Manuscript accepted on :
Published online on: 06-01-2016
Plagiarism Check: Yes
Arif Yezdani1
Professor in Dept. of Orthodontics and Dentofacial Orthopaedics, Bharath University, Sree Balaji Dental College and Hospital, Narayanapuram, Pallikaranai, Chennai-600100
DOI : https://dx.doi.org/10.13005/bpj/708
Abstract
This case report illustrates the fact that rapid orthodontic tooth movement occurs when selective alveolar decortication is done. This in conjunction with bone graft enhances the bone volume, corrects the fenestrations and bony dehiscence and expands the limits of orthodontic tooth movement. A 24 year-old male patient presented with a Class II Division I malocclusion on a skeletal Class I base with increased bi-maxillary dento-alveolar protrusion with unilateral maxillary posterior cross-bite on the left side. Pre-adjusted edgewise appliance, Roth’s prescription,(0.022 x 0.028 inch slot), was strapped a week prior to the surgical procedure. Full thickness labial and lingual flaps were reflected in the maxillary arch only and the alveolar bone was selectively de-corticated and augmented with an osseograft. Orthodontic treatment was commenced a week post-surgery and adjustments were done fortnightly. The duration of the treatment was about 9 months. The rapid correction of the malocclusion in one-third the treatment time required for conventional orthodontics was as a result of regional acceleratory phenomena triggered by bone activation. The augmentation with the bone graft further enhanced the bone volume required for the expansion of the constricted maxilla without the intervention of any orthopedic device.
Keywords
alveolar bone activation; osseograft; rapid orthodontic treatment
Download this article as:| Copy the following to cite this article: Yezdani A. Alveolar bone shaping and augmentation – A prelude for rapid orthodontics. Biomed Pharmacol J 2015;8(October Spl Edition) |
| Copy the following to cite this URL: Yezdani A. Alveolar bone shaping and augmentation – A prelude for rapid orthodontics. Biomed Pharmacol J 2015;8(October Spl Edition). Available from: http://biomedpharmajournal.org/?p=3550> |
Introduction
Wilcko et al have explicitly documented that subsequent to labial and lingual alveolar decortication, there has been rapid orthodontic tooth movement.1 They have reported that the accelerated orthodontic tooth movement with corticotomy facilitated orthodontics was more as a result of demineralization-remineralization phenomena triggered by regional acceleratory phenomena (RAP) wherein the increased osteopenia due to increased osteoclastic activity resulted in decrease in density of bone with no change in bone volume.2 However, rapid tooth movement subsequent to corticotomy surgery has been reported for over half a century.3-7
Ferguson et al, 8 reported on orthodontic treatment in combination with bone activation and particulate bone grafting material called Accelerated Osteogenic Orthodontics (AOO) wherein osseous insults in the form of corticotomy cuts or perforations were extended only barely into the medullary bone on both the labial and lingual plates. This is in contradistinction to the “bony block” movement advocated by Kole.3
Alveolar bone augmentation corrects the alveolar fenestrations and bone dehiscences and this could be done with anyone of the grafting materials like, a mixture of demineralized freeze dried bone allograft (DFDBA) and bovine bone, 100% (DFDBA) or alloplast. The combined effects of these 2 techniques- namely selective alveolar decortication and alveolar augmentation alongwith normal orthodontic treatment produces rapid tooth movement with shortened duration time. Animal experiments too demonstrated an increase in apposition and resorption of alveolar bone adjacent to the corticotomy site. 9, 10, 11
This case report validates the use of this AOO procedure to correct the Class II division 1 malocclusion and the constricted maxillary dental arch.
Materials and methods
A male patient, aged 24 years, presented with forward placement of maxillary and mandibular anteriors with constricted maxillary dental arch.
Extra-oral assessment (Fig.1a-c).
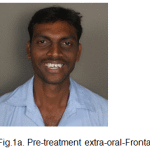 |
Figure 1a: Pre-treatment extra-oral-Frontal |
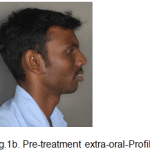 |
Figure 1b: Pre-treatment extra-oral-Profile |
 |
Figure 1c: Pre-treatment extra-oral-Smiling |
The patient had a leptoprosopic face, convex profile, posterior divergence, slight asymmetry of the face, incompetent lips with lower lip redundant and everted, deep mentolabial sulcus, average clinical mandibular plane angle, nonconsonant smile arc with no signs of temporomandibular joint dysfunction.
Intra-oral assessment (Fig. 1d-h).
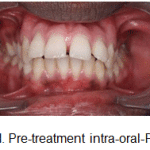 |
Figure 1d: Pre-treatment intra-oral-Frontal |
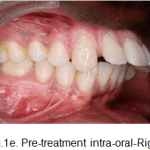 |
Figure 1e: Pre-treatment intra-oral-Right |
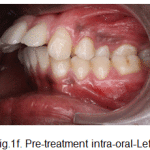 |
Figure 1f: Pre-treatment intra-oral-Left |
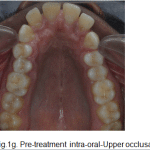 |
Figure 1g: Pre-treatment intra-oral-Upper occlusal |
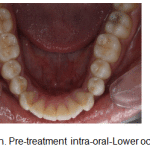 |
Figure 1h: Pre-treatment intra-oral-Lower occlusal |
Oral hygiene was satisfactory. Maxillary arch was V-shaped with proclined maxillary incisors and spacing. Mandibular arch was V-shaped with proclined and mildly rotated mandibular incisors. Curve of spee was 3mm.
In occlusion, increased overjet with developing anterior open bite was observed. It was an Angles’ Class II division 1, subdivision malocclusion with end-on molar relation on left side with class 1 molar relation on right side with a class I canine relation on right side and end-on relation on left side, with an unilateral posterior cross bite on left side.
Radiographic assessment
The panoramic radiograph confirmed the presence of all permanent teeth, and normal alveolar bone levels. (Fig 2).
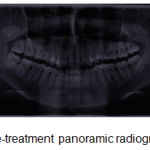 |
Figure 2: Pre-treatment panoramic radiograph |
Lateral cephalometric analysis, revealed a skeletal Class I pattern with an orthognathic maxilla and orthognathic mandible,with an average mandibular plane angle and severely proclined maxillary and mandibular incisors. (Fig. 3).
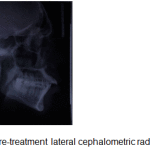 |
Figure 3: Pre-treatment lateral cephalometric radiograph |
CBCT revealed the asymmetry of the face with a vertically short ramus on the left side. (Fig.4, Fig. 5).
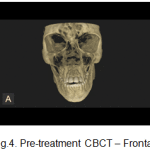 |
Figure 4: Pre-treatment CBCT – Frontal |
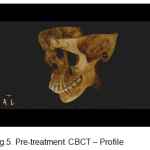 |
Figure 5: Pre-treatment CBCT – Profile |
Aims and Objectives
- Improve facial profile and smile esthetics.
- Correction of constricted maxillary dental arch and maxillary unilateral posterior cross bite on left side.
- Correction of protruded maxillary and mandibular teeth.
- Correction of spacing in maxillary teeth.
- Correction of rotated mandibular teeth.
The patient opted for AOO, as the treatment would be completed in one-third to one fourth the treatment time required for conventional orthodontics.
Pre Adjusted Edgewise Appliance Therapy (0.022 x 0.028 inch slot), Roth’s prescription was strapped up a week prior to the surgical procedure. The patient underwent alveolar de-cortication and alveolar augmentation with osseograft. Maxillary first premolars were extracted during the surgical procedure.
Surgical procedure
Surgery was performed on only maxillary dental arch under local anaesthesia. Labial and lingual sulcular incisions were made using a 12 BP blade except lingually between maxillary central incisors.
With care taken not to disturb the neurovascular bundles exiting the bone, the full thickness flaps were reflected with the interdental papillae intact beyond the apices of the teeth from maxillary right first premolar upto the maxillary left second molars. (Fig. 6).
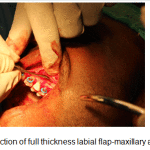 |
Figure 6: Reflection of full thickness labial flap-maxillary anterior view |
The alveolar bone on the labial and lingual aspects of the maxillary teeth from maxillary right first premolar upto the maxillary right second molars were de-corticated with round perforations made with a surgical round bur, barely into the medullary bone accompanied with copious saline irrigation. (Fig.7). Platelet rich plasma, was obtained from the patients’ own blood and the same was mixed with osseograft (Advanced Biotech products (P) Ltd. Chennai, under licence from En Coll Corp. Fremont, CA, USA). Osseograft (DMBM) TM is a bio-resorbable xenograft demineralized bone matrix material. The alveolar augmentation was done with osseograft to a thickness of 2-3mm and the full thickness flaps were then returned to their original position and sutured into place with one interrupted loop 3/0 suture, interproximally. (Fig. 8, Fig.9).
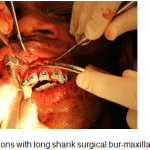 |
Figure 7: Perforations with long shank surgical bur-maxillary left quadrant |
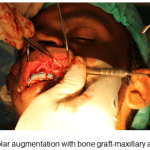 |
Figure 8: Alveolar augmentation with bone graft-maxillary anterior view |
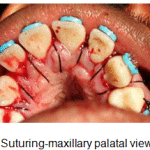 |
Figure 9: Suturing-maxillary palatal view |
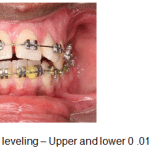 |
Figure 10a: Aligning and leveling – Upper and lower 0 .016 inch NiTi archwires |
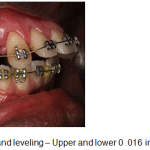 |
Figure 10b: Aligning and leveling – Upper and lower 0 .016 inch NiTi archwires |
Post-surgically Amoxycillin 500mg t.id./week and anti-inflammatory drugs t.i.d/week was given and chlorhexidine mouthwash was advised. A week post-surgery sutures were removed and non-steroidal anti-inflammatory drugs were asked to be discontinued until orthodontic treatment was completed such that these drugs do not interfere with orthodontic tooth movement.
Orthodontic procedure
A week following surgery the first orthodontic adjustment was made and thereafter, adjustments were made every 2 weeks until the completion of treatment. Initial aligning and leveling was done with upper and lower 0.016 NiTi archwires. (Fig.10a-c). Space closure was achieved with NiTi retraction coil springs attached to crimpable hooks on upper 0.017 X 0.025 stainless steel archwire only. (Fig.11a-c). The upper stainless steel archwire was expanded to correct the constricted maxillary dental arch on the left side. Finishing and detailing was accomplished with upper and lower 0.019 X 0.025 stainless steel archwires. (Fig.12).
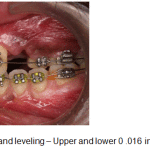 |
Figure 10c: Aligning and leveling – Upper and lower 0 .016 inch NiTi archwires |
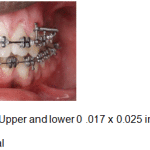 |
Figure 11a: Space closure – Upper and lower 0 .017 x 0.025 inch SS archwires with NiTi retraction springs – Frontal |
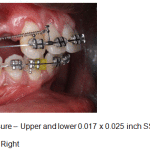 |
Figure 11b: Space closure – Upper and lower 0.017 x 0.025 inch SS archwires with NiTi retraction springs – Right |
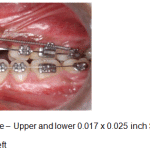 |
Figure 11c: Space closure – Upper and lower 0.017 x 0.025 inch SS archwires with NiTi retraction springs – Left |
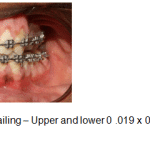 |
Figure 12: Finishing and detailing – Upper and lower 0 .019 x 0.025 inch SS archwires – Frontal |
Results
The patient showed remarkable improvement in correction of the unilateral maxillary posterior cross bite, constricted maxillary dental arch, increased bi-maxillary dento-alveolar protrusion, maxillary spacing, rotated mandibular incisors and developing anterior open bite with an achievement of a class I canine relation on both the sides. (Fig.13a-f). This rapidity of the treatment results was attributed to RAP.
 |
Figure 13a: Post-treatment extra-oral-Frontal |
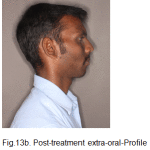 |
Figure 13b: Post-treatment extra-oral-Profile |
 |
Figure 13c: Post-treatment extra-oral-Smiling |
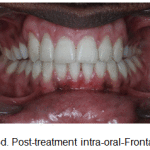 |
Figure 13d: Post-treatment intra-oral-Frontal |
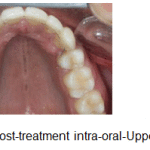 |
Figure 13e: Post-treatment intra-oral-Upper occlusal |
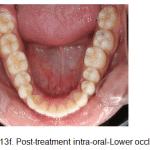 |
Figure 13f: Post-treatment intra-oral-Lower occlusal |
The periodontal alveolar augmentation with osseograft provided an adequate overall alveolar bone volume to facilitate the correction of the malocclusion, more so the unilateral maxillary posterior crossbite on the left side with just the use of archwires only and not the customary orthopaedic rapid palatal expansion appliance which is recommended in such cases. (Fig.13g-i).
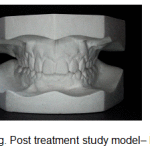 |
Figure 13g: Post treatment study model– Frontal |
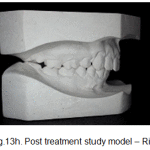 |
Figure 13h: Post treatment study model – Right |
 |
Figure 13 i: Post treatment study model – Left |
Discussion
This case report validates the use of (AOO) procedure highlighted by alveolar bone shaping and augmentation. The de-cortication procedure triggered RAP which, according to reports commences a few days after surgery, peaks between 1-2 months when catabolic and anabolic responses are 3-fold higher, and dissipates to a normal steady state by 11 weeks after surgery.12 The RAP facilitated rapid orthodontic tooth movement and the provision of bone graft provided the necessary bone volume for expansion of the constricted maxillary dental arch. Decortication produces a catabolic process, a resorption response, characterized by osteopenia causing reduction in bone density, with no change in alveolar bone volume.13 The remaining collagenous soft tissue matrix of the bone is transported with the root in the direction of movement termed, “bone matrix transportation”.14 The osteoid matrix gets subsequently re-mineralized by the anabolic process.
Alveolar bone shaping is a physiologically driven process and the intense regional healing response promulgated was utilized to correct the unilateral maxillary posterior cross bite on the left side and the bi-maxillary dento-alveolar protrusion. Bone luxation is contraindicated because it could lead to intra-pulpal and intraosseous morbidity, hence, decortication is done by just perforating the alveolar bone and these perforations provide the necessary bleeding points and communications through which new blood vessels and pluripotential cells migrate from the medullary bone into the cortical plates, differentiate into bone cells which then remove old bone and create new bone and make the cortical plates more vital and responsive to the forces of tooth movement. It has been reported that the primitive uncommitted stem cells become specific cell types in bone morphogenesis under the influence of bone morphogenetic protein15, which stimulates an increase in the osteoblastic activity, resulting in re-mineralization of the soft tissue matrix, after cessation of tooth movement.16 In the AOO procedure, root resorption is minimized due to “bone matrix transportation”.
The Accelerated Osteogenic Orthodontics procedure with the osseograft had significantly improved the structural integrity of the periodontium, and provided additional bone volume to expand the constricted maxillary dental arch. Absence of this increased bone volume on the left side of the maxillary dental arch would have resulted in bony dehiscence subsequent to expansion of the maxillary dental arch. It has been reported that in adults, bony dehiscence formation over the roots after traditional orthodontic therapy, resolves only partially during retention.17 In this case the provision of additional bone volume in the form of bone graft negated this side effect and provided stability and reduced potential for relapse in affirmation with that which has been reported in literature.18
Orthodontic adjustments were performed fortnightly with application of normal orthodontic forces and the constricted maxillary dental arch was expanded with the use of only progressively increasing diameter of stainless steel archwires and use of crossbite elastics. No orthopaedic device was used to expand the constricted maxillary dental arch.
The patient was given a maxillary and a mandibular fixed lingual retainer as a retention appliance, to create an environment to foster alveolar re-mineralization. Therefore, it cannot be denied that periodontal bone activation with alveolar augmentation, alongwith orthodontic tooth movement is in essence “in vivo tissue engineering”.
Conclusion
Accelerated Osteogenic Orthodontics had caused the correction of the malocclusion in less than 9 months. The periodontal alveolar augmentation with the osseograft had caused an increase in alveolar bone volume which provided for an intact periodontium, aiding in the correction of the unilateral maxillary posterior cross bite on the left side alongwith correction of increased bi- maxillary dentoalveolar protrusion. No loss of tooth vitality nor apical root resorption was reported. An adequate zone of gingival attachment and good presence of interdental papillae were the other hallmarks of this procedure. Continued mineralization in the retention period will reduce the risk potential of relapse. An added advantage of this procedure is that due to the reduced duration of the presence of the appliance in the mouth, the incidence of caries and infection is also minimized. AOO is indeed an useful alternative treatment modality for those patients who desire orthodontic treatment but prefer shortened duration time.
References
- Wilcko MW, Ferguson DJ, Bouquot JE, et al: Rapid orthodontic de-crowding with alveolar augmentation: case report, World J Orthod 2003;4:197-205.
- Wilcko MW, Wilcko MT, Bouquot JE, Ferguson DJ. Rapid orthodontics with alveolar reshaping: Two case reports of decrowding. Int J Periodontics Restorative Dent 2001;21:9-19.
- Kole H .Surgical operations of the alveolar ridge to correct occlusal abnormalities. Oral Surg Oral Med Oral Pathol 1959;12:515-529
- Generson RM, Porter JM, Zell A, Stratigos GT. Combined surgical and orthodontic management of anterior open bite using corticotomy. JOral Surg 1978;34:216-219.
- Anholm M, Crites D, Hoff R, Rathbun E. Corticotomy-facilitated orthodontics. Calif Dent Assoc J 1986;7:8-11.
- Gantes B, Rathbun E, Anholm M. Effects on the periodontium following corticotomy-facilitated orthodontics. Case reports. J.Periodontol 1990;61:234-238.
- Suya H. Corticotomy in orthodontics. In:Hosl E, Baldauf A(eds). Mechanical and Biological Basics in Orthodontic Therapy. Heidelberg, Germany; Hutlig Buch,1991:207-226.
- Ferguson DJ, Wilcko WM, Wilcko MT: Selective alveolar decortication for rapid surgical- orthodontic resolution of skeletal malocclusion treatment, in Bell WE, Guerrero c (eds): Distraction osteogenesis of the Facial Skeleton. Hamilton, BC Decker, 2006, pp199-203.
- Goldie RS, King GJ. Root resorption and tooth movement in orthodontically treated, calcium-deficient, and lactating rats. Am J Orthod 1984;85:424-430.
- Sebaoun JD, Ferguson DJ, Wilcko MT,et al: Corticotomie.Alveolaire et traitements orthodontiques rapides. Orthod Fr 2007; 78:217-225.
- Bogoch E, Gschwend N, Rahn B, Moran E, Perren S. Healing of cancellous bone osteotomy in rabbits – Part I: regulation of bone volume and the regional acceleratory phenomenon in normal bone. J Orthop Res 1993;11:285-91.
- Yaffe A, Fine N, Binderman I. Regional accelerated phenomenon in the mandible following mucoperiosteal flap surgery. J Periodontol 1994;65:79-83.
- Ferguson DJ, Wilcko WM, Wilcko TM: Accelerating Orthodontics by Altering Alveolar Bone Density. Good Practice,2:2-4,2001.
- Wilcko TM, Wilcko MW, Bissada NF,An Evidence-Based Analysis of Periodontally Accelerated Orthodontic and Osteogenic Techniques:A Synthesis of Scientific Perspectives. Semin Orthod 2008;14:305-316.
- Fiorellini J, Nevins M. Repair and regeneration of oral tissues: The molecular approach.Postgrad Dent Series 1996;3(2):3-10.
- Nyman S, Karring T, Bergenholtz G. Bone regeneration in alveolar bone dehiscences produced by jiggling forces. J Periodontal Res 1982;17:316-322.
- Fuhrmann R: Three-dimensional evaluation of periodontal remodeling during orthodontic treatment. Semin Orthod 2002;8:23-28.
- Murphy NC: In vivo tissue engineering for orthodontists: a modest first step, in Davidovitch Z, Mah J, Suthanarak S(eds); Biological Mechanisms of Tooth Eruption, Resorption and Movement, Boston, Harvard Society for the Advancement of Orthodontics, 2006:385-410.







