Manuscript accepted on :06-Mar-2019
Published online on: 15-03-2019
Plagiarism Check: Yes
Reviewed by: Yuvaraj Sujin
Second Review by: Telmo Pereira
Final Approval by: Dr. Ayush Dogra
Medvedev I. N.
Russian State Social University, Moscow, Russia.
Corresponding Author E-mail: ilmedv1@yandex.ru
DOI : https://dx.doi.org/10.13005/bpj/1621
Abstract
Ischemic stroke is still a very common disease with quite serious consequences. Modern medicine considers in this regard its main task in the curation of such patients, the maximum possible restoration of the functions of the affected brain and the volume of its control over the body. Due to the rapid development of medicine associated with the emergence of innovative technologies in the field of rehabilitation, hardware methods of rehabilitation today have gone far ahead and have in their arsenal a lot of high-tech tools. For this purpose, a search is being made for means of increasing the activity of brain cells located in the affected area. Of particular importance in this regard are the methods of rehabilitation in the early recovery period after ischemic stroke using robotic methods of mechanotherapy, one of which is the use of the Lokomat system. Among them, a prominent place is occupied by the walking training system - Lokomat, consisting of robotic orthoses and a body support device, which are combined with a treadmill. Information about the successful use of Lokomat during the rehabilitation of patients with movement disorders is still scattered, and this required their generalization and understanding. The main advantage of this system is the ability to effectively control and ensure high intensity, repeatability (reproducibility) and purposefulness of the trained movements. The convincing advantages of automated training on the Lokomat system compared to traditional rehabilitation in terms of various clinical indicators in patients with post-stroke hemiparesis have been identified. It was shown that in patients trained on the Lokomat system, a single support on the paretic leg intensified, which contributed to a more symmetrical gait. This system is more than other devices and technologies designed for learning to walk, in line with the modern approach to the restoration of impaired motor functions. The inclusion of training sessions on the Lokomat robotic system in the comprehensive treatment of patients with post-stroke hemiparesis leads to a marked improvement in movement skills. This is associated with a pronounced restructuring against the background of its use of the motor stereotype of walking, which makes it possible to increase the effectiveness of recreational activities in post-stroke patients.
Keywords
Brain Damage; Ischemic Stroke; Lokomat; Rehabilitation; Restoration of Functions
Download this article as:| Copy the following to cite this article: Medvedev I. N. Place and Possibilities of the Robotic System Lokomat in the Rehabilitation of Patients After Ischemic Stroke. Biomed Pharmacol J 2019;12(1). |
| Copy the following to cite this URL: Medvedev I. N. Place and Possibilities of the Robotic System Lokomat in the Rehabilitation of Patients After Ischemic Stroke. Biomed Pharmacol J 2019;12(1). Available from: https://bit.ly/2XXhmAM |
Introduction
To date, the stroke remains one of the most important reasons for the high pathological abnormalities, disability and mortality.1 In addition to a large medico-social damage, stroke also causes significant economic damage, as very often it develops in people of working age. For these reasons, the present researchers special attention is paid to acute circulatory disorders, developed on the background of stenosis of the cerebral arteries.2
Considering the rather severe consequences of ischemic stroke, modern medicine considers physical rehabilitation as the main task for the curation of such patients, that is, the maximum possible restoration of the functions of the affected brain and the amount of its control over the body. To this end, various means are being sought to increase the activity of brain cells located in the affected area.3
Of particular importance in this regard are the methods of rehabilitation in the early recovery period after ischemic stroke using robotic methods of mechanotherapy, one of which is the use of the Lokomat system.4 This approach to rehabilitation is gathering more and more supporters as more information is accumulated on its successful use during the rehabilitation of patients with post-stroke hemiparesis.5
Various advantages of automated training on the Lokomat system were revealed in relation to traditional rehabilitation in terms of the clinical parameters of walking in patients with post-stroke hemiparesis.6 In patients who received training on the Lokomat system, the duration of a single support on the paretic leg increased, which contributed to a more symmetrical gait.7 At the same time, information on the successful use of Lokomat in the course of rehabilitation of patients with movement disorders is still very fragmented, and this requires their generalization and reflection to create recommendations on the use of this rehabilitation complex in patients who have had ischemic stroke and with varying degrees of neurological deficit.
The purpose of the study is to summarize and examine information about the effectiveness of rehabilitation of patients with ischemic stroke, evaluating the place in her mechanotherapy using hardware Lokomat.
Modern View on the Problem of Ischemic Stroke
Stroke is an acute violation of cerebral circulation in a particular arterial pool, which leads to the appearance of a focus of necrosis in the brain tissue and is accompanied by persistent pronounced neurological deficit. Currently, stroke is a very common form of disorders of cerebral circulation. In Russia, the mortality rate from this disease remains one of the highest in the world, with more than 400000 cases of stroke annually recorded, which, if not fatal, lead to persistent disability.8
The main risk factors for the development of ischemic stroke are usually attributed9: atherosclerosis, its combination with untreated hypertension; diabetes; tobacco smoking; obesity, hyperlipidemia; history of thromboembolism; male gender (men have strokes more often) and old age.
The pathogenesis of stroke is based on the “ischemic cascade,” which develops during an ischemic stroke during 8 stages10:
first: the reduced blood flow to the top of the ischemic threshold;
second, the Hyper-production of glutamate (an amino acid which in large quantities has a toxic effect on the brain).
third: the development of the phenomena of edema of brain tissue (due to the impact of glutamate in the cells begins to accumulate water, sodium, calcium);
fourth: activation of intracellular enzymes, thereby increasing the sensitivity to glutamate;
fifth: the increase of NO synthesis, which leads to dilatation of the vascular wall and affects the inflow and outflow of blood in brain tissue;
sixth: a flood in the blood level of the inducers of apoptosis.
seventh: the transformation of ischemia to hemorrhage (change in haemorrhagic stroke) -it happens not always.
eighth: apoptose activation and massive cell death.
Very often, possible acute onset of illness with rapid neurological symptoms, and neurological deficit. Thus the patient can clearly indicate the start time of their illness. This condition is quite common for embolic stroke option, especially if there is a patient of atrial fibrillation. It is also possible unduliruûŝie beginning: symptoms of brain damage are fluctuating in nature and gradually increase in time. Possible often tumor-like beginning: ischemia increases slowly, affecting extensive areas of the brain. The result is a detailed stroke with a large lesion of the brain tissue.10
The first signs of a stroke are: impaired or impaired speech, severe headache that does not come after taking neuroprotectors and vasoactive drugs, weakness and numbness of half of the body, severe dizziness, accompanied by nausea and vomiting, loss of orientation in space, time and self, sudden blindness in one eye or loss of visual fields.11
There are the following options for stroke12:
Cardioembolic: emboli are blood clots that form in the heart cavity during atrial fibrillation, mitral heart disease, or after a recent myocardial infarction;
Atherothrombotic: an atherosclerotic plaque builds up in the lumen of large arteries, which then ulcerates and thrombi form at this place;
Hemodynamic: stroke develops on the background of stenosis of about 70% of intracranial and extracranial vessels in combination with a sharp drop in blood pressure;
Hemorheological: thrombosis in the vessels of the brain occurs due to hematological diseases with symptoms of hypercoagulation – erythremia or thrombocythemia;
Lacunar infarction: thrombosis of cerebral arterioles in the subcortical nuclei. The diameter of the lesion is often 15 mm and is characterized by a specific clinic and therefore is allocated in a separate group.
The main ones in the localization of a lesion are vascular basins10: carotid pool (internal carotid artery; anterior cerebral artery; middle cerebral artery) and vertebrobasilar basin (vertebral; basilar artery; cerebellar arteries; posterior cerebral artery; thalamus vessels). The lesion clearly corresponds to the specific vascular basin in which the brain catastrophe occurred (Figure 1). However, regardless of the lesion, cerebral symptoms appear in the form of depression of consciousness, headache and dizziness. It is more pronounced with extensive hemispheric infarctions, cerebral and cerebellar infarctions.
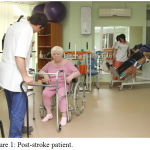 |
Figure 1: Post-stroke patient.
|
In the development of ischemic stroke decided to allocate the following periods12:
The most acute is the first 3 days. In the acute period, the leading value is given to the first three hours after the onset of cerebral catastrophe – the so-called therapeutic window (it is during this period of time that it is possible to actively and drastically influence the course of a stroke by conducting thrombolytic therapy;
Sharp – up to 28 days. If the neurological deficit regresses to 21 days, then this condition is regarded as a minor stroke;
Early recovery – up to six months;
Late recovery – up to 2 years;
The period of residual manifestations is more than 2 years.
Thus, ischemic stroke is a very dangerous disease that can lead to disadaptation of a person and his persistent disability or death. In this regard, their timely and effective rehabilitation, which is able to give them a chance for the maximum possible recovery of their lost functions, is of particular importance for these patients.
Basics of rehabilitation for patients with ischemic stroke
It is recognized that rehabilitation after an ischemic stroke should include a complex of active medical, psychological, educational, socio-economic and professional measures aimed at restoring impaired functions and social rehabilitation of patients. The use of neuroprotectors and vasoactive drugs, which increase the degree of recovery of neurological defects, is of great importance when carrying out rehabilitation measures.13
The main goal of rehabilitation of patients undergoing ischemic stroke at the hospital stage and after the patient is discharged from the hospital is the restoration of impaired functions, prevention and treatment of post-stroke complications (pneumonia, bedsores, urinary tract infections, deep vein thrombosis of limbs, arthropathies, septic conditions), walking training and speech, as well as self-service techniques.14
Great impact on the outcome of rehabilitation for ischemic stroke and the degree of restoration of impaired functions has the timeliness of hospitalization of the patient in a medical institution, the intensity of treatment at the hospital stage and the subsequent early admission of the patient to specialized rehabilitation centers. The clarity of the phasing, systematic and long duration of the rehabilitation process, as well as the active participation in the rehabilitation activities of the patient himself, has a strong influence on the prognosis for life, social adaptation and working capacity.15
An important aspect affecting the possibility of a more complete recovery of neurological and mental defects after suffering ischemic stroke, participation in the rehabilitation process of doctors of different profiles – neurologists, speech therapists, neuropsychologists, massage therapists, physiotherapists, social workers, kinesitherapy specialists, occupational therapists, biological specialists feedback with the mandatory complexity and adequacy of rehabilitation measures.16
It is best for the patient in the early recovery period of rehabilitation to get into the local specialized neurological sanatorium, where he will continue recovery of all impairments (motor, sensory, vestibular, neuropsychiatric disorders) with the help of medical gymnastics and physical culture, physiotherapy, massage, mud therapy, acupuncture and treatment with neuroprotective agents and vasoactive drugs.17
The physical exercises of physiotherapy in these patients should be aimed at a gradual increase in range of motion, normalization of increased muscle tone, increasing the ability to arbitrary movements of the muscles in the form of walking, standing and lost skills of domestic self-service.18
In the acute, the acute and early recovery periods, generally dominated by passive movements which stimulate the appearance of active movements, prevent the development of contractures, improve circulation of blood and lymph circulation and optimizes muscle tone. At this time, is to start active training of the patients sitting, standing, walking and self-care.16
In the late recovery period and in the period of residual effects, the use of physical exercises is aimed at improving existing walking skills with resistance training in a vertical posture (Figure 2). Important methods of rehabilitation of such patients are also massage and electrostimulation of the neuromuscular apparatus.19
 |
Figure 2: Classes of therapeutic physical culture with post-stroke patients.
|
The results of the successful restoration of the disturbed functions in patients after ischemic stroke are summarized in the later recovery period. The outcomes of recovery are divided into five classes of recovery20,21:
Thus, the rehabilitation of patients after ischemic stroke should include a complex of active medical, psychological, socio-economic and professional measures aimed at the maximum possible restoration of impaired functions of patients and their social readaptation.
Improving potential of modern hardware rehabilitation tools
Rehabilitation of different categories of post-stroke patients is one of the priorities of modern medicine worldwide.19 It is believed that with a properly selected set of rehabilitation measures, it is often possible to return the patient to an active life.24,25 At present, the use of hardware rehabilitation tools takes a serious place in rehabilitation programs.26
The main indications for hardware rehabilitation are diseases of the spine, joints and muscles, pathology of the central nervous system and peripheral nerves, as well as diseases of the internal organs. With the help of hardware rehabilitation, motor functions are fully restored and metabolic processes are activated, general and local hemodynamics are improved, tissue trophism is enhanced, a general tonic effect is achieved. Proper and effective use of modern hardware, taking into account the use of new technologies in the diagnosis and treatment significantly affects the effectiveness of any rehabilitation measures.27,28
When carrying out rehabilitation measures, an appropriate level of equipment of the material and technical base of medical institutions that solve rehabilitation tasks of different levels is of paramount importance.29,30
On the market today, you can find a huge number of hardware rehabilitation. This method is called mechanotherapy. He showed high potential in terms of restoration or compensation of disturbed functions of the body. It is based on the use of devices that facilitate movement, or increase simultaneously the efforts for their implementation. It is successfully used in combination with other methods of medical rehabilitation.31,32
The history of the development of mechanotherapy began in the nineteenth century, when Gustav Zander, Professor of Uppsala University (Sweden), created a system of gymnastics, which he called machine. G. Zander had a deep knowledge of gymnastics counter and thought that since this gym depends entirely on the practitioner, it is difficult to expect accurate dosage of resistance. He developed a special apparatus that gave the opportunity to more accurately dosed exercise without practitioner. Mechanical devices Zander quickly became widespread throughout the world.30
The basis of mechanotherapy are dosed rhythmically repeat the exercise on special machines with the aim of restoring joint mobility (on pendulum), facilitate the movements and strengthening muscles (on block type) and General health (isokinetic machines). Exercises have a positive impact on certain joints or muscle groups and can be dosed in the ratio of the amplitude of motion, the drag force and rate with the help of special devices.33
It is proved that the local impacts of the different apparatuses excitation occurs proprioceptors and Central zones of the engine analyzer. The result is a broad impact on the whole organism through the autonomic nervous system (figure 3). This mechanism metronomically and motorotonic reflexes to exercising limbs increases blood flow.34,35 Long weak rhythmic irritation provide a total concentration of excitation in the nervous centers, through the irradiation and induction leads to the emergence or strengthening of the reflex motor discharge. The cyclical nature of muscle activity during classes contributes to the improvement of voluntary regulation of contraction and relaxation of the muscles and also lead to an increase in muscle strength.36,37
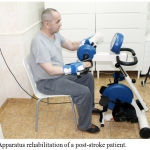 |
Figure 3: Apparatus rehabilitation of a post-stroke patient.
|
According to the purpose, the rehabilitation equipment can be divided into a number of main groups38: the device is mainly a local impact on individual muscle groups and joints of the extremities – mechanotherapy equipment (simulators); more complex devices for training global motor acts and functions of the main internal organs (cardiovascular and respiratory systems) – cardiovascular equipment; electronic-computer complexes, with the help of which the monitoring of the training of various physiological functions is carried out on the basis of the principle of biological feedback – devices for complex diagnostics of movements Tergumed 3D, Biodex System; devices designed to mobilize patients – the Erigo verticalizer, the Lokomat robotic orthopedic device for restoring the skills of walking, the equipment for moving patients (elevator).
According to the method of motor activation, all hardware is divided into36: devices of active action; passive devices; robotic devices active-passive action.
The basis of the apparatus of active action, or simulators, is to obtain a mechanotherapeutic effect due to the patient’s own muscular activity. The use of sports simulators in rehabilitation has limitations. This is due to the fact that the loads used in them do not have low thresholds that are permissible for patients. Adjustment of sports simulators is possible only within the limits originally characteristic of a healthy person. This drawback is overcome in specialized simulators. Unlike sports, they are designed taking into account the physical condition of the patient and the possible presence of comorbidities.39,40
The main task of mechanotherapy on the devices of passive action – an increase in mobility in an isolated joint is solved by dosed stretching of soft paraarticular tissues with maximum muscle relaxation. Effectiveness is due to the fact that passive movement is performed according to an individually selected program without active contraction of the periarticular muscles (joint stabilizers).41 The advantage of such devices over other types of mechanotherapy is the possibility of their earlier use. Apparatus of passive action provides the possibility of mechanical stretching of tissues with muscle spasticity, which helps to eliminate articular contractures.42,43
At the same time, patients with bed rest need regular physical exertion to prevent secondary complications, including pneumonia, pressure sores, dysfunction of the pelvic organs and thromboembolic complications.44,45
Means of active-passive exposure can prevent unwanted complications. First of all, they include specialized robotic systems,36,46 in particular, Erigo. It allows the patient to verticalize, cyclic load on the lower limbs using a special inclined table with an integrated robotic orthopedic device having automatic regulation. The Erigo system combines the simultaneous dynamic movement of the lower extremities and the physiological load on them (the movements of the lower extremities correspond to the physiological movement of the hip, knee and ankle joints). This system is used in the early stages of rehabilitation (starting from the first day of the disease). With early patient verticalization, prevention of secondary complications is performed, orthostatic training is performed, the cardiovascular system is activated, and afferent stimulation is intensified.47
Thus, the health potential of modern apparatus for the rehabilitation of post-stroke patients allows them to significantly improve their health, increase the effectiveness of rehabilitation and reduce the risk of potentially possible complications.
The possibility of using the device Lokomat in rehabilitation practice
Methods of physical rehabilitation of post-stroke patients, as a rule, are aimed at teaching the patient the proper walking skills.48 To restore the maximum possible correct gait, they use methods of kinesitherapy and work with specially trained instructors.35 It requires a lot of human, intellectual, physical and economic costs. At present, robotized technologies are introduced into the practice of rehabilitation, which allow not only to reduce costs, but also to exclude the human factor of improper patient education. Special robots use biofeedback mode. It allows you to estimate the percentage of the patient performing active or passive movements, “imposed” by the robot.49
Among physical methods, the modern mechanized robots Lokomat simulators come out on top in the 21st century. These are robotic orthopedic devices for restoring walking skills. Lokomat is able to provide external mechanical control of the movements of the lower limbs, regardless of the level of consciousness and movement control by the patient (Figure 4). The action of the system contributes to the restoration and preservation of joint mobility. It provides prevention and treatment of dystrophic processes in soft tissues and prevents osteoporosis.50
 |
Figure 4: Post-stroke patient rehabilitation using Lokomat.
|
The Lokomat robot is a slave gait orthosis that automates movement therapy on a treadmill and increases the effectiveness of learning to walk after injury and stroke. The use of Lokomat significantly improves the results of therapy, providing a high intensity of individual rehabilitation, using the principle of feedback.49
There are 2 models of Lokomat: Lokomat Pro and Lokomat Nanos.50 Lokomat Pro has the perfect compact equipment. It has a wide feedback function and a touch screen. In addition to Lokomat Pro, a more compact version of the device –Lokomat Nanos was created. Like Lokomat Pro, it can increase the effectiveness of rehabilitation. It is suitable for outpatient and non-ambulatory conditions. Thanks to its compact format, Lokomat Nanos is designed for small spaces and is suitable for rooms that have a ceiling height of 240 cm. Despite its compact size, the simulator is provided with all the necessary functionality for effective rehabilitation. Exercise occurs in single mode under the supervision of an operator. The main indicator of improved walking in classes is to increase the accuracy of movements and increase motivation through visualized feedback.51
Pledged feedback tools in both versions of Lokomat display walking activity in real time and provide a high level of patient motivation. By walking on a treadmill, the patient receives the necessary information from the receptors of the lower extremities, which allows him to re-successfully form the skills of motor activity.52
The computer-controlled robotic Lokomat engines are precisely synchronized with the speed of the treadmill (range from 1 to 3.2 km / h). They set the patient’s foot to a trajectory of movement that is close to the physiological pattern of walking. The user-friendly computer interface allows the therapist to effortlessly control Lokomat and adjust the workout parameters according to the needs of each patient.
New competitive programs increase long-term patient motivation. Lokomat Pro game programs offer exciting exercises that increase patient motivation and activity, providing elements of competition with an intuitive assessment system. Functional enhanced feedback motivates the patient to improve walking parameters.53
The real-time adaptive intensity of the mechanical assistance to movement contributes to a more active participation of the patient in rehabilitation. An integrated feedback system monitors the patient’s gait and is visually displayed in real time, increasing the patient’s motivation and encouraging him to actively participate.54
Thus, Lokomat is a modern robotic orthosis that performs the physiological movements of the lower extremities especially effectively in post-stroke patients with impaired walking, which increases the success of their rehabilitation.
Conclusion
Thanks to the rapid development of medicine that is associated with the emergence of innovative technologies in the field of regenerative medicine, hardware and methods of rehabilitation today has gone far ahead and have at their disposal a variety of high-tech means. Among them the visible place is occupied by the system for walk training–Lokomat, consisting of robotic orthoses and devices to support the body, combined with a treadmill. The main advantage of this system is the ability to effectively control and provide high-intensity, consistency and focus of train movements. This system to a greater degree than other devices and technologies designed for learning to walk, meets the modern approach to restoration of disturbed motor functions. The inclusion of training on the Lokomat robotic system in complex treatment of patients with post-stroke hemiparesis results in significant and early improvement of their movement skills. This is due to the significant positive restructuring against the background of its use, movement patterns walk, reflected in the significant improvement in the temporal parameters of the step, and improve the kinematics of walking, which significantly improve the efficiency of health measures in post-stroke patients.
Acknowledgements
The author(s) received no specific funding for this work.
References
- Skoryatina I. A and Yu S. Z. Ability to aggregation of basic regular blood elements of patients with hypertension anddyslipidemia receiving non-medication andsimvastatin. Bali Medical Journal 2017;6(3):514-520. DOI:10.15562/bmj. v 6i 3.553.
- Mikhaylova I. V and Makhov A. S. Introducing chess education in Russian school system: Theoretical and practical aspects. Teoriya i Praktika Fizicheskoy Kultury. 2018;(5):53-55.
- Yushchuk S. A and Abdrakhmanov A. D. Non-drug methods of rehabilitation of patients after cerebral stroke (literature review). Young scientist. 2016;29:215-219.
- Yu V. P and Getzman Y. A. Methods of using LOKOMAT for the rehabilitation of patients with movement disorders. Novosibirsk. 2012;21
- Bulow M., Speyer R., Baijens L and Woisard V. Neuromuscular electrical stimulation in stroke patients with oral and pharyngeal dysfunction. Dysphagia. 2012;23(3):302-303.
CrossRef - Schumacher G. I., Romashin O. V., Sidyakina I. V. et al. Staged physical rehabilitation of post-stroke patients. Methodical recommendations for doctors. Moscow. 2012;44.
- Chernikova L. A. New technologies in the rehabilitation of stroke patients. Nervous diseases. 2005;2:32-35.
- Kadykov A. S., Shakhparonov N.V and Chernikova A. Rehabilitation of neurological patients. Moscow. 2009;49-61.
- Kuznetsov A. N and Vinogradov O. I. Ischemic stroke: diagnosis, treatment, prevention. Moscow. 2009;47.
- Vibers D. O., Feigin V. L and Brown R. D. Stroke: clinical guide. Moscow. 2005;607.
- Gusev E. I and Kamchatnov R. Plasticity of the nervous system. Journal of Neurology and Psychiatry. 2004;3:73-78.
- Gusev E. I. The problem of stroke in Russia. Journal of Neurology and Psychiatry. S. Korsakova. 2003;9:3-5.
- Skoryatina I. A and Yu S. Z. A Study of the Early Disturbances in Vascular Hemostasis in Experimentally Induced Metabolic Syndrome. Annual Research & Review in Biology. 2017;15(6): 1-9. doi: 10.9734/ARRB/2017/34936.
CrossRef - Glagoleva T. I and Zavalishina S. Y. Aggregation of Basic Regular Blood Elements in Calves during the Milk-feeding Phase. Annual Research & Review in Biology. 2017;17(1):1-7. doi: 10.9734/ARRB/2017/34380.
CrossRef - Skoryatina I. A., Zavalishina S. Y.,Makurina O. N., Mal G. S and Gamolina O. V. Some aspects of Treatment of Patients having Dislipidemia on the Background of Hypertension. Prensa Med Argent. 2017;103. doi: 10.4172/lpma. 1000250.
CrossRef - Epifanov V. A. Medical rehabilitation. Moscow: MEDpress-inform. 2005;92-106.
- Ivanova G. E. Medical rehabilitation in Russia. Development prospects. Journal of Restorative Medicine. 2013;5:3-8.
- Ivanova G. E., Shklovsky V. M and Petrova E. A. Principles of the organization of early rehabilitation of patients with stroke. The quality of life. The medicine. 2006;2:62-70.
- Apanel E. N. Neuropathological and physiological basis for the recovery of post-stroke patients. Medical news. 2003;10:23-30.
- Stroke: diagnostics, treatment, prophylaxis. Under the editorship of Suslina Z. A., Piradov A. Moscow: Medpress-inform. 2008;288.
- Glagoleva T. I and Zavalishina S. Y. Physiological Peculiarities of Vessels’ Disaggregating Control over New-Born Calves’ Erythrocytes. Annual Research & Review in Biology. 2017;19(1):1-9. DOI: 10.9734/ARRB/2017/37232.
CrossRef - Isanova V. A. New innovative technologies of medical and social rehabilitation in the conditions of multidimensional rehabilitation institutions. Kazan. 2007;27.
- Sizov A. A. Investigation mistakes in investigation of crimes of foreign citizens, committed in the territory of Russia. Biosciences Biotechnology Research Asia. 2015;12(1). http://www.biotech-asia.org/?p=5452>
- Shmeleva S. V., Yunusov F. A., Morozov Y. U. S., Seselkin A. I and Zavalishina Y. S. Modern Approaches to Prevention and Correction of the Attorney Syndrome at Sportsmen. Prensa Med Argent. 2018;104:2. DOI: 10.4172/0032-745X. 1000281.
- Morozova E.V., Shmeleva S. V., Rysakova O. G., Bakulina E. D and Zavalishina S. Y. Psychological Rehabilitation of Disabled People Due to Diseases of the Musculoskeletal System and Connective Tissue. Prensa Med Argent. 2018;104:2. DOI: 10.4172/0032-745X. 1000284.
- Baranov V. V and Nikulin A.V. the Use of hardware methods and means of rehabilitation. Doctor.Ru. 2009;7(51):20-26.
- Батышева Т. Т., Скворцов Д. В., Труханов А. И. Современные технологии диагностики и реабилитации в неврологии и ортопедии. Москва: Медика. 2005;2005.-256.
- Sizov А. А and Zavalishina S. J. Russian Criminal Legislation in Prevention of Sexually Transmitted Diseases in the Territory of the Russian Federation. Biology and Medicine (Aligarh). 2015;7(5):5. BM-142-15.
- Bikbulatova A. A and Andreeva E. G. Dynamics of Platelet Activity in 5-6-Year Old Children with Scoliosis Against the Background of Daily Medicinal-Prophylactic Clothes’ Wearing for Half A Year. Biomed Pharmacol J. 2017;10(3). Available from: http://biomedpharma journal.org/?p=16546.
- Belova A. N and Shchepetova O. N. Guidelines for the rehabilitation of patients with movement disorders. Moscow. 1998;224.
- Belova A. N. Moscow. 2002;736.
- Zavalishina S. Y. Restoration of Physiological Activity of Platelets in New-Born Calves With Iron Deficiency. Biomed Pharmacol J. 2017;10(2):711-716. DOI: http://dx.doi.org/10.13005/bpj/1160.
CrossRef - Weiner E. N. Therapeutic physical training. Moscow. 2009;424.
- Zavalishina S. Y. Physiological Dynamics of Spontaneous Erythrocytes’ Aggregation of Rats at Last Ontogenesis. Annual Research & Review in Biology. 2017;13(1):1-7. DOI: 10.9734/ARRB/2017/33616.
CrossRef - Zavalishina S. Y. Physiological Features of Hemostasis in Newborn Calves Receiving Ferroglukin, Fosprenil and Hamavit, for Iron Deficiency. Annual Research & Review in Biology. 2017;14(2):1-8. DOI: 10.9734/ARRB/2017/33617.
CrossRef - Kuzminova T. I., Romanenkova Y .S and Kyzymko M. I. Robotic technologies in neurorehabilitation of patients with vertebrobasilar insufficiency. Young scientist. 2016;12:517-519.
- Bikbulatova A. A. Dynamics of Locomotor Apparatus’ Indices of Preschoolers with Scoliosis of I-II Degree Against the Background of Medicinal Physical Training. Biomed Pharmacol J. 2017;10(3). Available from: http://biomed. pharma. journal.org/?p=16762.
- Kremneva E. I., Konovalov R. N., Krotenkova M. V and Chernikova L. A. Activation of the brain in response to stimulation of the support zones of the foot in healthy individuals and in patients with a history of stroke: MRI study. Abstracts Nevsky radiology forum, St. Petersburg, 2-5 April. 2011;121.
- Kuznetsov A. N., Daminov V. D., Rybalko N. V., Uvarova O. A and Kankulova E. A. Hemodynamic control in the combined use of functional electrostimulation and robotic mechanotherapy in patients in the acute period of ischemic stroke. Journal of Restorative Medicine. 2011;3:27-31.
- Kutafina N. V. Platelet Parameters of Holstein Newborn Calves. Annual Research & Review in Biology. 2017;15(2):1-8. doi: 10.9734/ARRB/2017/35214.
CrossRef - Vorobyeva N. V. Physiological Reaction of Erythrocytes’ Microrheological Properties on Hypodynamia in Persons of the Second Mature Age. Annual Research & Review in Biology. 2017;20(2):1-9. doi: 10.9734/ARRB/2017/37718.
CrossRef - Levin O. S. Violations of walking: mechanisms, classification, principles of diagnosis and treatment. Extrapyramidal disorders. Moscow, MED press-inform. 2002;473-494.
- Skoryatina I. A and Zavalishina S. Y. Impact of Experimental Development of Arterial Hypertension and Dyslipidemia on Intravascular Activity of Rats’ Platelets. Annual Research & Review in Biology. 2017;14(5):1-9. DOI: 10.9734/ARRB/2017/33758.
CrossRef - Makarova M. R and Preobrazhensky V. N. Musculoskel et al programs in patients with acute cerebral circulation, using new medical technologies. Journal of Restorative Medicine. 2013;4:41-42.
- Bikbulatova A. A. Determining the thickness of materials in therapeutic and preventive heat-saving garments. Proceedings of higher education institutes. Textile industry technology. 2014;1(349):119-123.
- Mikhaylova I. V., Makhov A. S., Seselkin A. I and Alifirov A. I. Chess in Russian inclusive education system: Problems and prospects. Teoriya i Praktika Fizicheskoy Kultury. 2018;3:97-99.
- Parfenov V. A and Khasanova D. R. Ischemic stroke. Moscow. 2012;288.
- Klochkov A. S., Telenkov A. A and Chernikova L. A. Pathological locomotor synergies after a stroke and the effect on them of training on the Lokomat system. Physiotherapy, balneology and rehabilitation. 2011;6:31-35.
- Masabaev E. S., Shokutbaeva F. Z and Kabdeshev A. M. The use of IT-technologies in the rehabilitation of post-stroke patients (literature review). Young scientist. 2016;30:111-115.
- Daminov V. D., Zimina E. V., Rybalko N.V and Kuznetsov A. N. Robotic technology to restore the function of walking in neurorehabilitation. Moscow. 2010;128.
- Daminov V. D., Zimina E. V., Kankulova E. A and Kuznetsov A. N. Restoration of walking by the method of stimulation of the brain stem during training on robotized complexes. Journal of Restorative Medicine. 2010;6:55-59 .
- Sidyakina I. V. Medical rehabilitation programs in the acute period of stroke. Bulletin of the Medical Dental Institute. 2011;3(18):30-34.
- Sidyakina I. V., Ivanov V. V., Lyadov K. V. Modern technologies in neurorehabilitation. Second National Congress “Stroke and Cerebrovascular Disorders”. Ukraine, Kiev. 2010;3-5.
- Rybalko N. V. Rehabilitation treatment of patients in the acute period of ischemic stroke using the technology of robotic mechanotherapy. Thesis for the degree of candidate of medical sciences. Moscow. 2009;122.







