Manuscript accepted on :October 04, 2017
Published online on: --
K. Aravind1 and Ashish R. Jain2
1Department of Prosthodontics, Saveetha Dental College and Hospitals,Saveetha University, Chennai, India.
2Department of Prosthodontics, Saveetha Dental College and Hospitals, Saveetha University, Chennai, India.
Corresponding Author E-mail: dr.ashishjain_r@yahoo.com
DOI : https://dx.doi.org/10.13005/bpj/1312
Abstract
Maxillary defects can be rehabilitated with conventional simple obturator prosthesis. However, inadequate retention, stability and support may be associated with the use of an obturator. Rehabilitating a patient with a maxillary defect is a challenging problem to the prosthodontist. Precision attachments have been used to retain obturators for some time. The use of precision attachments in a dentate maxillectomy patient can yield significant functional improvement while maintaining the obturator’s aesthetic advantages. Hence, the design of the obturator should create an artificial barrier between the oral and nasal cavities and thereby restore the functional capabilities of speech, mastication and swallowing. In dentate patients, the obturator prostheses could be designed to use the available teeth and bearing tissue to achieve maximum retention and stability, whereas in completely edentulous patients the support is taken only from the remaining bone, it is of utmost importance to take care of what is remaining, while keeping in mind what is lost. This article describes prosthetic rehabilitation of a maxillary defect with obturator using precision attachment as an aid in the retention of the hollow bulb in a completely edentulous patient.
Keywords
Maxillary Defect; Obturator; Precision Attachment; Retention; Stability
Download this article as:| Copy the following to cite this article: Aravind K, Jain A. R. Precision Attachment Retained Palatal Obturator in A Completely Edentulous Patient: A Case Report. Biomed Pharmacol J 2017;10(4). |
| Copy the following to cite this URL: Aravind K, Jain A. R. Precision Attachment Retained Palatal Obturator in A Completely Edentulous Patient: A Case Report. Biomed Pharmacol J 2017;10(4). Available from: http://biomedpharmajournal.org/?p=17455 |
Introduction
Rehabilitating a patient with a maxillary defect is a challenging problem to the prosthodontist. These patients encounter difficulty in not only speech and esthetics but more importantly in mastication and good nutrition.1
The success of an obturator is dependent upon its good retention, stability and support while at the same time it must provide for a good seal to prevent leakage of fluids from the oral cavity into the nasal cavity. Fabrication of a prosthesis requires proper planning and should be designed to achieve its objectives while, at the same time have good patient satisfaction.2-3
Brown et al classified maxillary defects based on their vertical and horizontal extent.4 This classification is helpful in deciding the design for a patient requiring a palatal obturator. The design of the prosthesis can either be a single piece with the hollow bulb attached to the denture base or two piece obturator with the hollow bulb being detachable from the denture base. The primary goal of prosthetic obturation is closure of the maxillectomy defect and separation of the oral cavity from the sino-nasal cavities in order to prevent hyper-nasal speech and liquid leakage into the nasal cavity.4 The prosthesis should also improve mastication, swallowing, articulation and speech intelligibility, restore facial contours and reduces drooling. Advantage of two-piece hollow obturator is that it is more hygienic and easy to handle. A hollow bulb obturator allows fabrication of a light weight prosthesis that is readily tolerated by the patient while effectively extending into the defective areas. An often encountered problem with open hollow obturators is the tendency to accumulate nasal secretions which lead to foul odour and added weight. This necessitates frequent cleaning of the obturator and greater discomfort to the patient. Additionally, it is difficult to polish and clean the internal surface from saliva, mucous crusts, and food accumulation. Where as in closed hollow bulb obturators, pooling of moisture is eliminated.5 Another advantage of these prostheses is that, it can be designed to extend superiorly into the defect, thereby reducing the air space and increasing the retention.
The use of hollow bulb obturator has been reported to improve speech resonance as well as decrease the weight of the prosthesis. This in-turn minimises the downward displacement of the prosthesis due to gravity or function. Nonetheless, the bulb must be carefully fabricated to achieve an adequate seal and partition between the oral and nasal cavities so as to prevent leakage of fluid from the oral cavity into the nasal cavity. However, sometimes, patients experience problems with the path of insertion. In such cases, a two-part design may have to be considered to overcome this problem. In a two part obturator, magnets have been used to join the bulb with the denture base.6
In the present case, we report the use of a precision attachment as an aid in the retention of the hollow bulb in a completely edentulous patient.
Case Report
A female patient aged about 45 years, reported to the Department of Prosthodontics, Saveetha Dental College and Hospital, for the restoration of the palatal defect subsequent to a surgery performed for the removal of a maxillary tumour on the right side of the maxilla. The defect extended from the buccal mucosa to the mid-palatine region medially and anteriorly from the premolar region to the posterior extent of the hard palate. The defect was classified as class 2A according to Brown’s classification. (Figure 1a, 1b, 1c, 1d). The patient had partially edentulous maxillary and mandibular arches along with the presence of a few root stumps. The teeth present were 11,12, 32, 33 and 21, 34, 35, 42, 43, 44, 45 (Root stumps). Patient had no relevant medical history. Since the patient required a comprehensive rehabilitation procedure to close the defect as well as a prosthesis to replace her missing teeth, it was decided to extract her remaining teeth and the retained root stumps followed by the fabrication of a complete denture along with the palatal obturator. Since the palatal area available for denture retention was reduced on account of the acquired defect, it was considered that a base metal denture base would be more effective than the conventional acrylic denture base. It was also planned to fabricate the prosthesis as a two piece device with the obturator being attached to the denture base through precision attachments. This design was selected as it would be easier to clean the prosthesis from nasal secretions while at the same time ensuring a good attachment of the hollow bulb with the denture base. The bulb portion would have good retention from the undercuts in the defect. The precision attachment selected was stud attachment. Usually, anchors or stud attachments are indicted in removable partial dentures as a means of providing additional retenion. They are extracoronal attachments which have the matrix part in the denture while the patrix part is usually attached to the crowns of the abutment teeth. This design was adapted in the obturator designed for the patient. The denture base had the matrix part while the bulb portion housed the patrix components. In a completely edentulous patent, the residual maxillary form (ie, amount and contour of the remaining palatal shelf, height of the residual alveolar ridge, configuration and size of the defect, availability of undercuts) determines the degree of obturator movement. In this patient, the size of the defect was not large and hence the stress on the alveolar ridge was also expected to be minimum. Considering the size of the defect, it was planned to utilize two ball attachments. The selected ball attachments (Dalbo) were of 3 mm diameter.
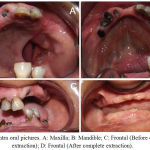 |
Figure 1: Intra oral pictures. A: Maxilla; B: Mandible; C: Frontal (Before complete extraction); D: Frontal (After complete extraction)
|
Procedure
Primary impression of maxillary arch along with defect and the mandibular arch was made using irreversible hydrocolloid (Tropicalgin; Zhermack), and the cast was poured with type III gypsum material (Orthokal; Kalabhai). Subsequently, the special tray was fabricated with light cured acrylic resin (Polytray; Delta Products of India, Mumbai, India), and border moulding was done using a hydrophilic vinyl polysiloxane material (Virtual ® Heavy Body, Ivoclar). The definitive impression was made with vinyl poly siloxane impression material (Elite HD+; Zhermack). The master cast (Orthokal, Kalabhai) of the maxillary impression was duplicated and a refractory cast was poured. An additional cast was duplicated for the fabrication of closed hollow bulb separately (Figure 2a-2i). The adaptation of the metallic denture base to the palate was verified and jaw relation of the patient was then recorded by conventional method. However, intraoral tracing was not done in this case because of the presence of palatal defect (Figure 3a). Subsequently, the models were articulated on a mean value articulator based on the jaw relation recorded earlier. The teeth selection for the patient was done as per the dentinogenic concept and teeth setting was done according to the principles of teeth setting. The trial denture was then readied over the cast denture base and along with the bulb was tried in the patient’s mouth. Adjustments were done such that the occlusal contact between the maxillary and mandibular teeth were lighter on the right side (the side of surgery) while heavier contact was ensured on the left side of the patient. (Figure 3b,3c,3d). From the refractory model and the metal denture base for the maxillary arch (along with the female portion of the precision attachment) as well as the hollow bulb (along with the male part of precision attachment) were also fabricated and occlusal rims were built on the maxillary and mandibular denture bases. Prior to fabricating the metallic denture base, the position of the male and female components of the Dalbo attachments were identified. The hollow bulb was fabricated separately with the incorporated patrix part. The patrix parts were positioned 10 mm apart. The metallic denture base was fabricated using the refractory model. The matrix portion of the attachments were positioned in the wax pattern of the cast denture base (Figure 4a-4g). The wax-up of the trial denture was completed after which, the dentures were processed using heat cure compression moulding technique. The processed dentures were then polished and delivered to the patient. After the insertion of the dentures, the occlusal contacts were once again verified and all heavy contacts on the right side were adjusted to light occlusal contact while it was ensured that heavier contacts were present on the left side. (Figure 5a-5c).The facial appearance of the patient was improved drastically, along with esthetics and smile and a follow up of this technique was done periodically at regular intervals for upto 2 years. (Figure 6a-6b).
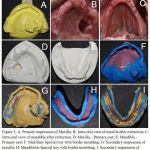 |
Figure 2: A: Primary impression of Maxilla; B: Intra-oral view of maxilla after extraction; C:
|
Intra-oral view of mandible after extraction; D: Maxilla – Primary cast; E: Mandible – Primary cast; F: Maxillary Special tray with border moulding; G: Secondary impression of maxilla; H: Mandibular Special tray with border moulding; I: Secondary impression of mandible;
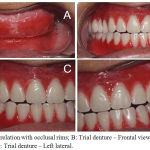 |
Figure 3: A: Jaw relation with occlusal rims; B: Trial denture – Frontal view; C: Trial denture – Right lateral; D: Trial denture – Left lateral
|
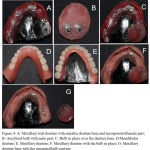 |
Figure 4: A: Maxillary trial denture with metallic denture base and incorporated female part; B: Acrylized bulb with male part; C:
|
Bulb in place over the denture base; D:Mandibular denture; E: Maxillary denture; F: Maxillary denture with the bulb in place; G: Maxillary denture base with the separated bulb portion
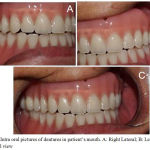 |
Figure 5: Intra oral pictures of dentures in patient’s mouth. A: Right Lateral; B: Left lateral; C: Frontal view
|
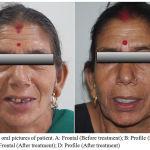 |
Figure 6: Extra oral pictures of patient. A: Frontal (Before treatment); B: Profile (Before treatment); C: Frontal (After treatment); D: Profile (After treatment)
|
Discussion
The conventional removable obturator framework design uses various clasps as retention components. Clasps have a low capacity for retention, and plastic deformation caused by cycles of insertion/removal may also lead to a rapid loss in retention. In some cases, precision attachments may be choice of treatment. Although major disadvantage of it is increase in cost and additional laboratory steps, alternatively nylon attachments are fairly economical, easily replaced, and reduce receptacle wear.7-11 The residual maxillary ridge affects the degree of obturator movement. The abutment teeth postion and its periodontal status are critical factors that contribute to the absorption of stress generated by functional movement of the obturator prosthesis and play an essential role in retaining and stabilizing the prosthesis. Resilient attachments accommodate obturator movement and reduce the stress on abutment teeth. If the defect is large and some or all of the remaining teeth are weak, extra coronal retainers should be used. The commonly used material for dentures is Poly(methylmethacrylate)(PMMA). However, acrylic has poor fracture resistance and is susceptible to fracture during mastication. The chances of fracture are high when the thickness of the denture base is thin.12-16 Additionally, PMMA based dentures undergo unavoidable dimensional changes during fabrication, such as thermal expansion on heating, contraction on cooling, and polymerization contraction. However, to a certain extent, these contractions may be compensated by expansion because of water sorption.8 An additional source of dimensional change occurring in the conventional compression molding technique is the flash which is encountered during packing of the mould space. Few Authors suggested the use of cobalt-chromium bases in maxillary dentures to overcome the limitations of acrylic denture bases.9 Habib, in his study on different denture base materials, reported that Co-Cr denture base was more dimensionally stable than acrylic denture bases at normal oral temperatures.10 Belfiglio11 enumerated some of the advantages of using metallic denture bases. A few of these are (1) more retentive,(2) have less occlusal discrepancy, (3) cause fewer sore spots, (4) have a reduced incidence of fracture, (5) feel better to the patient, (6) are better thermal conductors, (7) have a thinner palate that aids speech. The patient was satisfied with the outcome of the prosthesis. This prosthesis met several of the treatment objectives: Closure of the oro/nasal communication; facilitate easy cleaning of the bulb portion; good retention of the two piece obturator; improvement in phonetics and masticatory function; replaced the missing teeth and; improved esthetics of the patient.
Conclusion
Rehabilitating patients with a maxillofacial prosthesis requires a good knowledge about material science, the anatomy of the defective area as well as skill of the prosthodontist as well as the laboratory technician. Most importantly good communication between the lab and the prosthodontist is also essential for the successful outcome of the prosthesis. Considering the socio economic status and the clinical condition of the patient, it was decided to fabricate the precision attachment retained palatal obturator. The use of metallic denture base in the maxillary denture further lightened the prosthesis and increased not only the retention of the denture but also the comfort of the patient.
Acknowledgement
The authors greatly acknowledge the institution for their great support.
Sources of Support
The work was supported by the Department of Prosthodontics, Saveetha Dental College And Hospital, Saveetha University, Chennai, India.
Conflict of Interest
Authors declare that they have no conflict of interest.
References
- Jain A.R, Philip J.M, Ariga P. Attachment-retained Unilateral Distal Extension (Kennedy’s Class II Modification I) Cast Partial Denture. Int J Prosthodont Restor Dent. 2012;2(3):101-107.
CrossRef - R et al. Prosthodontic Rehabilitation of Cantor and Curtis Class III Mandibular Defect Using Cast Partial Denture- A Case Report .J. Pharm. Sci. & Res. 2016;8(6):461-463.
- Jain A.R. A Prosthetic Alternative Treatment for Severe Anterior Ridge Defect using Fixed Removable Partial Denture Andrew’s Bar System. World J Dent. 2013;4(4):282-285.
CrossRef - Jain R, Mathew J, Philip R,Pradeep C.J, Krishnan V and Narasimman M. “Cast Retainer Hollow Bulb Obturator for a Maxillary Defect -A Case Report.” International Journal of Dental Sciences and Research. 2014;2(6):164-167.
- Beumer J, Curtis T, Marunick M. Maxillofacial rehabilitation: prosthodontic and surgical considerations. St Louis: Ishiyaku EuroAmerica. Inc. 1996;240-285.
- Lapointe H.J, Lampe H.B, Taylor M. Comparison of maxillectomy patients with immediate versus delayed obturator prosthesis placement. .J. Otolaryngol. 1996;25:308-312.
- Lang B.R, Bruce R.A. Presurgical maxillectomy prosthesis. J. Prosthet Dent. 1967;17:613-619.
CrossRef - Aramany M.A. Basic principles of obturator design for partially edentulous patients. Part I: Classification. J. prosthet dent. 2001;86(6): 559-561.
CrossRef - Aramany M.A. Basic principles of obturator design for partially edentulous patients. Part II: Design principles. J prosthet dent. 2001;86(6):562-568.
CrossRef - Gregory R.P, Greggory E.T, and Arthur O.R. Prosthodontic principles in the framework design of maxillary obturator prostheses. J. Prosthet Dent. 2005;93:405-411.
CrossRef - Shaker K.T. A simplified technique for construction of an interim obturator for a bilateral total maxillectomy defect. Int J Prosthodont. 2000;13:166-168.
- Grossmann Y and Savion I. The use of a light polymerized resin-based obturator for the treatment of the maxillofacial patient. J. Prosthet Dent 2005;94:289-292.
CrossRef - Mark A.P. Conventional prosthetic rehabilitation after free flap reconstruction of a maxillectomy defect: A clinical report. J. Prosthet Dent. 2001;86:578-581.
CrossRef - Won-suck O and Roumanas E.D. Optimization of Maxillary Obturator Thickness Using a Double-Processing Technique. Journal of Prosthodontics. 2008;17:60-63.
- Parel S.M, Fuente L.H. Single visit hollow obturators for edentulous patients. J. Prosthet Dent. 1978;40(4):426-9.
CrossRef - Elliott D. J. The hollow bulb obturator: Its fabrication using one denture flask. Quintessence Dent Technol. 1983;7(1):13-4.







