721-9
CrossRef - Winchester LM, Harshfield EL, Shi L, Badhwar A, Khleifat AA, Clarke N, et al. Artificial intelligence for biomarker discovery in Alzheimer’s disease and dementia. Alzheimers Dement. 2023;19(12):5860-5871. https://doi.org/10.1002/alz.13390
CrossRef - Monsour R, Dutta M, Mohamed AZ, Borkowski A, Viswanadhan NA. Neuroimaging in the era of artificial intelligence: current applications. Fed Pract. 2022;39(Suppl 1):S14. https://doi.org/10.12788/fp.0231
CrossRef - Francisco A, Pascoal C, Lamborne P, Morais H, Gonçalves M, Pascoal Sr C, et al. Wearables and Atrial Fibrillation: Advances in Detection, Clinical Impact, Ethical Concerns, and Future Perspectives. Cureus. 2025;17(1). https://doi.org/10.7759/cureus.77404
CrossRef - Li K, Cardoso C, Moctezuma-Ramirez A, Elgalad A, Perin E. Heart rate variability measurement through a smart wearable device: Another breakthrough for personal health monitoring?. Int J Environ Res Public Health. 2023;20(24):7146. https://doi.org/10.3390/ijerph20247146
CrossRef - Masoumian Hosseini M, Masoumian Hosseini ST, Qayumi K, Hosseinzadeh S, Sajadi Tabar SS. Smartwatches in healthcare medicine: assistance and monitoring; a scoping review. BMC Med Inform Decis Mak. 2023;23(1):248. https://doi.org/10.1186/s12911-023-02350-w
CrossRef - Pandey P, Gauniya P. Image-Guided Surgery Through ML and IoT. InEvolution of Machine Learning and Internet of Things Applications in Biomedical Engineering 2024 Oct 30 (pp. 251-280). CRC Press.
CrossRef - Taiyeb Khosroshahi M, Morsali S, Gharakhanlou S, Motamedi A, Hassanbaghlou S, Vahedi H, et al. Explainable Artificial Intelligence in Neuroimaging of Alzheimer’s Disease. Diagnostics. 2025;15(5):612. https://doi.org/10.3390/diagnostics15050612
CrossRef - Rusz J, Krack P, Tripoliti E. From prodromal stages to clinical trials: The promise of digital speech biomarkers in Parkinson’s disease. Neurosci Biobehav Rev. 2024;105922. https://doi.org/10.1016/ j.neubiorev.2024.105922
CrossRef - Hao J, Kwapong WR, Shen T, Fu H, Xu Y, Lu Q, et al. Early detection of dementia through retinal imaging and trustworthy AI. npj Digit Med. 2024;7(1):294. https://doi.org/10.1038/s41746-024-01292-5
CrossRef - Khalifa M, Albadawy M. AI in diagnostic imaging: Revolutionising accuracy and efficiency. Comput Methods Programs Biomed Update. 2024;100146. https://doi.org/10.1016/j.cmpbup.2024.100146
CrossRef - Watts J, Khojandi A, Shylo O, Ramdhani RA. Machine learning’s application in deep brain stimulation for Parkinson’s disease: A review. Brain Sci. 2020;10(11):809. https://doi.org/10.3390/brainsci10110809
CrossRef - Chakrabarti S, Biswas N, Jones LD, Kesari S, Ashili S. Smart consumer wearables as digital diagnostic tools: a review. Diagnostics. 2022;12(9):2110. https://doi.org/10.3390/diagnostics12092110
CrossRef - Abdulkader SN, Atia A, Mostafa MS. Brain computer interfacing: Applications and challenges. Egypt Inform J. 2015;16(2):213-230. https://doi.org/10.1016/j.eij.2015.06.002
CrossRef - AbuAlrob MA, Mesraoua B. Harnessing artificial intelligence for the diagnosis and treatment of neurological emergencies: A comprehensive review of recent advances and future directions. Front Neurol. 2024;15:1485799. https://doi.org/10.3389/fneur.2024.1485799
CrossRef - Shimron E, Perlman O. AI in MRI: computational frameworks for a faster, optimized, and automated imaging workflow. Bioengineering. 2023;10(4):492. https://doi.org/10.3390/bioengineering10040492
CrossRef - Mak KK, Wong YH, Pichika MR. Artificial intelligence in drug discovery and development. Drug Discov Eval Saf Pharmakinet Assays. 2024:1461-1498. https://doi.org/10.1007/978-3-031-35529-5_92
CrossRef - Struble TJ, Alvarez JC, Brown SP, Chytil M, Cisar J, DesJarlais RL, et al. Current and future roles of artificial intelligence in medicinal chemistry synthesis. J Med Chem. 2020;63(16):8667-8682. https://doi.org/10.1021/ acs.jmedchem.9b02120
CrossRef - Rehman AU, Li M, Wu B, Ali Y, Rasheed S, Shaheen S, et al. Role of artificial intelligence in revolutionizing drug discovery. Fundam Res. 2024. https://doi.org/10.1016/j.fmre.2024.04.021
CrossRef - Serrano DR, Luciano FC, Anaya BJ, Ongoren B, Kara A, Molina G, et al. Artificial intelligence (AI) applications in drug discovery and drug delivery: Revolutionizing personalized medicine. Pharmaceutics. 2024;16(10):1328. https://doi.org/10.3390/pharmaceutics16101328
CrossRef - Singh S, Kaur N, Gehlot A. Application of artificial intelligence in drug design: A review. Comput Biol Med. 2024;179:108810. https://doi.org/10.1016/j.compbiomed.2024.108810
CrossRef
Abbreviations list
AI – Artificial Intelligence
ML – Machine Learning
DL -Deep Learning
EEG -Electroencephalogram
MRI – Magnetic Resonance Imaging
CT – Computed Tomography
PET – Positron Emission Tomography







